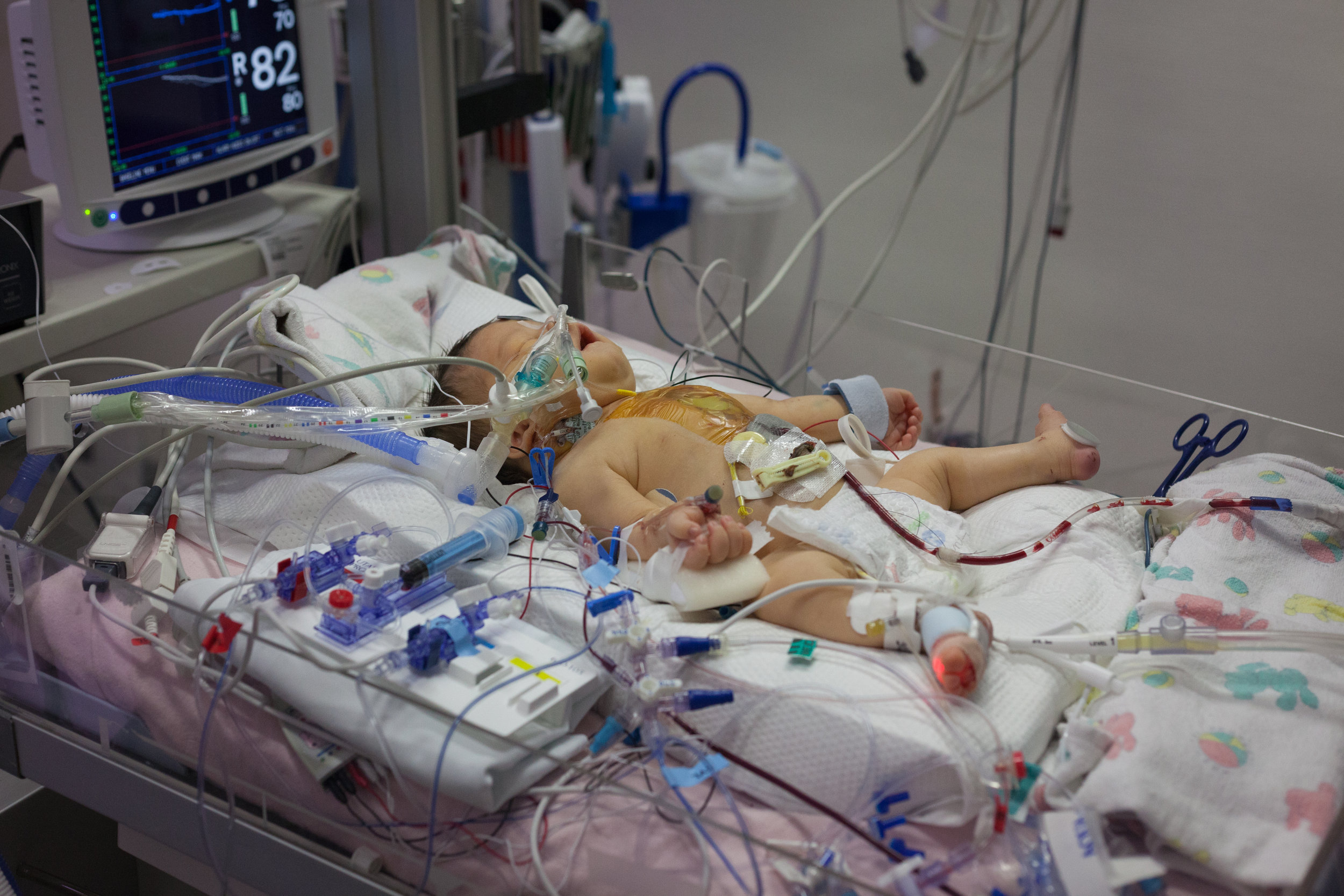
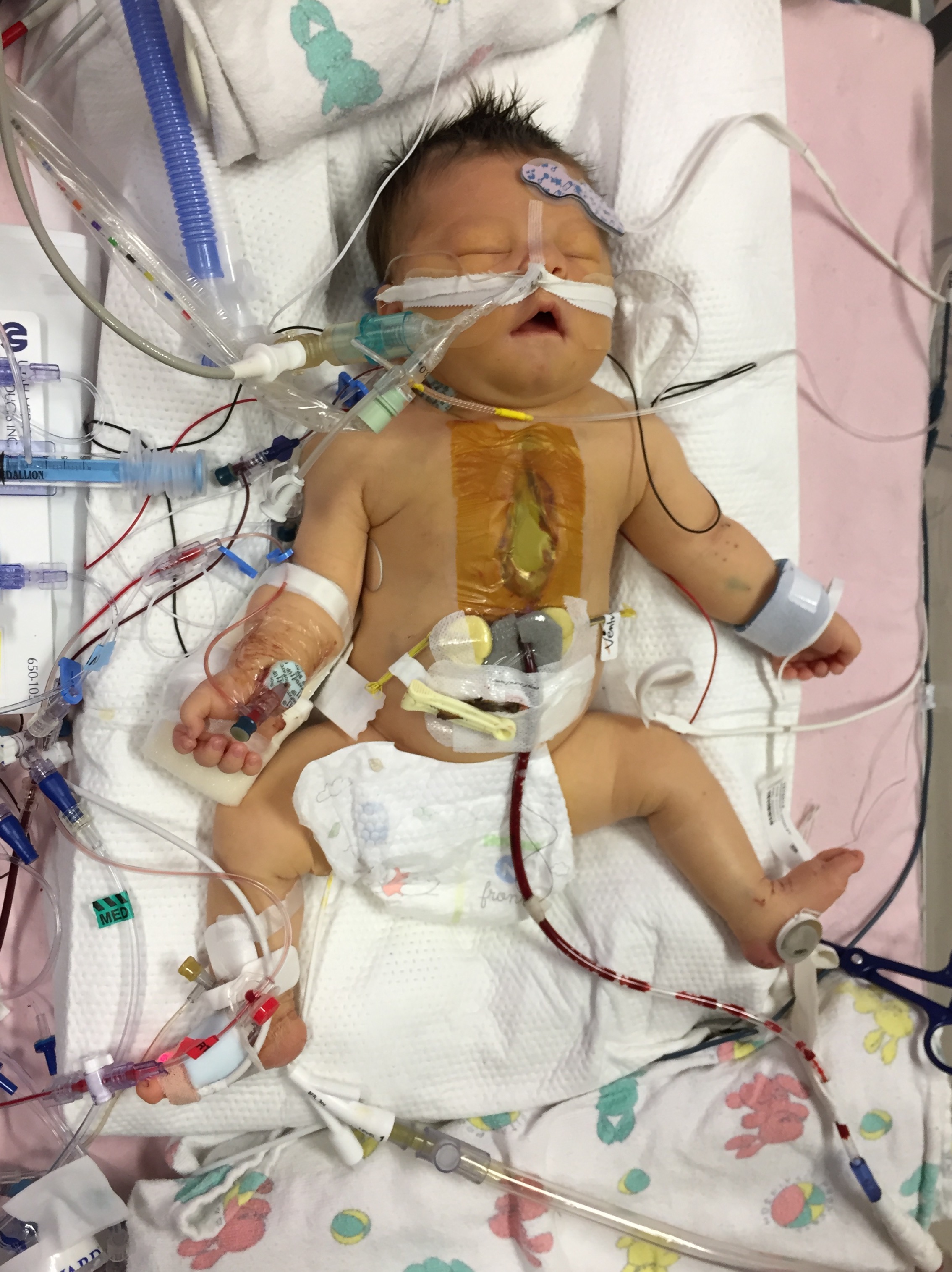
An update about our child with truncus arteriosus, a rare form of congenital heart disease.
Long Night and a Short Day.
Possible Infection
Shirley had a long and eventful night. We were up until midnight and decided to stay the night here sensing that it was going to be an active one. Around 3am Shirley spiked another fever just over 101. They pulled all the stops this time. It was pretty much non-stop activity from 3 to 8am. Shirley wasn't the most cooperative and just getting an IV placed took a considerable amount of time. Two nurses and a few pokes later they were finally able to get into a vein that would draw. They swabbed her nose and throat and tried to place a catheter for a urine sample. The urine sample was also very hard to come by. They wanted to start a broad spectrum antibiotic at 6am but didn't want to begin until after they had urine. One more try for a catheter at 8am worked out well and got enough to send to the lab. Her nose and throat swabs came back negative but her blood did show very high levels of c-reactive protein (CRP) which is an inflammation marker and also a good indicator of a possible infection. Still waiting on the full blood results but the initial urine sample came back positive for leukocytes and protein. Lets hope that it is as simple as a UTI. The complete urine and blood results will hopefully single something out. Until then, she is on a very broad spectrum antibiotic that will be changed out for something more specific once her results are in. Thanks for praying for our little girl.
Short Day
I wrote the first half of this post at 10am, it's now 9pm and I'm going to try to finish. Shirley responded almost immediately to the antibiotics. Her fever subsided and she slept the majority of the day. She was pretty much crying for 6 straight hours this morning so you can imagine how exhausted she was. There was a slim chance that she could have had an infection in her heart tissue and an echo revealed nothing. There was also the possibility that her heart was failing which could cause the temp and tachycardia but the echo showed no signs of decreased function beyond what she already has. Although her complete labs are not back yet they are pretty confident that she has a UTI and that the first dose of antibiotics hit it pretty hard. They are going to continue antibiotics for 48 hours.
Family and Friends
We almost canceled Shirley's visitors today but her Uncle John, Aunt Tish and baby cousin Lillie Belle traveled from San Diego to see her. She was either going to get worse from her infection or get better and we thought either way they should just come see the little girl. Some family friends also stopped by to say "hello." We had a few games of cribbage, doted on Shirley, and ate dinner.
Scare
Last night was scary but the nurses and doctors taking care of Shirley are amazing. They also let me be involved in almost every situation. I had a role throughout the entire night/morning and didn't want to be anywhere but next to Shirley. It was very difficult but it was also another good experience. There was nothing we could do to actually make Shirley better so we prayed... a lot. Last night and this morning proved to be the most difficult day for me. Surgery was a difficult time but it wasn't as scary. Surgery seemed so much more controlled and the outcomes so well explained. Last night was just tense, waiting on answers, and praying that it wasn't a worst case scenario. The sadness of thinking that her best days are behind us and that it was possible that these events could be the end. Those are the scariest thoughts I've ever had and it felt like a heavy weight on my chest. It's strange to me, but for whatever reason when I think of losing Shirley what scares me the most is not being able to look her into her eyes and tell her I love her. Her eyes have such a unique grip on me that I can't bear the thought of not being able to stare into them.
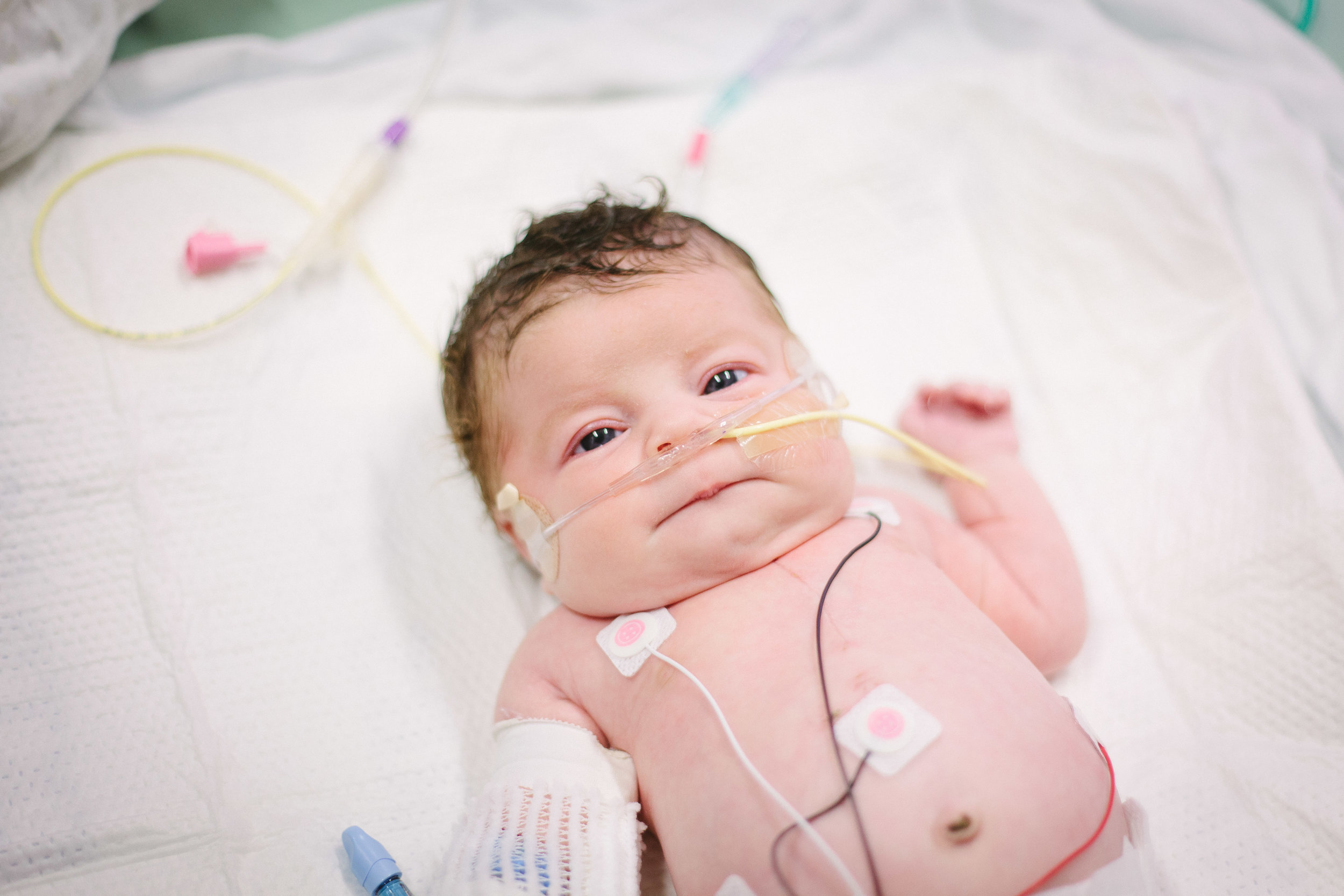
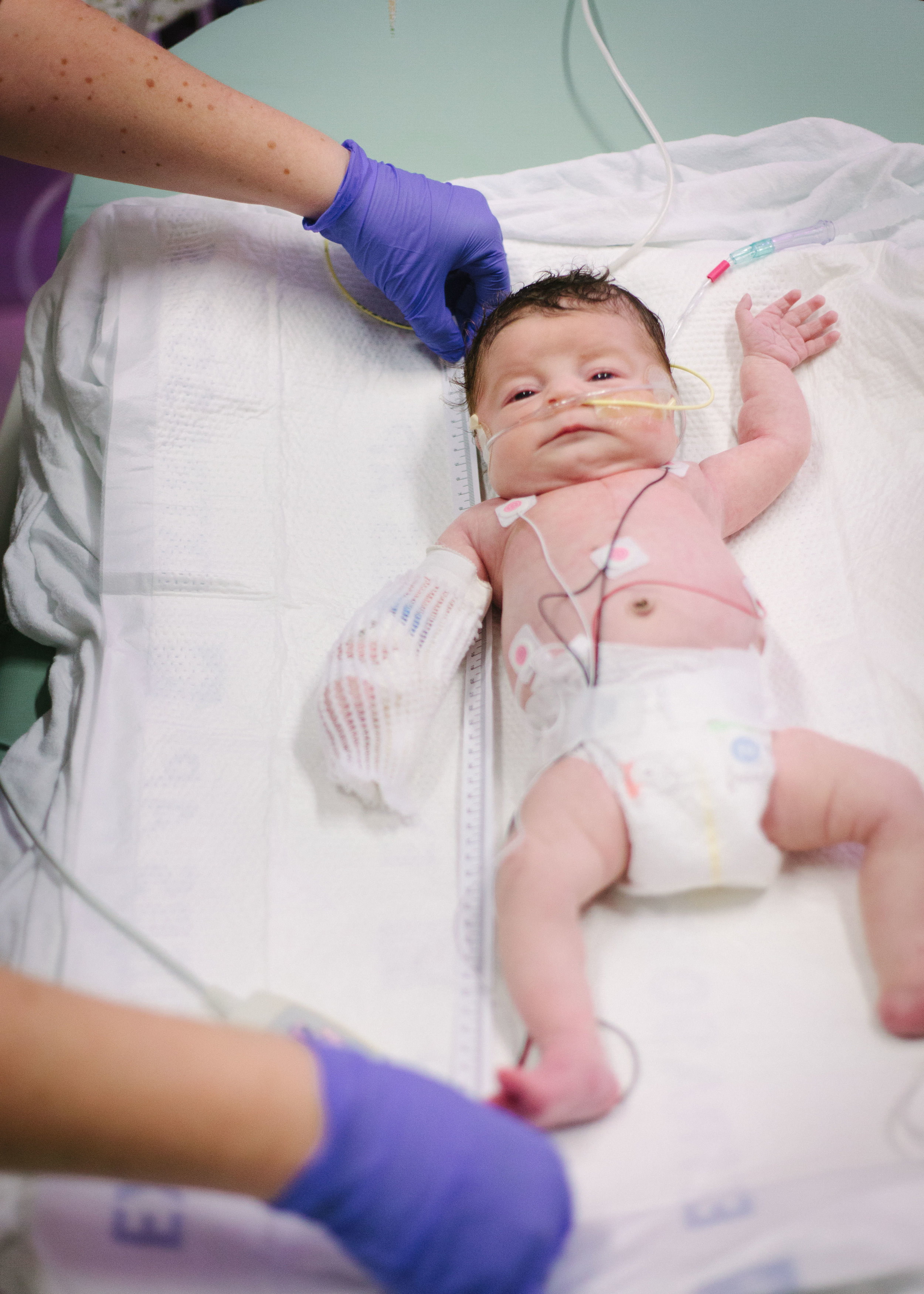
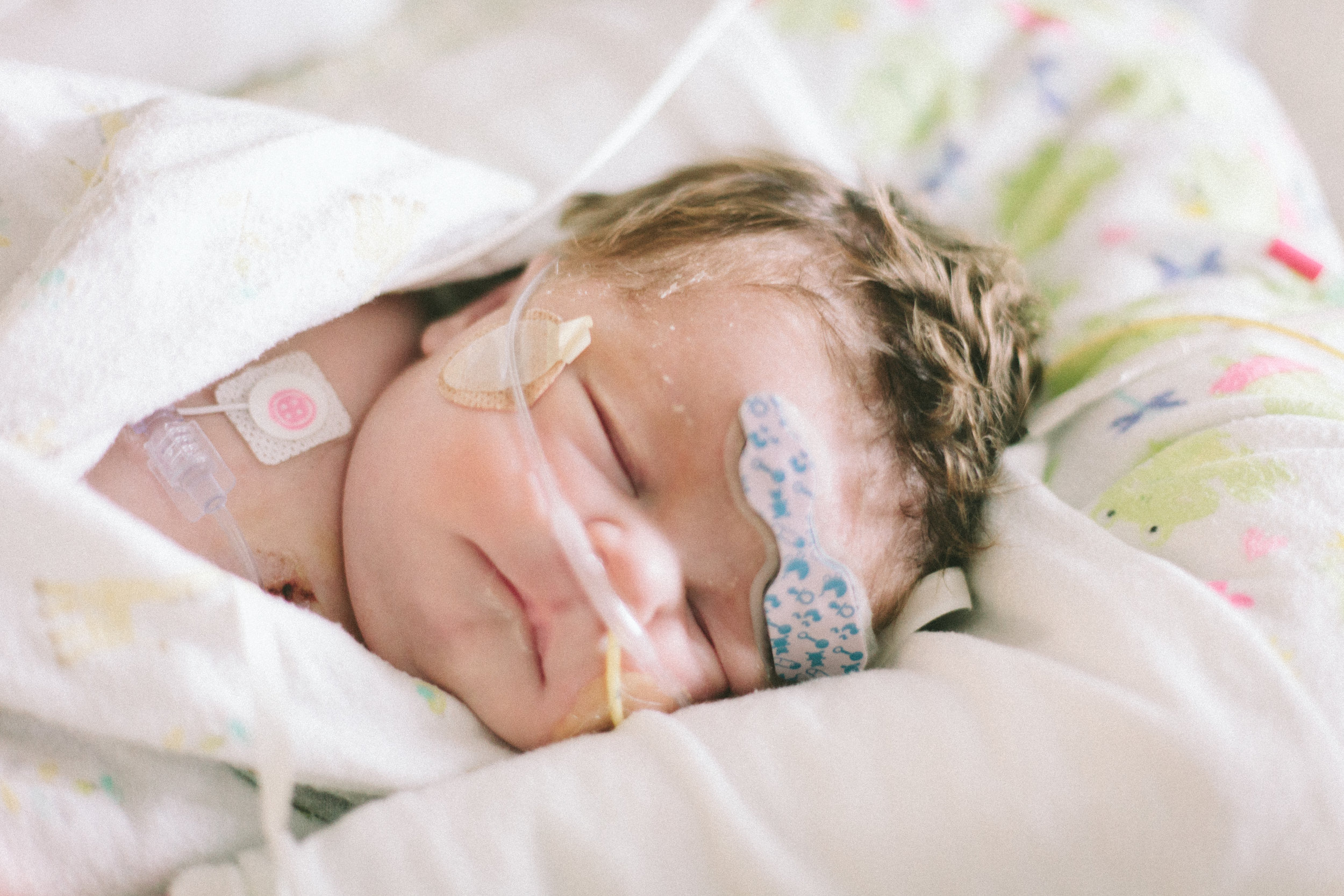
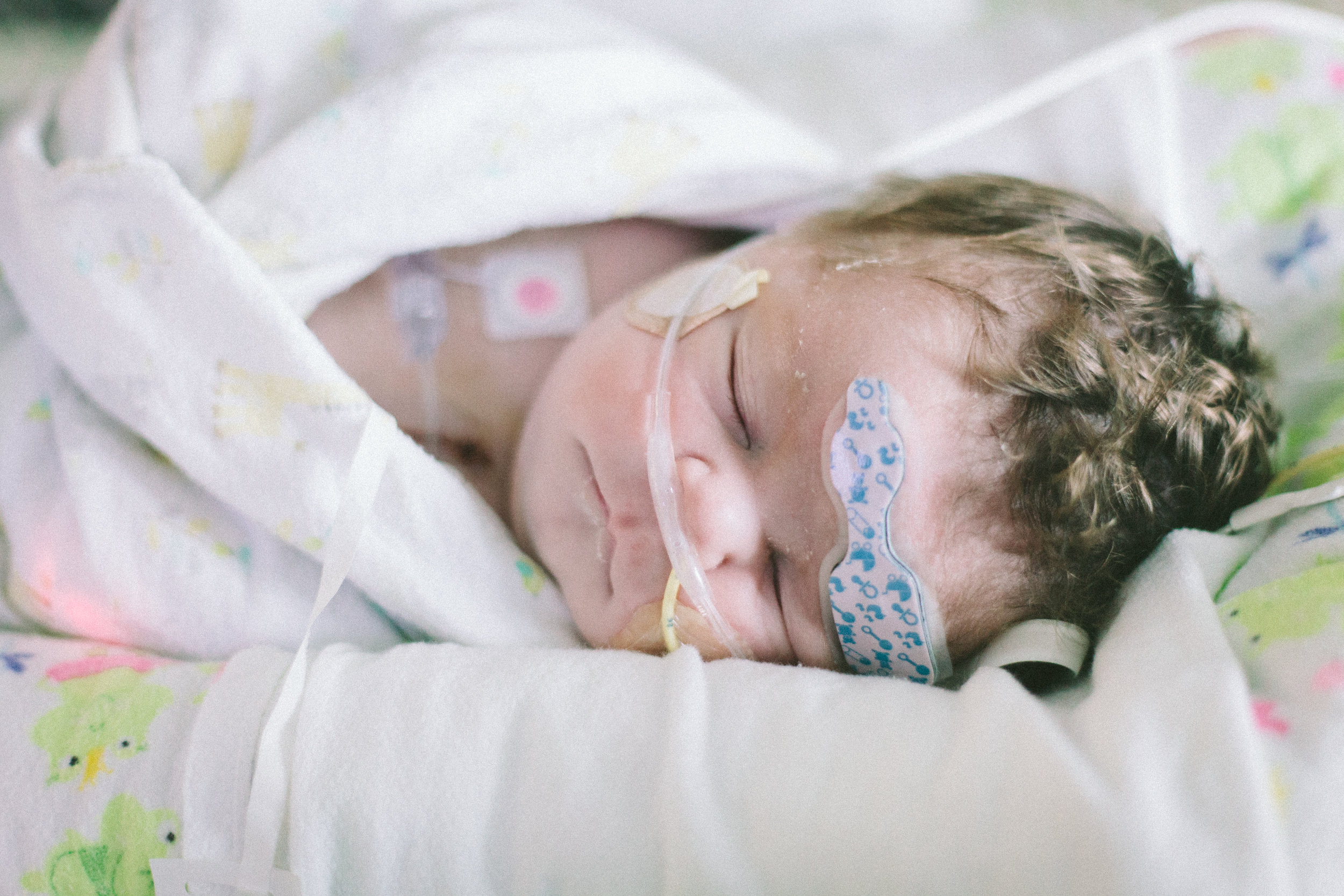
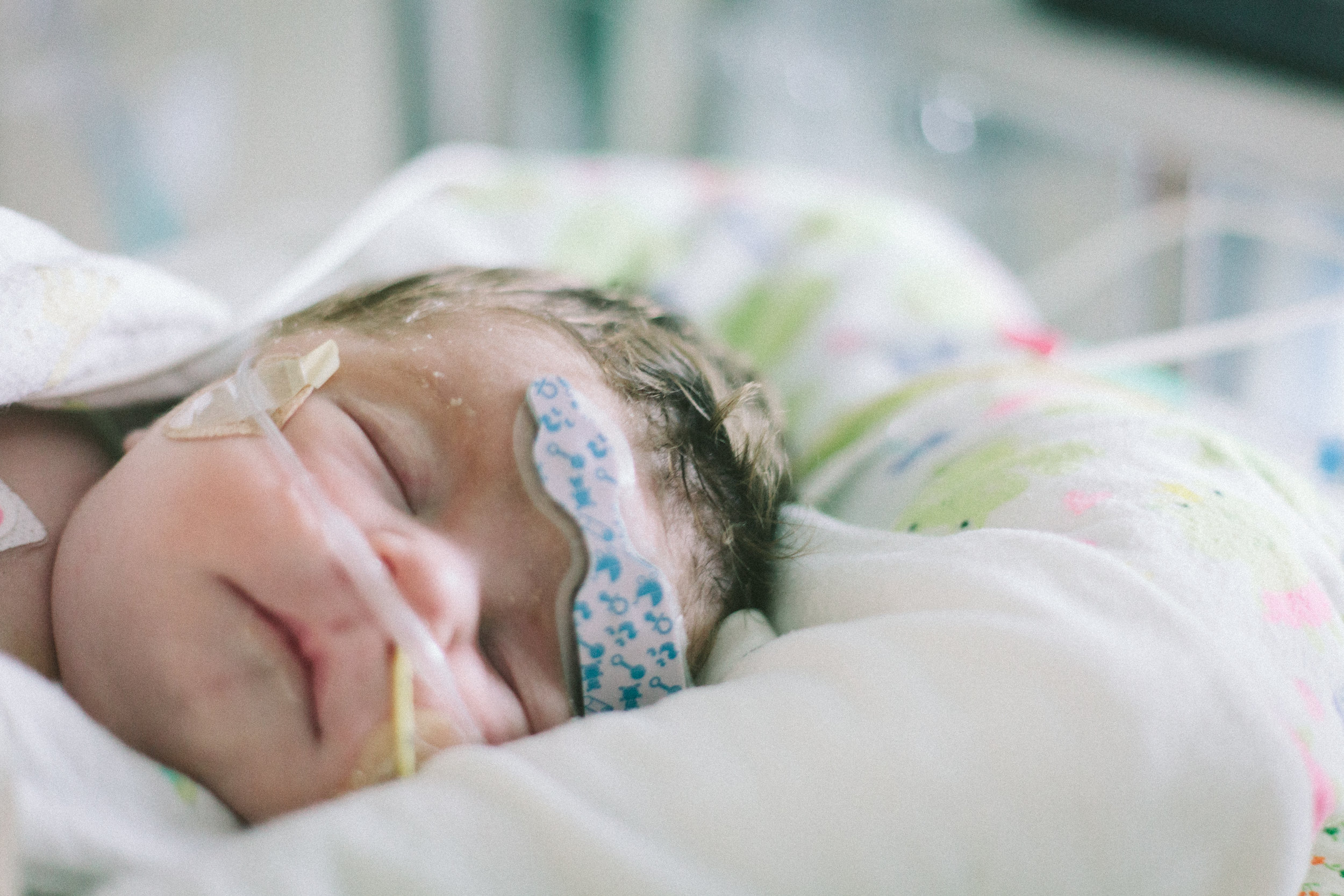
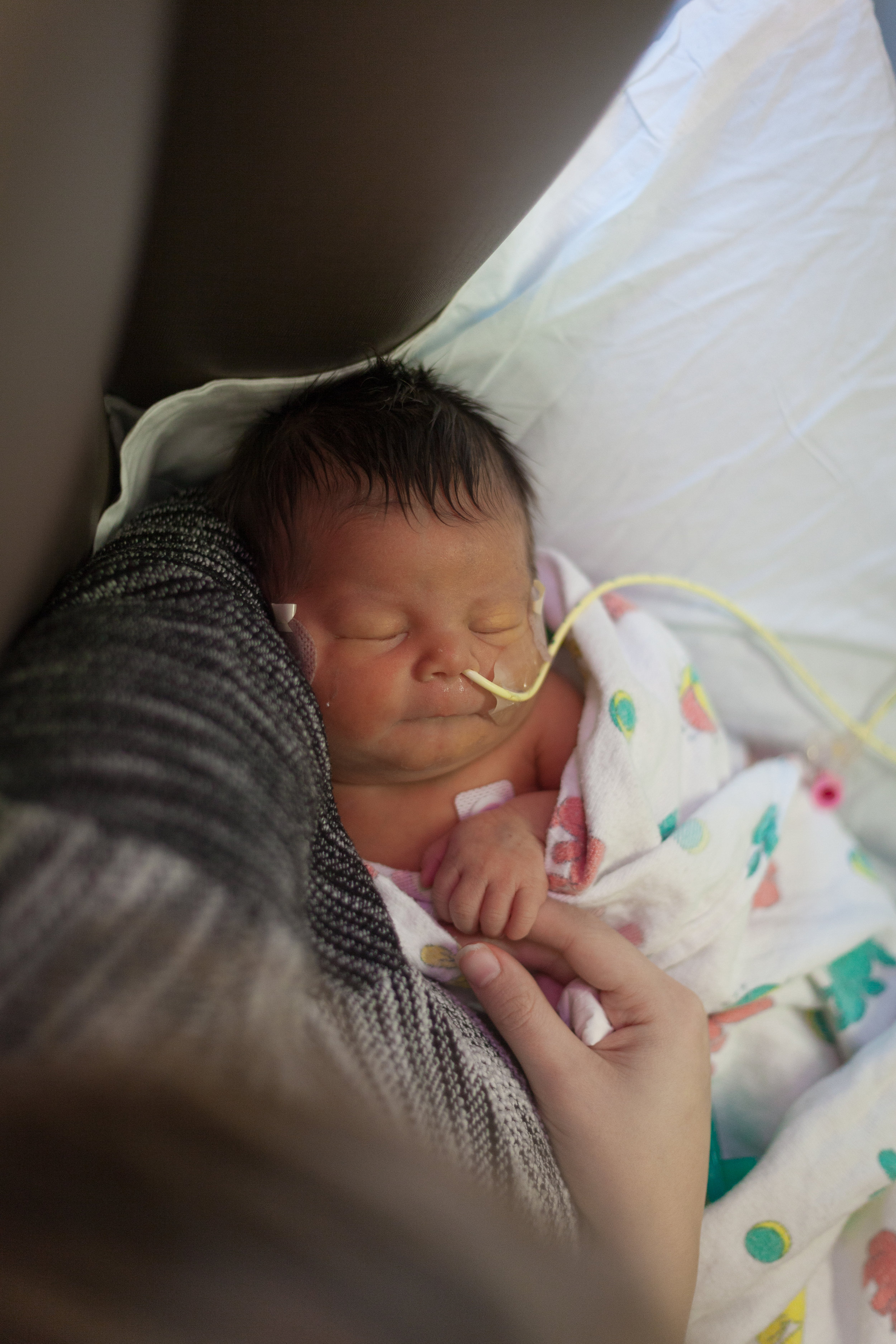
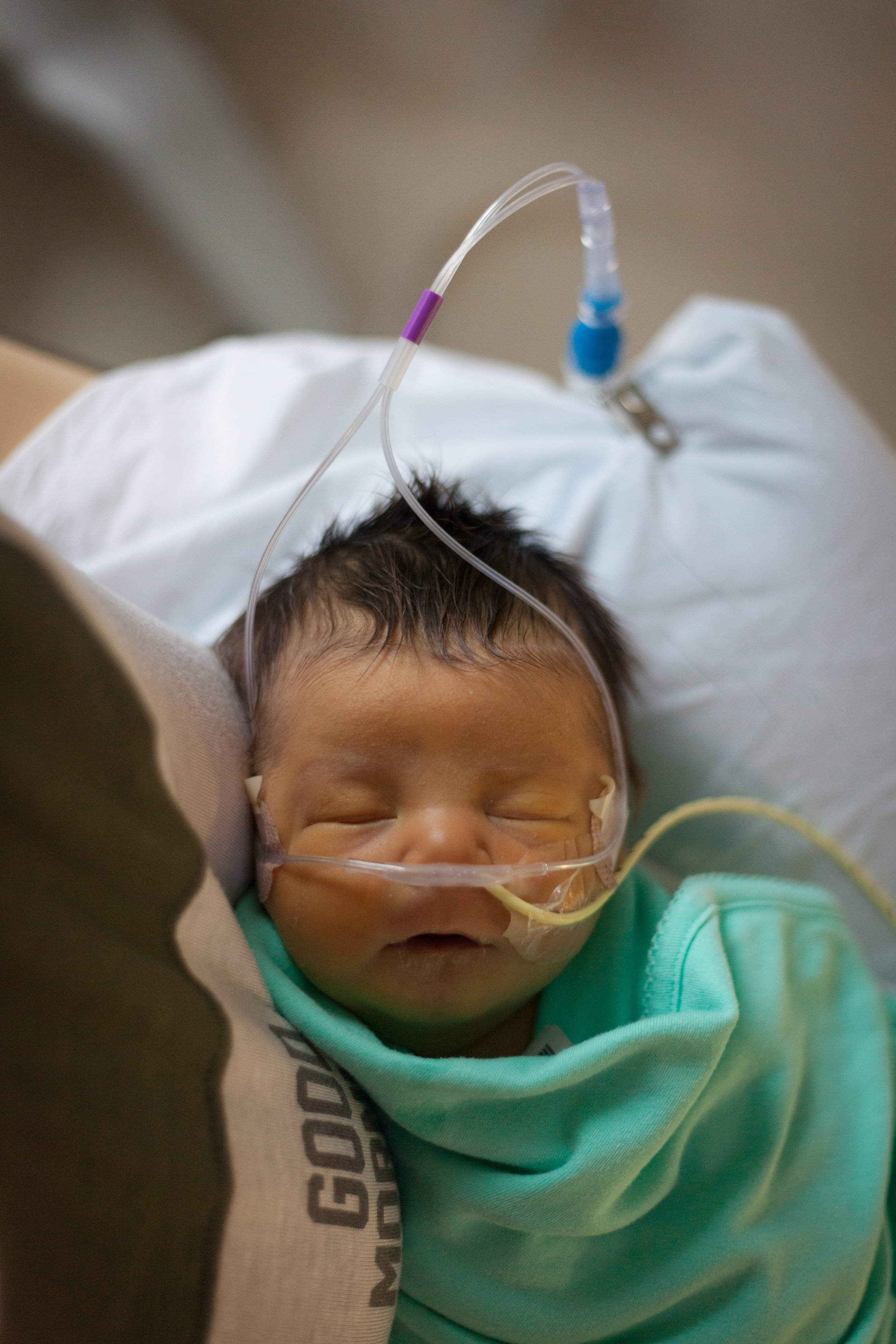
As I write this now Shirley is sleeping peacefully in her bed as if nothing ever happened and we went through the day almost as if last night was just a very bad dream.
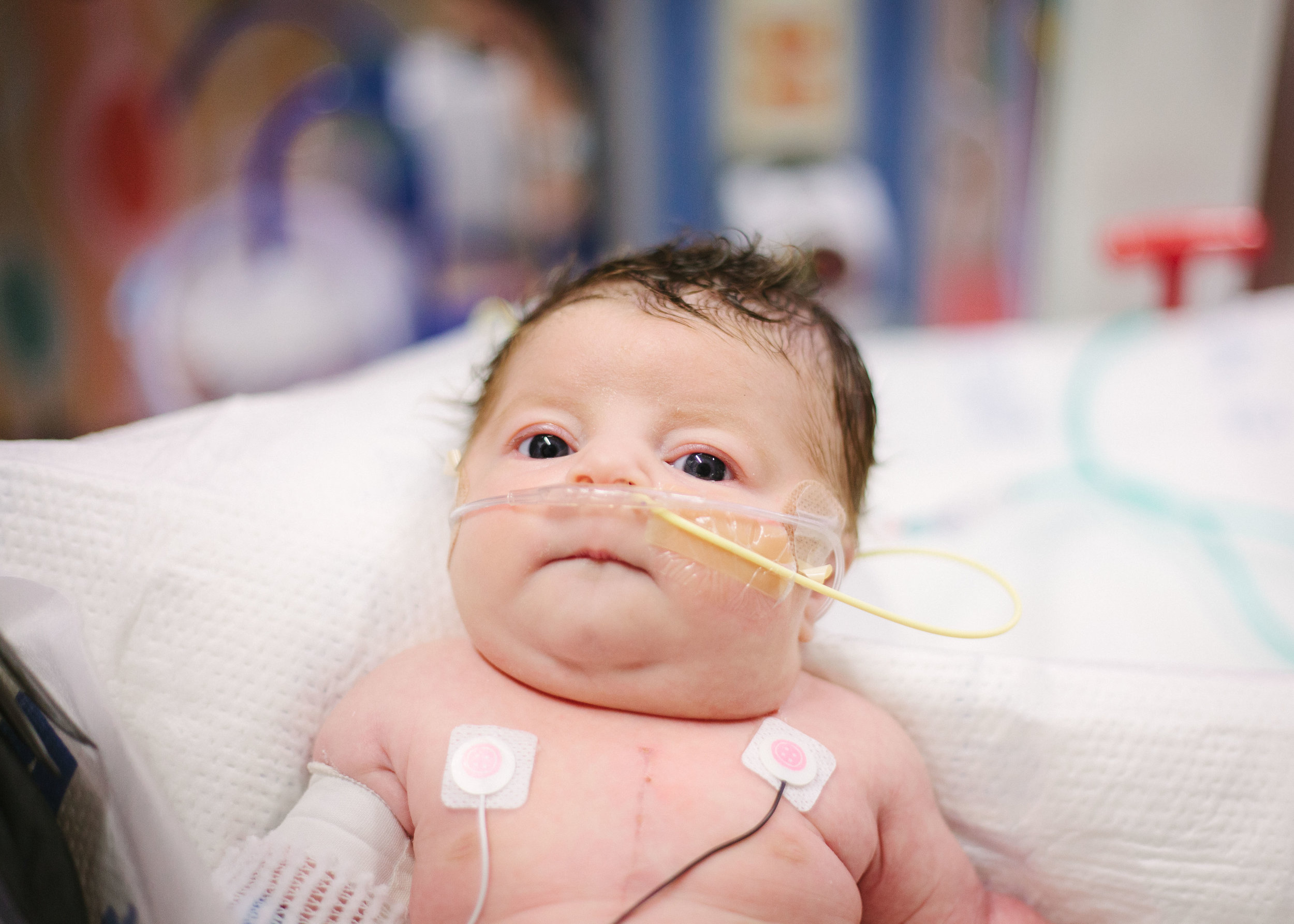
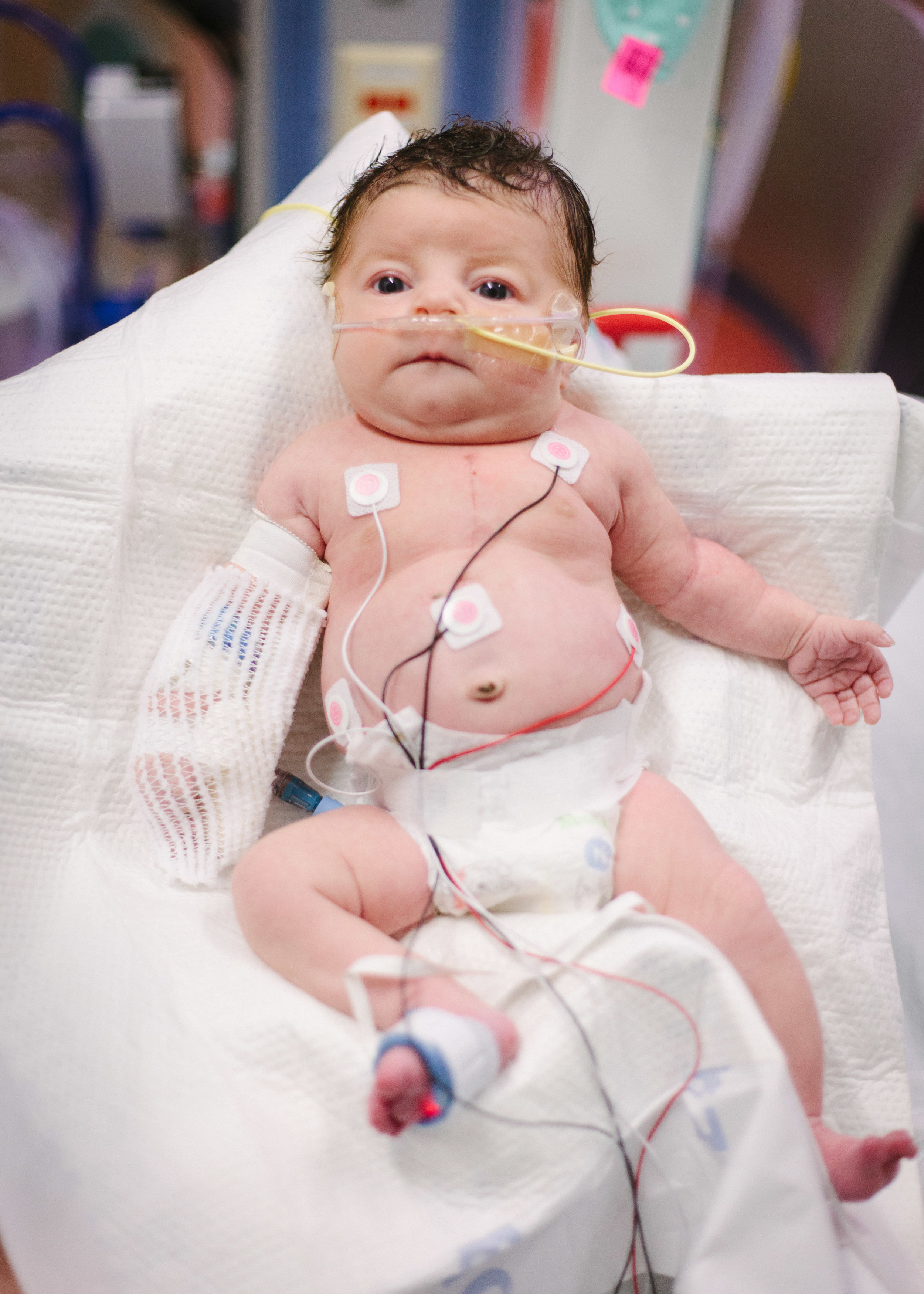
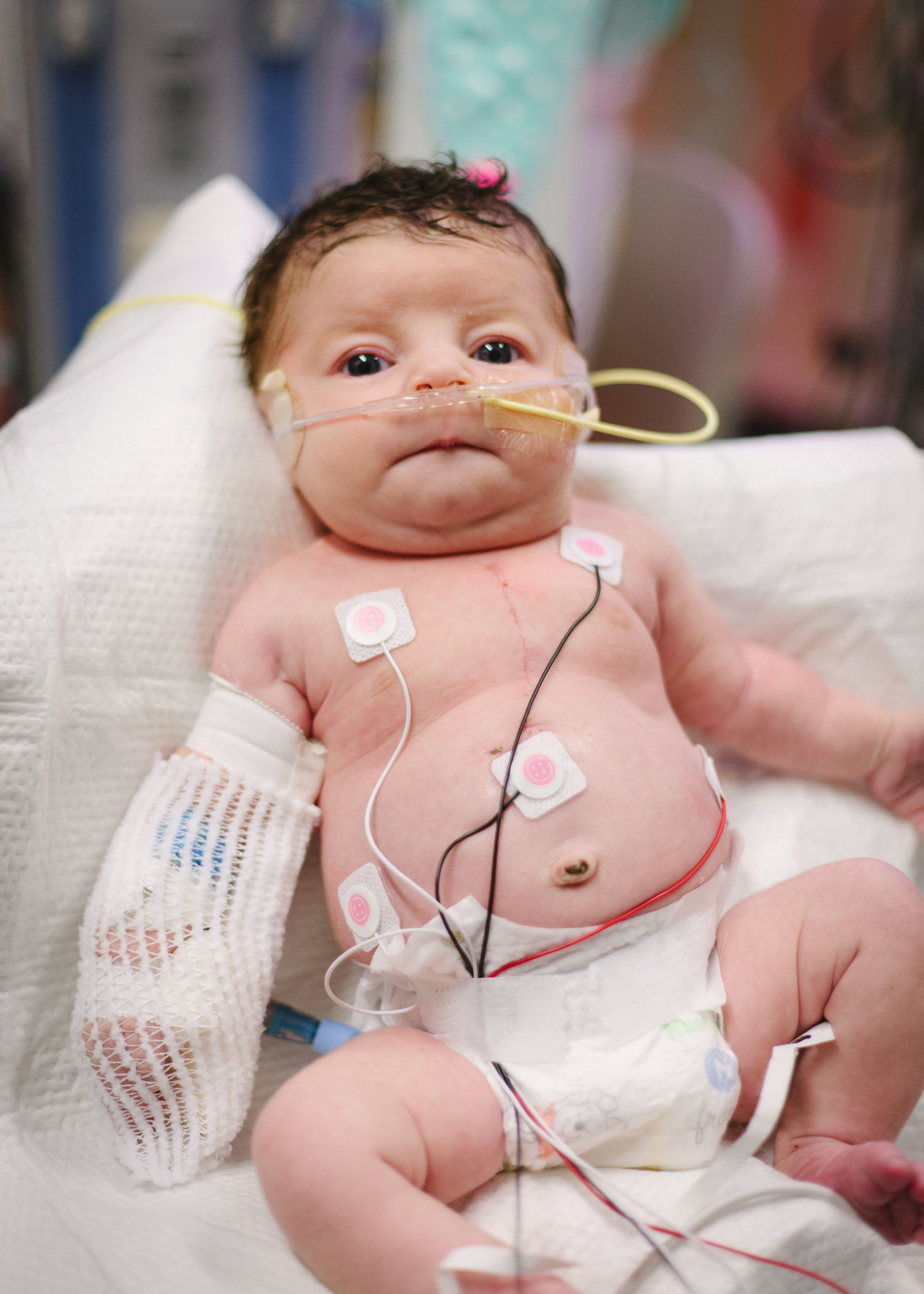
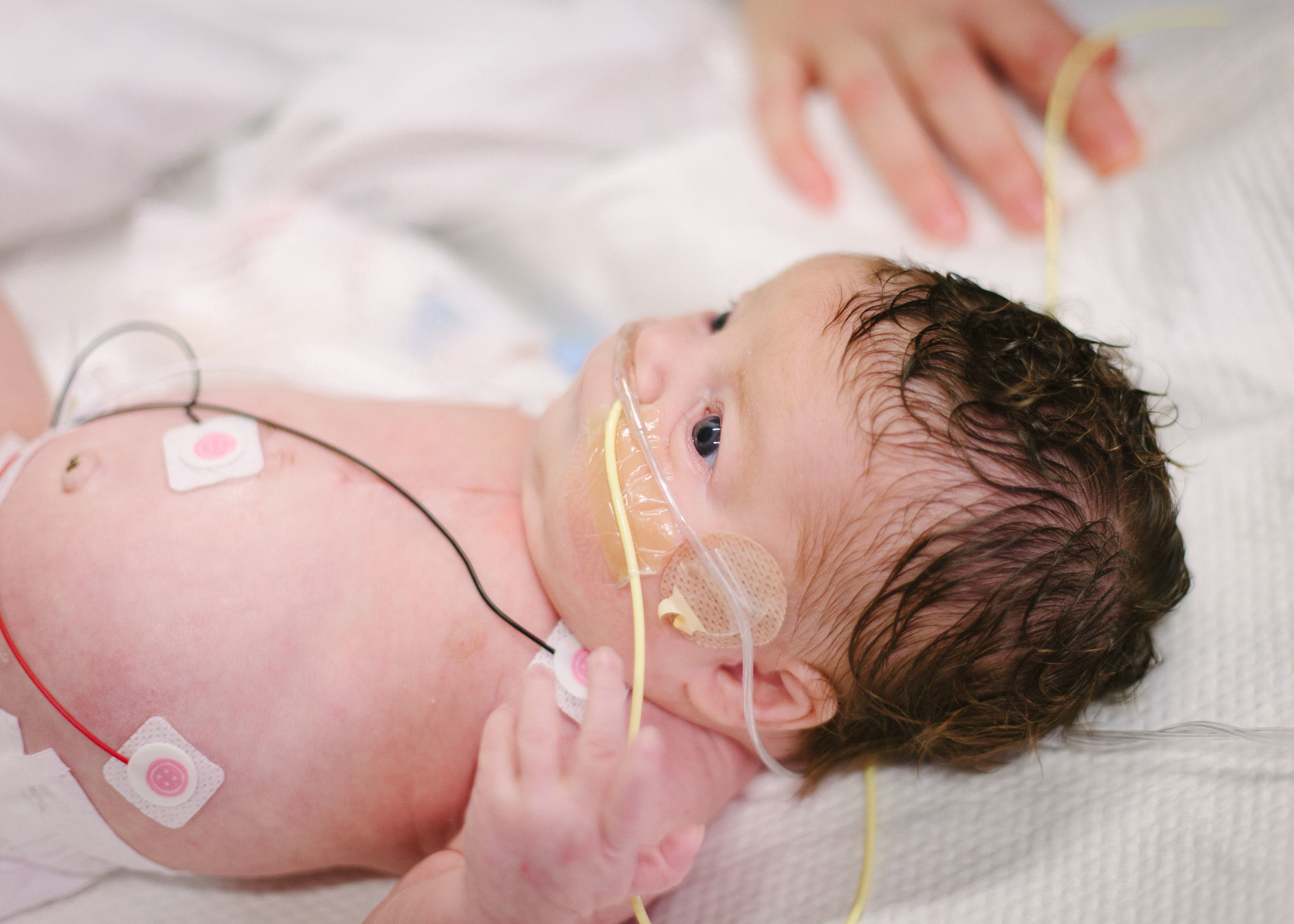
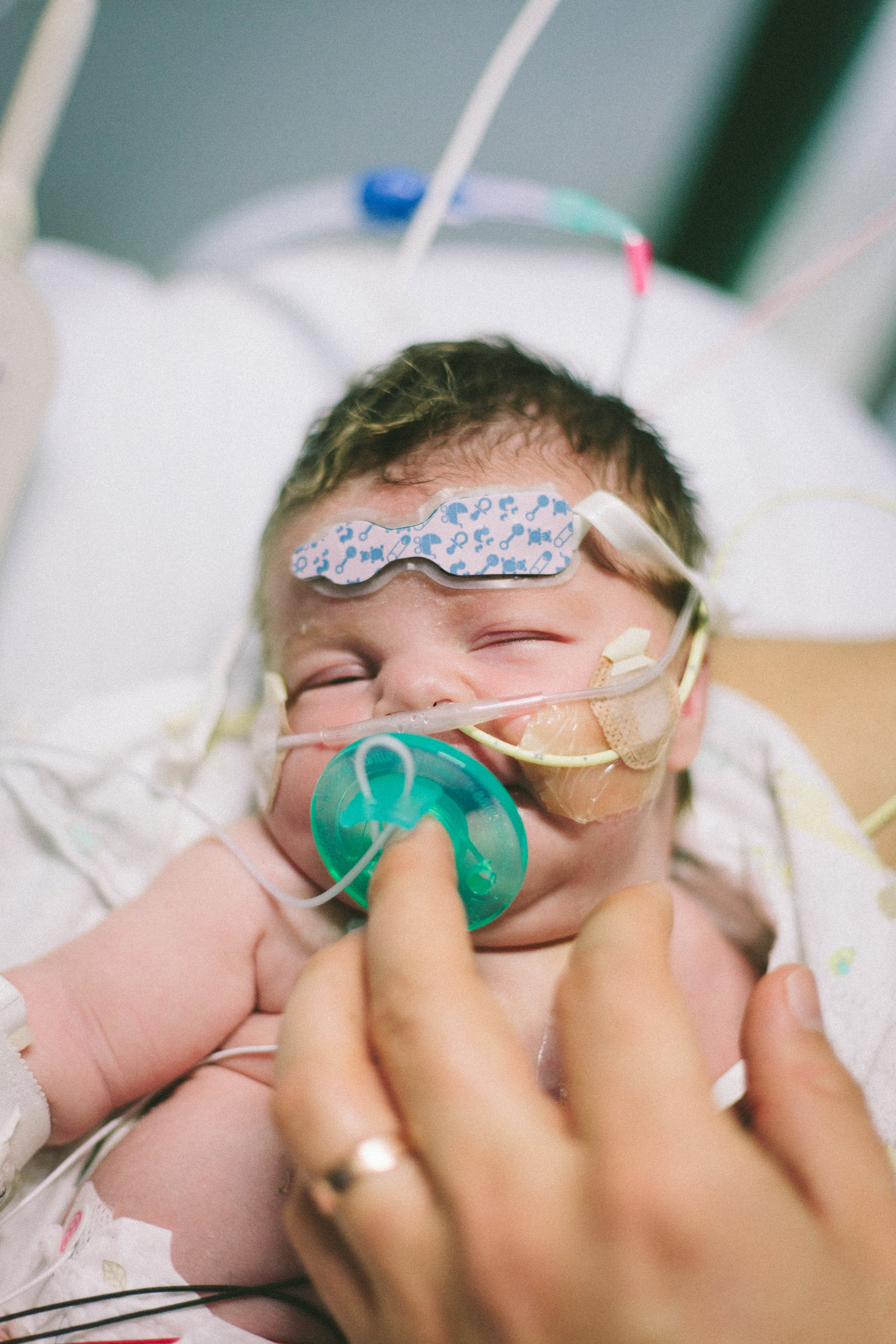
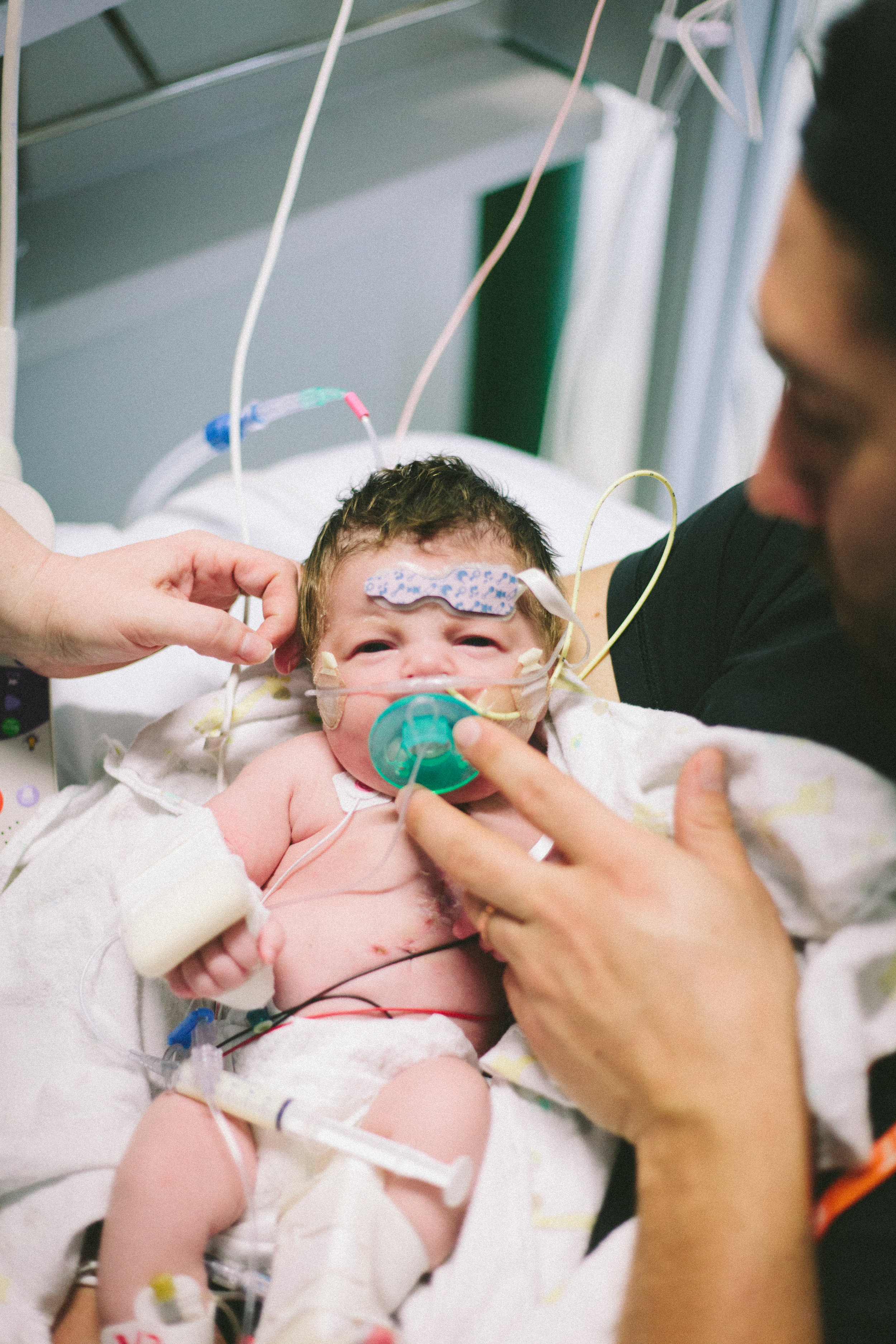
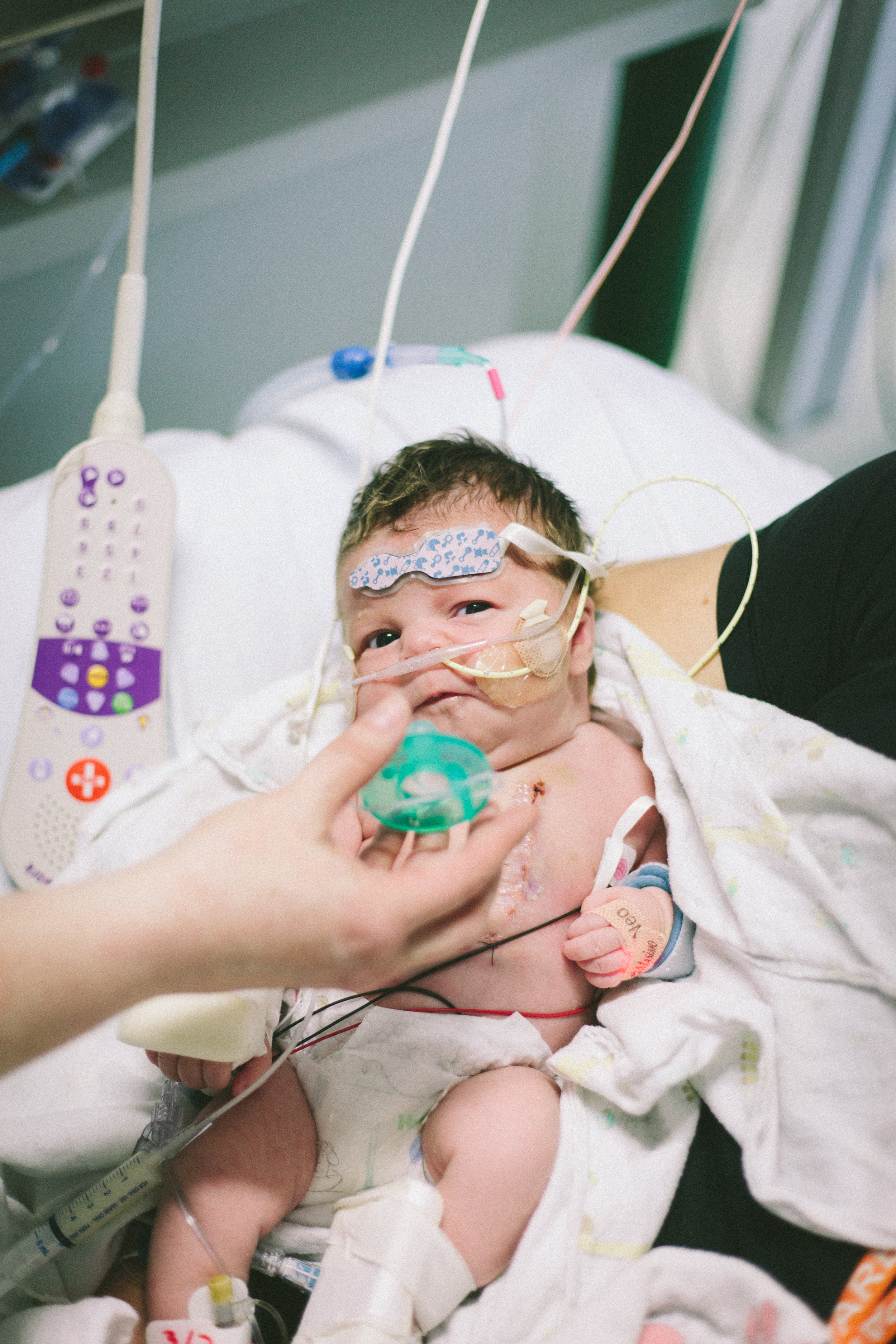
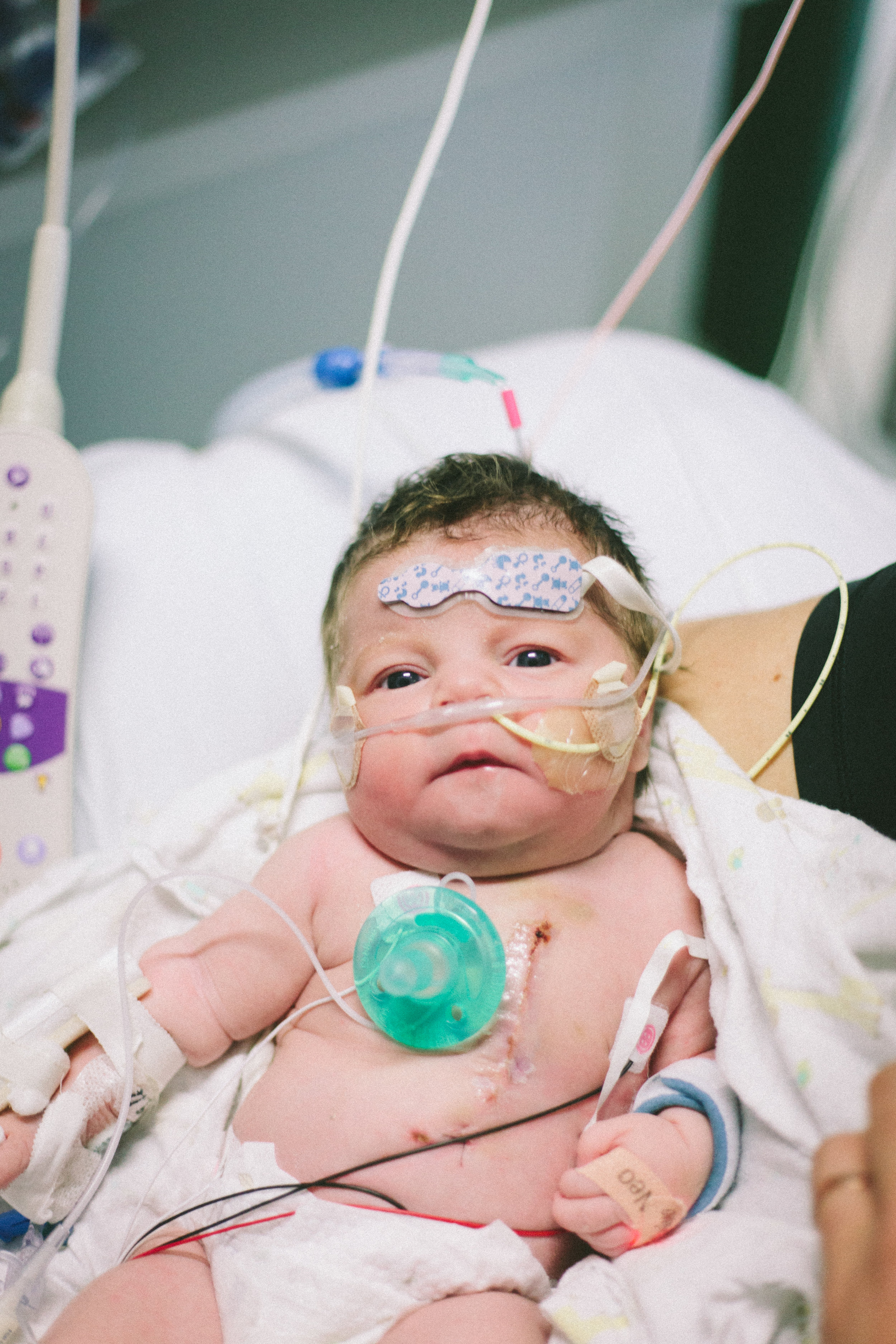
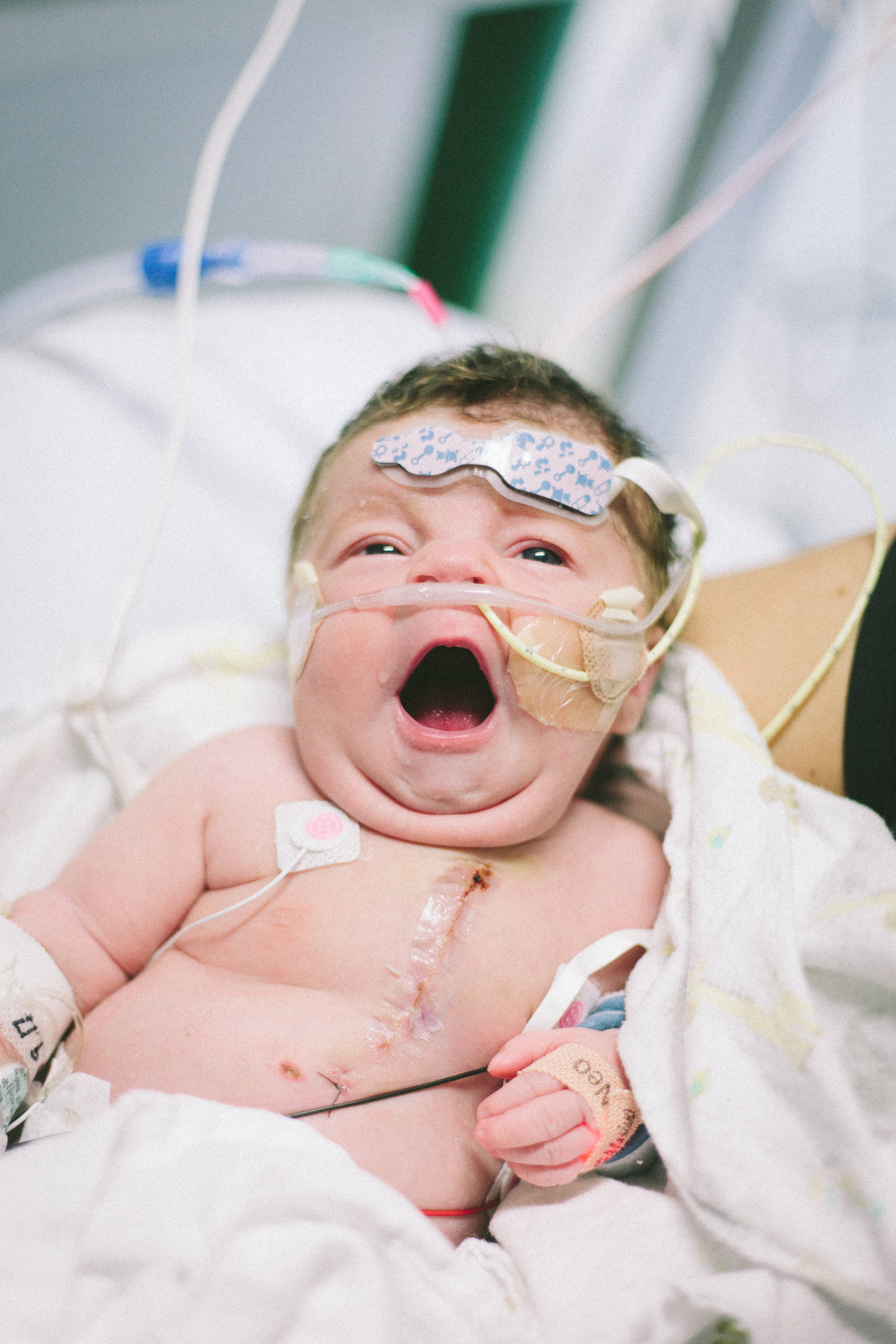
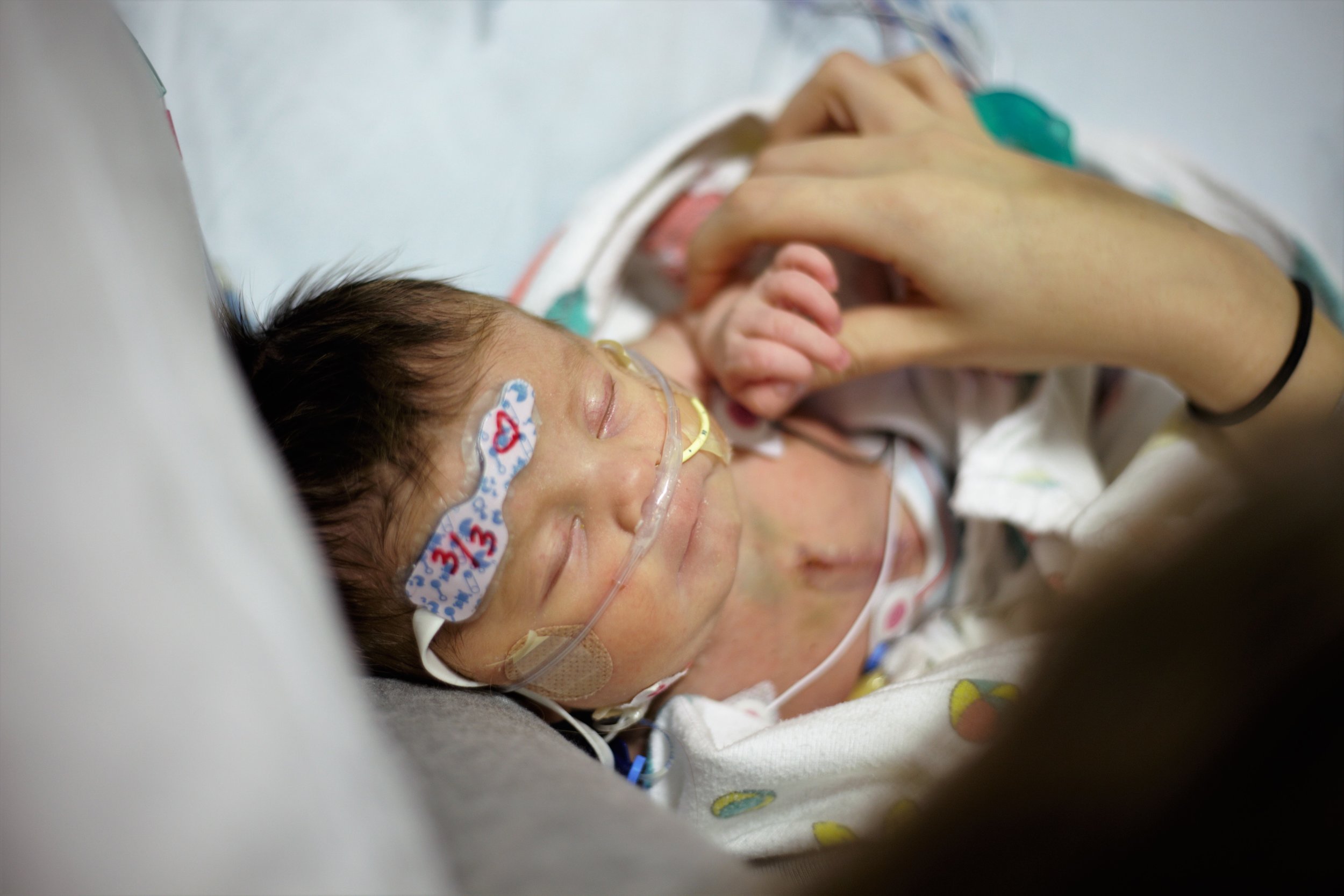
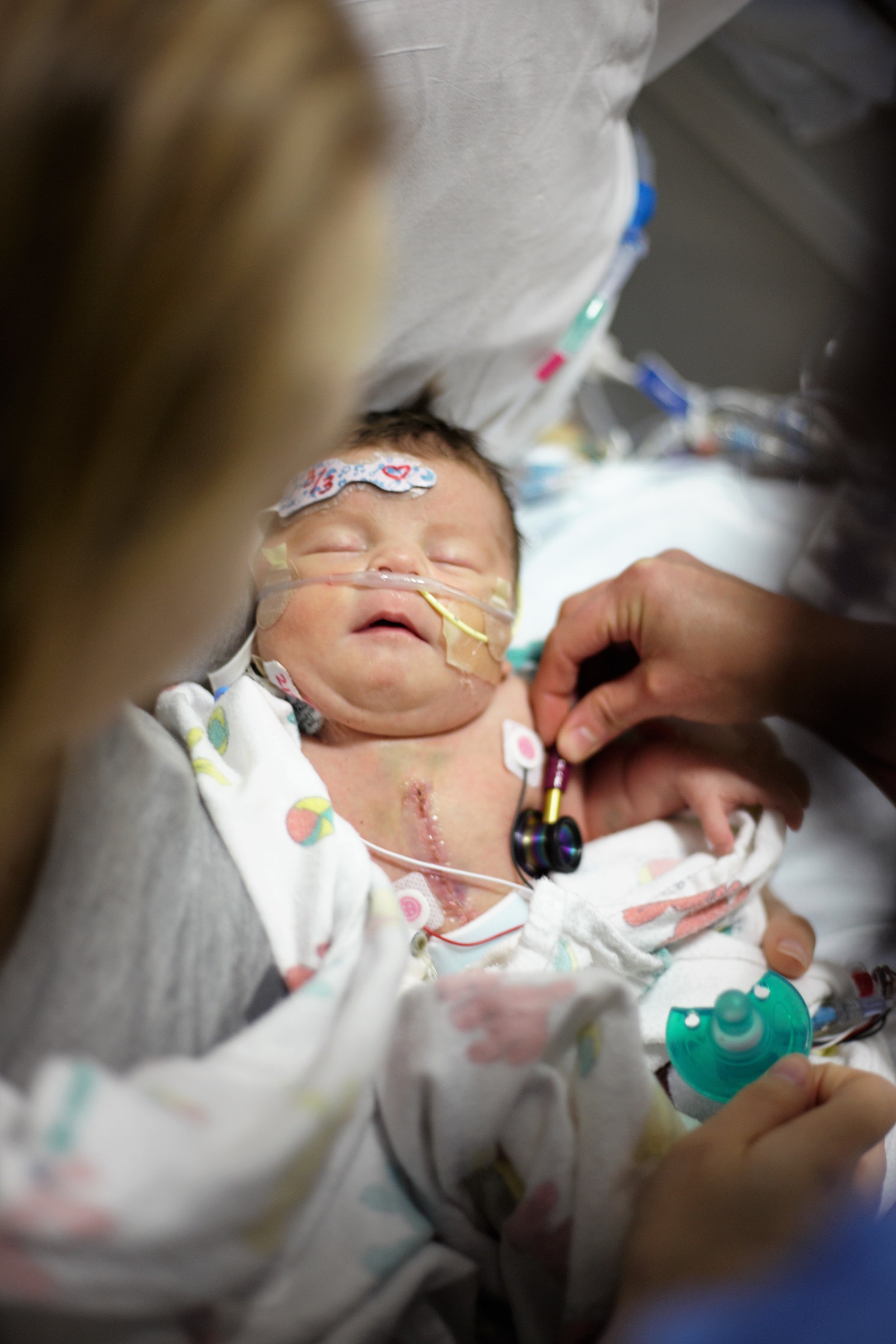
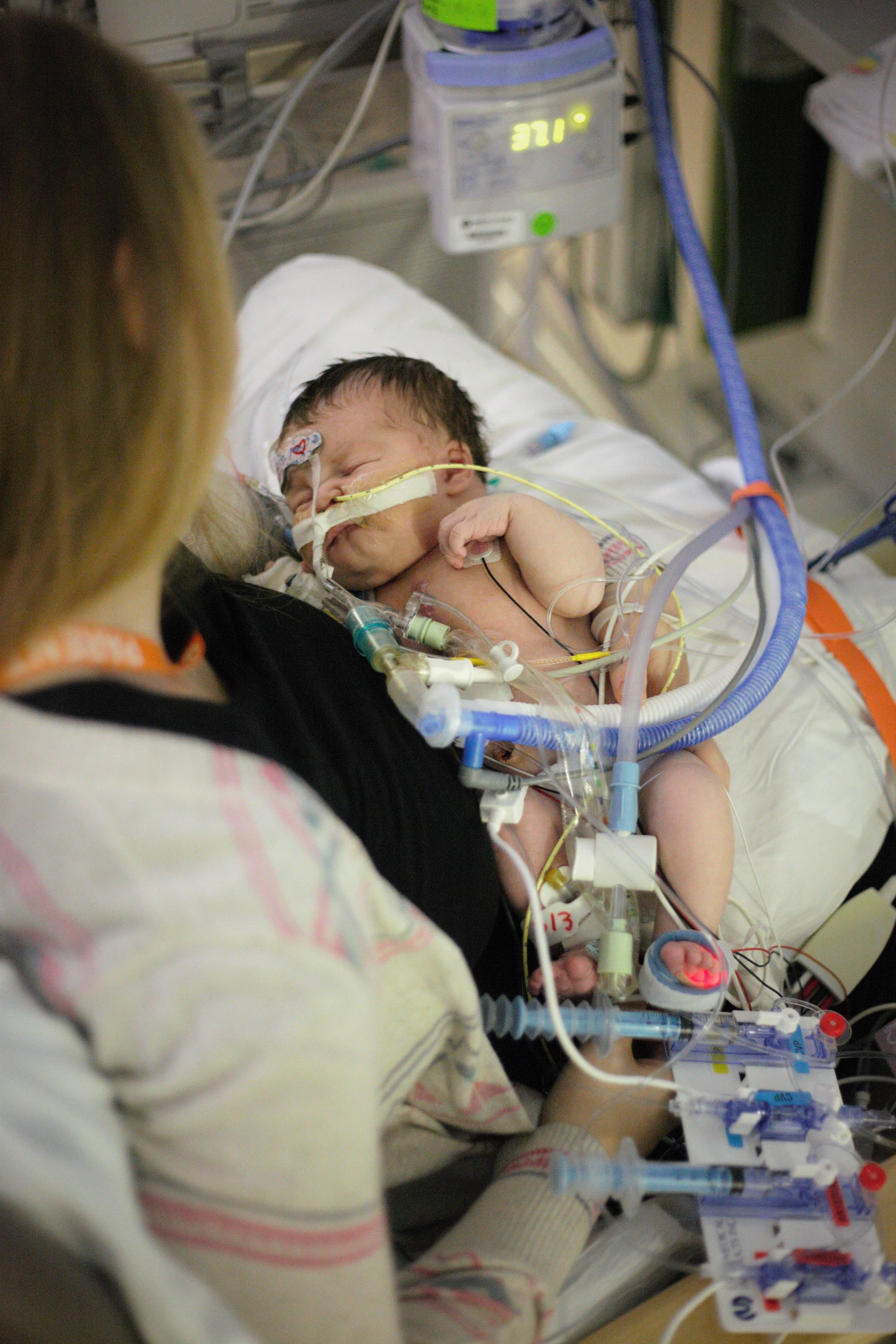
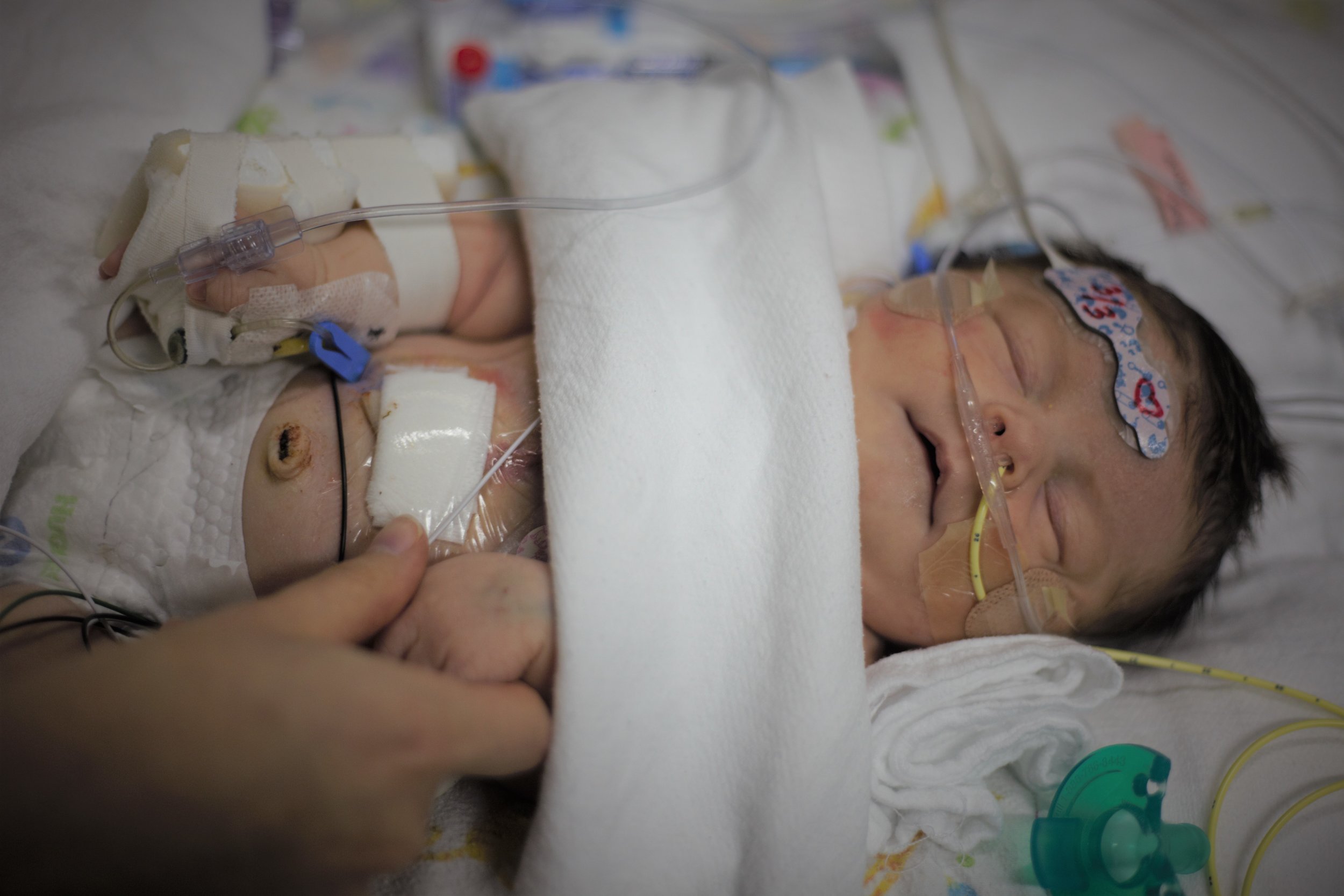
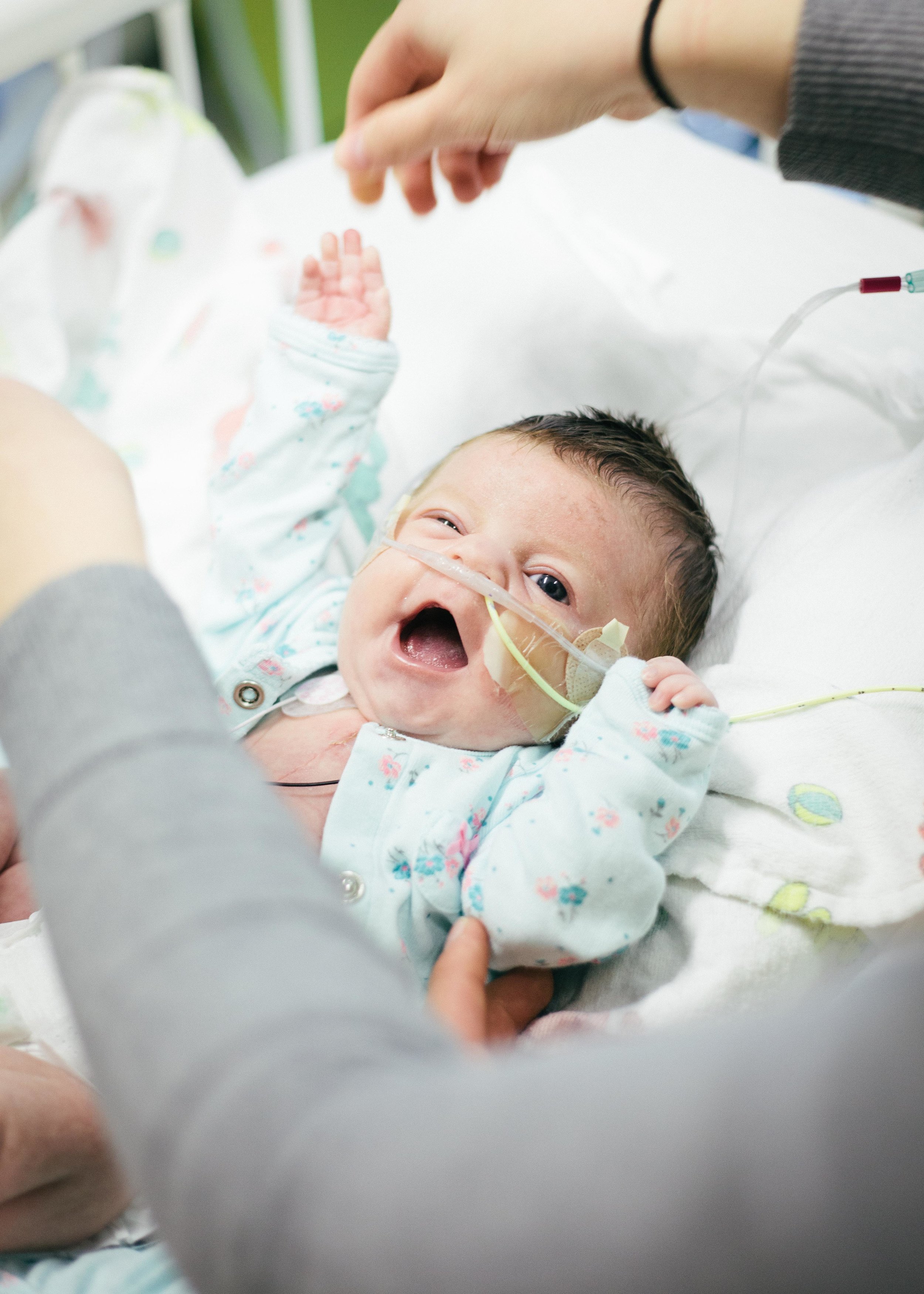
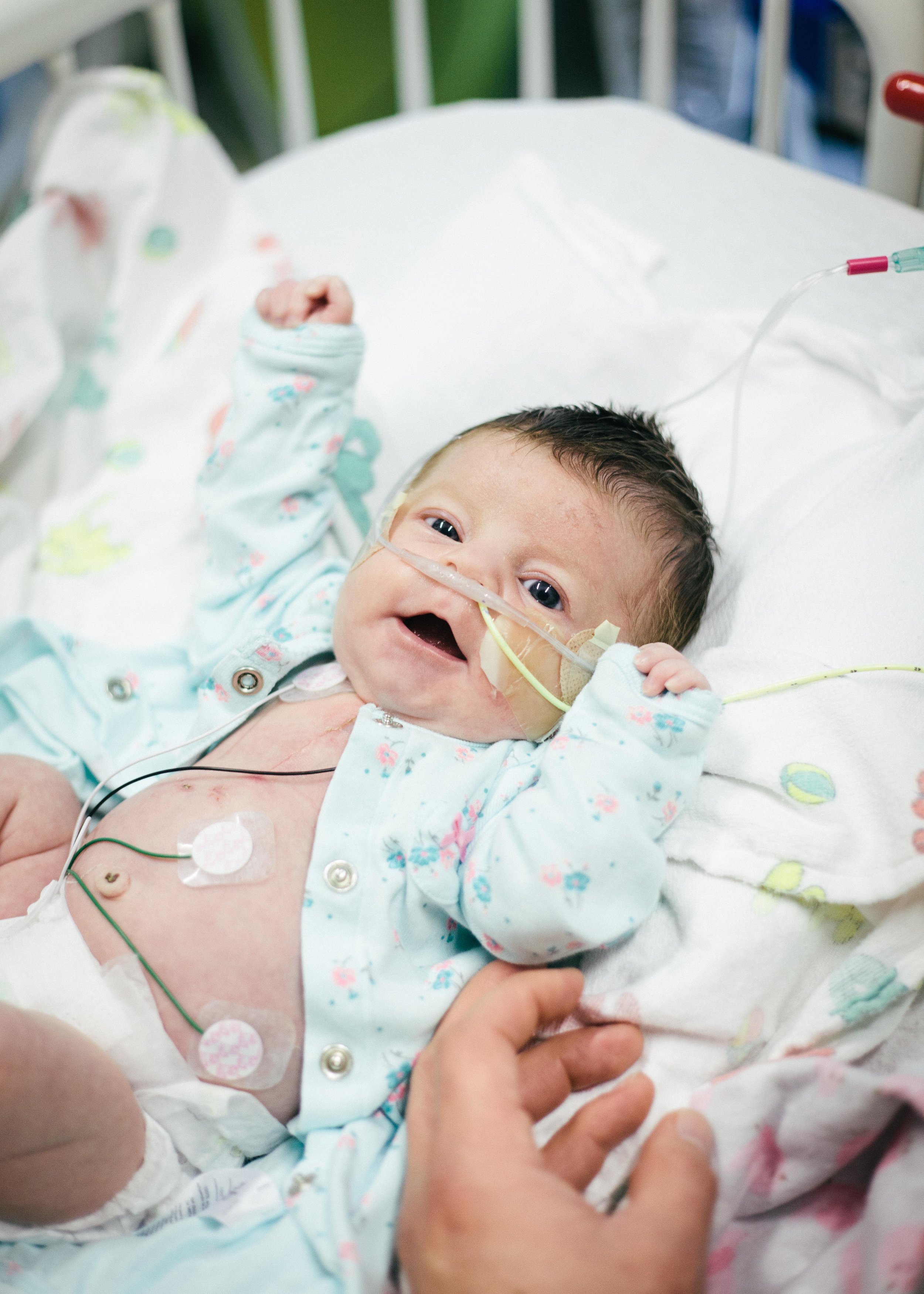
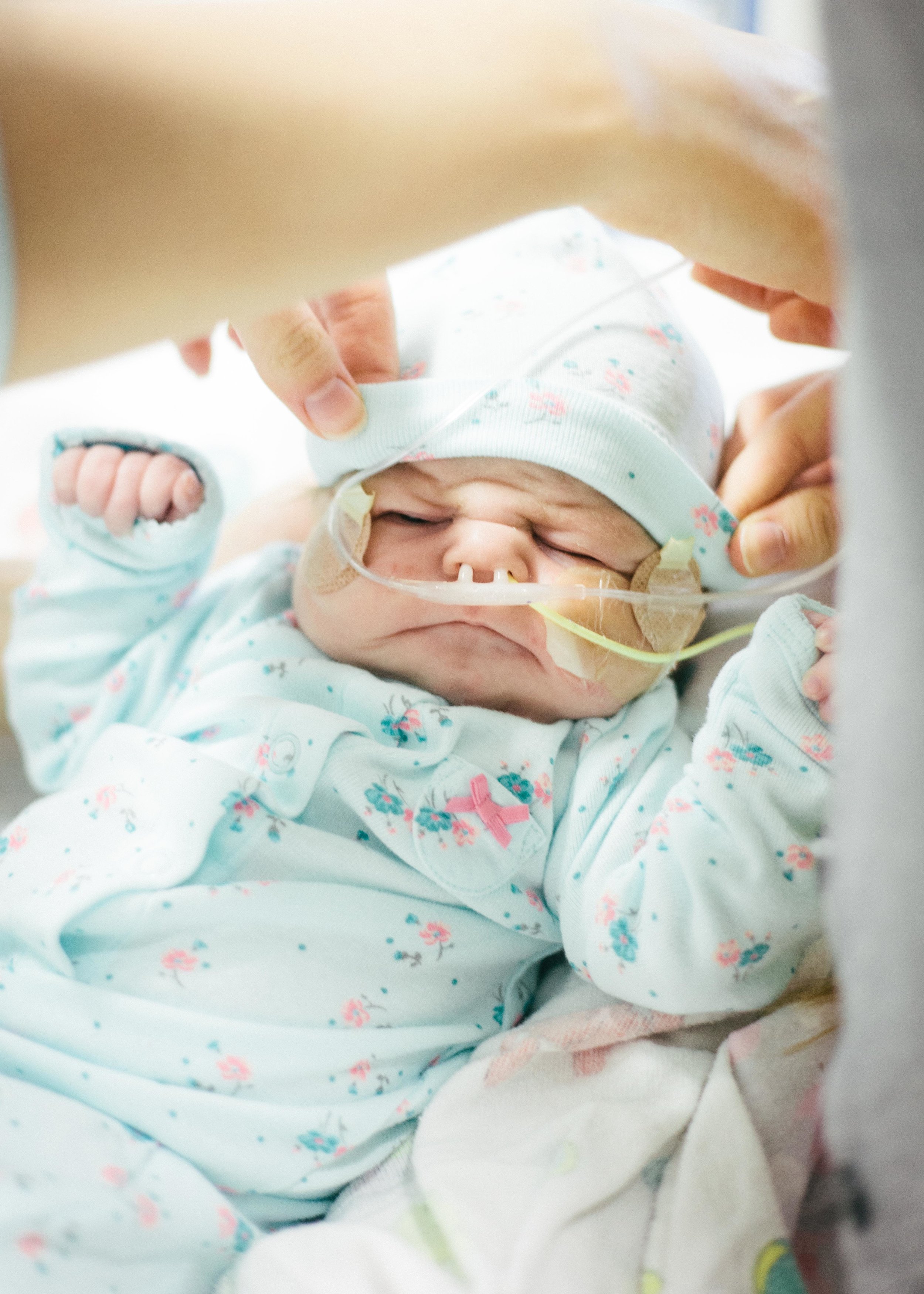
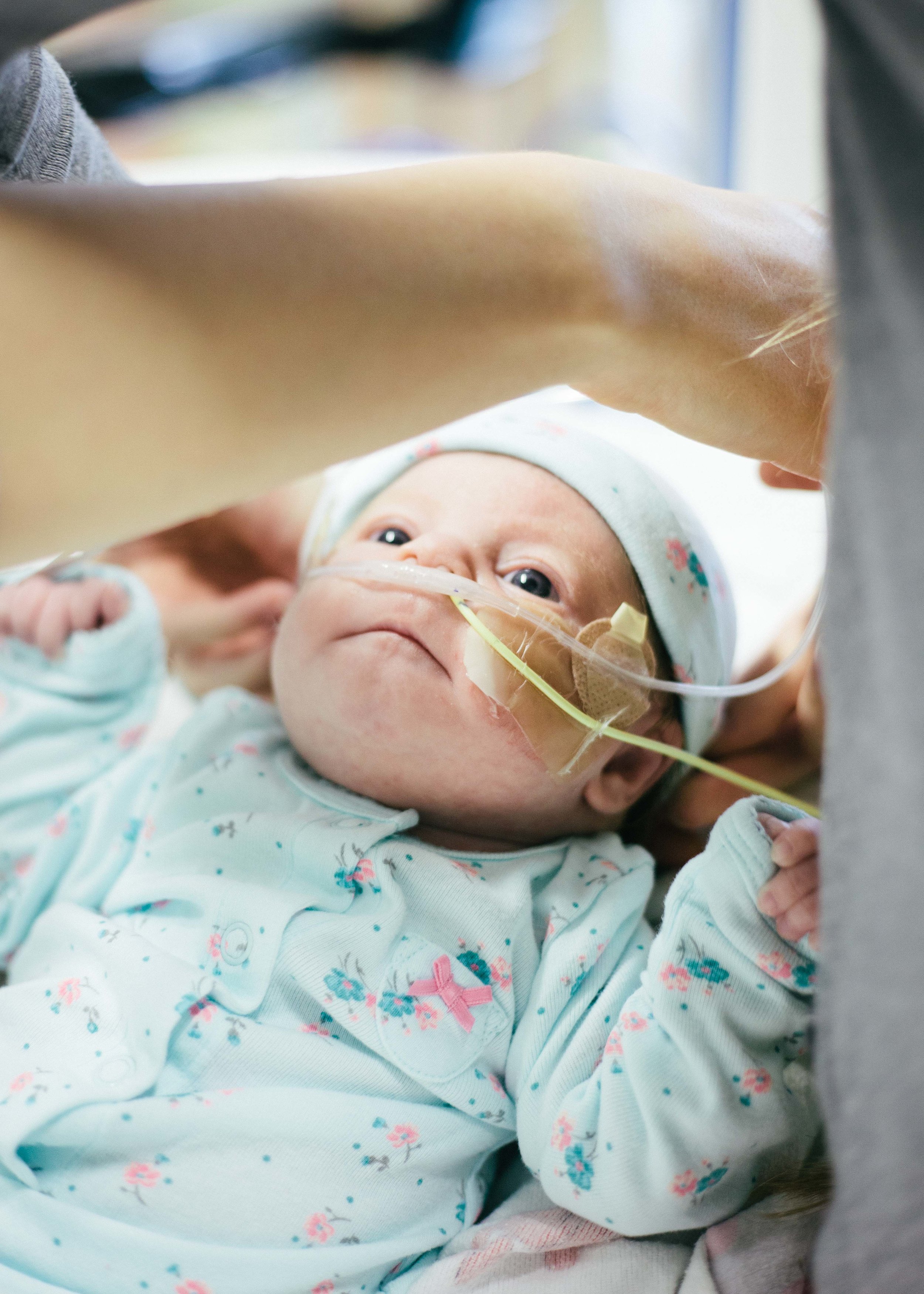
Here are some pictures from this evening just after her bath. She looks like the Shirley we know so well, alert and content.
-Joseph
Digging In
New Doctors
Along with the physicians that care for Shirley in the CICU a team of doctors that primarily work with "heart failure" have been brought on to consult in her everyday care. Shirley has had poor heart function since being taken off milrinone (the drug used to help the heart contract). Technically speaking there is a better phrase to describe her current state: Heart Failure. That sounds very bad and of course its not great but don't freak out. Heart failure is a very broad term used to describe the symptoms of a patient, in our case Shirley. She has been in a state of heart failure from birth. The large structural defects of her heart that were repaired during surgery can often times be the cure for neonatal congestive heart failure (CHF) but in Shirley's case her leaky valve combined with her heart not contracting with greater force are holding her back. Shirley's case isn't that severe, mind you, she is still functioning rather well given her issues. The doctors will simply be monitoring her and providing medications that will hopefully help her heart to work more efficiently. There still is some hope that her heart will rebound and function well enough to not need medication but now two and a half weeks post surgery they would have expected to see it already. It is highly likely that she will be in some state of heart failure until her valve is replaced.
Foxglove
This one is for the budding botanists out there. Shirley is starting a medication today to help address her minor case of heart failure. It's a drug called digoxin (wiki is a great source for this kind of stuff) and it's from a pretty little flowering plant called Digitalis, commonly known as foxglove. I was intrigued today when I found this out because I can remember being a child and having my mom tell us to not touch or play with foxglove while we tramped around in the woods. I knew it was poisonous and that it had something to do with it's effect on the heart but not much more than that. Crazy to think that the little plant we weren't allowed to play with as kids is now the same thing being used to treat our daughter's condition. There are many treatments for heart failure and digoxin is only one of many possible things they may try. The history of the drug goes way back and it's actually an interesting read. Hopefully she will respond well to it and won't need something more intense like milrinone. Digoxin is administered orally so it is a drug that can be given easily while at home if need be.
Rough Evening
Shirley is having a rough evening. I wrote the majority of this post earlier today but never got around to publishing it because Shirley started to get very fussy while I was holding her around 5pm. Shirley is a pretty relaxed baby so a few unprovoked fits put myself and her nurse on edge. They took her temp and it came back quite feverish at 101 and her heart rate jumped up between 180 and 190 BPM (she had been in the 130s and 140s all day). She was pretty upset for about 4 hours. They used some ice packs to cool her down and the doctors came to check her out. They are still waiting on the lab results to rule out infection. They also took a good look at her stomach to make sure there weren't any issues there. She has calmed down a little bit since but it is now 10pm and 5 minutes haven't passed the whole evening without some sort of unprovoked fit. Honestly they are hoping that it's just really bad gas that she is having difficulty passing but it's an unknown currently. The fever has come down which is a good sign but its also just a little strange.
Long Day
It wasn't a bad day but it wasn't a great day either. Shirley got to meet some new people today when my cousins came by to visit and also some aunts and uncles on Brianna's side. Today was the first day the term "heart failure" was used and that isn't really something that sits easy with anyone but they are confident that it will be manageable. Minus her fits and some issues this evening Shirley is still looking pretty comfortable and not too stressed on the whole. Hopefully she will have an uneventful night and be back to normal by the morning. The first half of the day went by very quickly but the last 6 hours have dragged on trying to calm little Shirley and being fixated at the live stream of vitals that is ever present on her monitor. Please continue to keep Shirley in your prayers. Now that the (very poorly named) "heart failure" team is monitoring Shirley we will be extending our stay in the CICU until they find a medication that works well for her overall. There is also the possibility that her heart starts to kick butt and pump like mad but they aren't waiting to find out.
Sorry if this post is all over the place but its just been a very interesting day. Here is a picture of Brianna feeding little Shirley her bottle this morning. I can't begin to relate to you how impressed I have been with how she has handled these extraordinary circumstances.
-Joseph
Pinch Us
Dream Land
None of us are wearing green and we feel like we are living in a dream state. Our current reality is a lot like a dream with unbelievable twists and turns, the occasional terrifying scenario, a strange environment, and a very cute baby. Seriously though, there are times this all feels like a dream. Maybe it's that we have, more or less, been in a 15x20ft box for three weeks putting us in a kind of non-drug induced trip. Well, maybe Shirley's is drug induced... but we are clean! Shirley is our little dream child as well. Although there is certainly a sense of what things could be like with an average child we couldn't be happier with the not so average child we were given. We still hold to the same belief we held before she was born, that is: Shirley has CHD for a reason beyond what is material and understandable. We also believe that no matter the outcome, Shirley's life is meant to bring good to us and others. With this hope and expectation we can charge into the days, months, and hopefully years ahead that we will be able to enjoy Shirley and the good she will bring to our lives and others. We don't know how many days are in any lifetime but that shouldn't cause us to live in fear. I think we both have a very clear understanding that this world does not revolve around our child, our family, or our lives. There are people suffering and enduring trials far worse than we can even imagine. I'll end this section with this: "Count it all joy, my brothers, when you meet trials of various kinds, for you know that the testing of your faith produces steadfastness."
Slow Going
We had a great talk with one of the "critical care" doctors today (about 10 minutes in length) and he explained Shirley's current status to us. They would love for us to leave the CICU but they just don't have the level of confidence in Shirley's heart that they would like. He said to think about it as a kind of pendulum; one side being a need for CICU care (possibly another procedure) and the other being a well functioning Shirley. He explained that she is just swinging back and forth somewhere in the middle. He was honest and said he has no idea when Shirley will be able to go home but they will do everything they can to make sure it is sooner rather than later. Shirley's leaky valve is the real concern for the team in the CICU and it will be the concern even after we are out of the CICU. What they are monitoring right now is whether or not she will present symptoms that will lead them to take action and attempt to correct her valve issues now rather than years from now. Years from now is by far the best option. During her surgery they thoroughly evaluated her truncal valve and concluded that it was, at the time, not worth the risk to attempt any kind of repair. The heart of a newborn is already extremely small (think strawberry) so imagining the precision needed to repair the valve is almost impossible. Valve replacements aren't really an option this early in life. What is more likely though is that she will need a host of drugs to help her heart to beat efficiently. Like my previous posts have said, her heart just isn't up to par. The Dr. did warn us that Shirley may need a much longer stay at SCH and that should at least be something we are aware of moving forawrd. Now, if you are thinking, "well that is typical hospital care, treat you more than you need and make tons of money on you in the process." I would caution you. Shirley is not the only child in the CICU. We met a family who arrived on Wednesday and will be discharged this weekend. Their son had OHS that same day and was closed and extubated immediately after surgery, sent to the step-down unit the next day and is now only taking the occasional Tylenol to help with pain. Their stay, from beginning to end, is likely to be less than a week. That is impressive and truly a reflection of how hard the team here is working to get children home where they belong. So, think whatever you would like. No two children are the same and I have no doubt that Shirley will leave SCH as soon as possible.
This just in (literally), Shirley drank 17ml (an hour's worth of milk) via a bottle in about 10 minutes. That is great work for a baby that has had so little practice feeding orally.
I hope you are enjoying these posts and find them informative! I am certainly enjoying writing them! The second photo is just killing me! I can't believe how cute Shirley is!
-Joseph

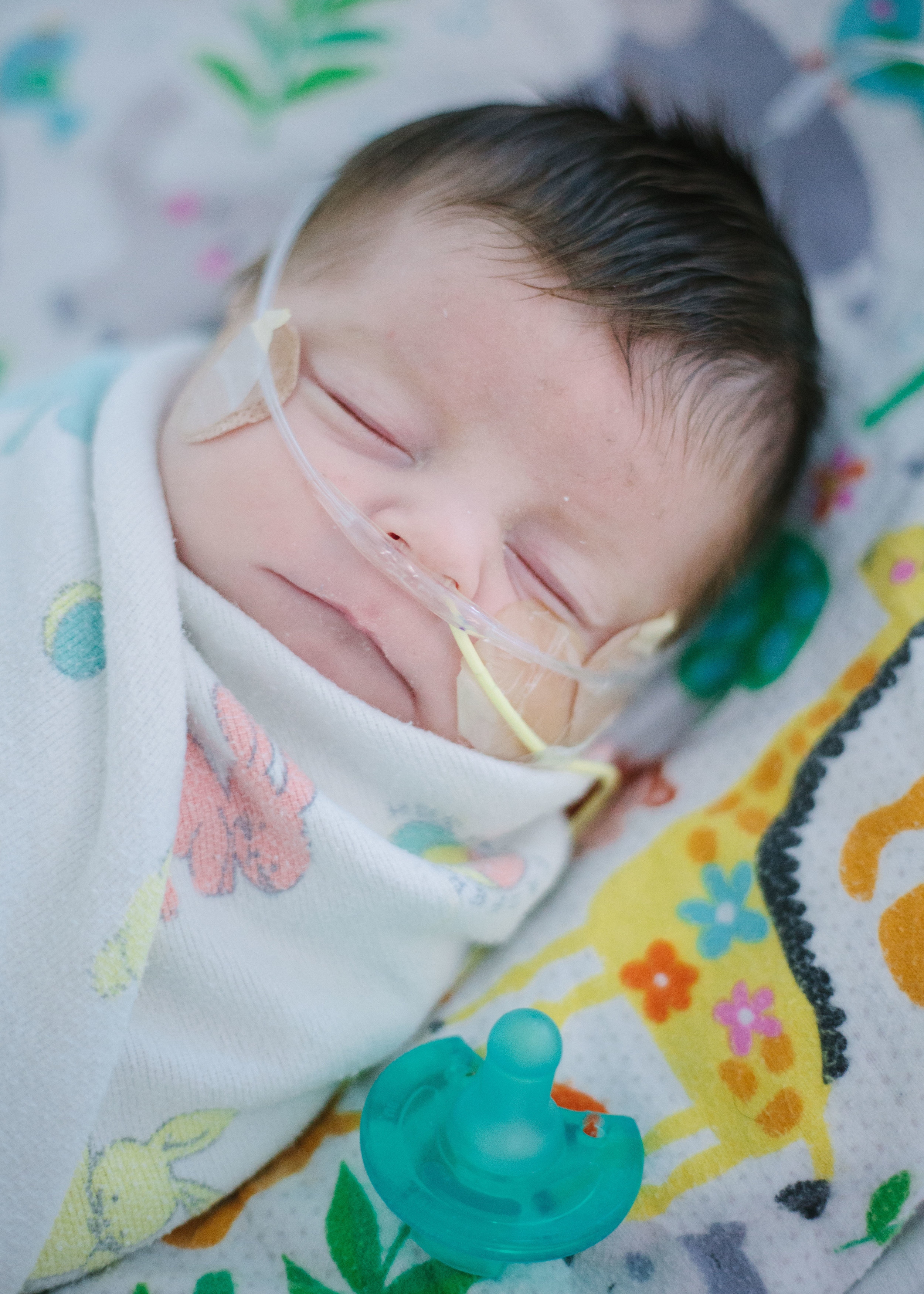
Week Three
Three Weeks
Shirley was born three weeks ago today! I can't believe how fast these few weeks have passed. The hospital environment has been amazing believe it or not. We are here with our wonderful and beautiful daughter, what more could you possibly ask for?
Seattle Children's
Seattle Children's Hospital has been unbelievable. I heard that it was a great place but actually experiencing it has been something else entirely. I have yet to meet a single person that has not genuinely cared about Shirley's or our needs. Whether you're talking with a Dr. or janitor they all show you the same amount of respect and care. The diversity of the staff here is also very impressive. It doesn't matter where in the world they may be from you get a sense of confidence, humility, smarts, and care from every person. I'm not sure how they do their hiring but they are doing something right. It's very hard to convey the level of confidence I have in the staff here but it's off the charts. "Do you have any questions?" and "is there anything I can do for you?" are some of the most common things you hear from nurses and doctors alike. They will explain just about anything to you and hear you out on any concern you raise. So much more could be said.
Heart Function and HFNC
Shirley had another echo today because they were concerned about her overall function. She is looking great in person but poor on paper. The last echo showed that she had some decreased heart function and this echo showed that it was a little worse than a few days ago. It sets off alarms in my head but the doctors aren't overly concerned. They still haven't given her drugs to help her function but its definitely on the table. Her best option is to go back on melirinone to help her heart contract with more force. The electrophysiologist took a look at her EKG today and said that her PACs and PVCs are not concerning given her recent surgery. Its possible that her heart tissue is still just irritated from surgery and that it may be causing the premature contractions. Also treating them right now isn't even an option. Her BP won't even allow them to add the β-blocker used to treat the arrhythmias. Her diastolic pressure is on the low side because of the vasodilator she is on to help with perfusion and the β-blocker is pretty much a "chill pill" for the heart. They are going to continue monitoring Shirley in the CICU for another few days. Shirley is only receiving 2LPM at "room air" through her HFNC now! Her breathing is still looking pretty good and the hope is she will be weaned off shortly.
Breastfeeding
On a very positive note... Shirley is a breastfeeding pro! OT/PT came today and observed her breathing and how she had no mercy on her pacifier and decided that it was time to try a feeding at the breast. Shirley latched immediately and was able to pause her breathing in order to swallow perfectly. That is one of the huge hurdles for a lot of children. Shirley gets 10 minutes three times a day at the breast now! It made me so happy to see Brianna get to bond with and feed Shirley the way she always wanted to. The possibility of not breastfeeding was something Brianna had already come to terms with and now being able to is a great boost in morale.
If you can handle all 3:27 of this video you will be able to see the little one fall asleep at the very end! If she is getting tired it only take a little pass down the forehead to the tip of the nose with a finger and she will pass out 90% of the time!
-Joseph
Normal Baby Stuff
Dress Up
Today is a big day for Shirley! Nearly three weeks old she will be able to wear her first outfit today! You didn't miss much yesterday but her last IV was taken out of her foot and her HFNC was decreased to 4LPM. Now that her IV is out we can dress her in one of her cute snap-down outfits! Brianna has probably been dreaming of dressing her child ever since she was wearing her own snap-down onesies, so its a huge day for her. Shirley has also been wearing little pink mittens to protect her face from those razor sharpe nails she sports.
Foot Prints
We did some footprints today. Now that her feet are free of those clumsy IV's we jumped on the opportunity to do the frivolous sentimental things! Like most baby feet, Shirley's feet are cute as all get out and to have an ink stamped representation of them is even more cute! I joked before we did the stamping that it may be a more accurate representation to keep the band-aid on her foot. Shirley thought so too, I guess, because if you look closely at the picture you can see a band-aid mark on her right heel! Having spent the whole three weeks of your child's life in an ICU, normal things become extraordinary things. When the plan of the day changes from open heart surgery and ensuring she doesn't have a stroke, to baby clothes and footprints it's a great feeling. We are moving on from truly sad and scary days to happy and fun days, though each day with Shirley has been filled with a real joy and peace no matter her condition. Joy and hope should not be overshadowed by fear and uncertainty. I want to write an entire post about joy, hope, fear, sadness and the like but its a work in progress. That, along with a post about wondering why Shirley has CHD have been brewing since day one.
Medical Jargon
Like I said earlier, Shirley was weaned to 4LPM on the HFNC and had her last IV removed yesterday. Sometimes the critical care docs will backtrack on the IV's though and want one just in case they need it. Let's hope they don't. Shirley is getting a full blood work-up today and had another echo ordered for the beginning of next week. She has been having some issues with premature ventricular contractions as well as premature atrial contractions, PAV's and PAC's respectively. These are both somewhat common for children with CHD and specifically those with large structural defects such as Shirley's. They can also be caused by an imbalance/deficiencies electrolytes. It can be difficult to pinpoint for her though because of some of the medications she is receiving. She is currently on two diuretics that make her pee quite often in order to help her fluid levels stay balanced and reduce the risk of acute pulmonary edema (this is a great link with tons of information). The diuretics would be the likely culprit for a electrolyte imbalance but its not that easy. Her labs come back with differing results, sometimes she might be low on an electrolyte or two sometimes her levels look great, yet the PVC's and PAC's remain. She is receiving breast milk which contains everything she needs as far as nutrition plus it is being fortified to help add calories so she can plump up. The moral of the story is that she is getting plenty of electrolytes with her feeds. There are also genetic things to consider concerning her electrolyte balance but the results are still out on her comprehensive screen.
Respiration Rate
Her HFNC has been weaned rather quickly and is likely the only thing keeping us in the CICU. There have been rumors of possibly shipping her out tomorrow. She is currently on 4LPM of "room air" for support and her RR is fluctuating from from about 50 to 70. Her last few x-rays have shown that her lungs are relatively dry thanks to the diuretics and the HFNC having been set to 8LPM for almost 48 hours a few days back. This is a great sign that she is at low risk for acute pulmonary edema and its likely not affecting her RR. Hopefully her breathing will continue to improve and that she will be able to make the jump to zero support shortly.
Heart Function
Her heart function is still slightly decreased but they're hopeful it will perk up. Labs will come back today with her most recent BNP levels as well as some other markers that may help them determine her cardiac function. I think her next echo is scheduled for Monday, which will be more definitive. That being said, heart function, believe it or not, is not one of the things keeping us in the CICU at this moment. Shirley has a troubled heart and to ever expect it to function like the average heart is out of the question but there is hope that it will function better than it does today.
Thanks
Thank you all for the continued support. I have no doubt that this entire experience has been eased by the tremendous amount of support we have received in every way. I can't imagine what it would be like without it. There are many families here in the CICU that are not as fortunate. Please keep them in your prayers as well. We are just one family here in an ever changing manifest of patients. We are very thankful to have meet a few of the families here and exchange stories. Its been our goal to attempt to brighten the days of any person we meet by being helpful and hopeful in our interactions.
Until next time, here are some pictures from this morning. Don't worry, it's okay if you return multiple times a day to check out how cute she is or to see if she is as cute as you remembered. No one is judging you except you!
-Joseph
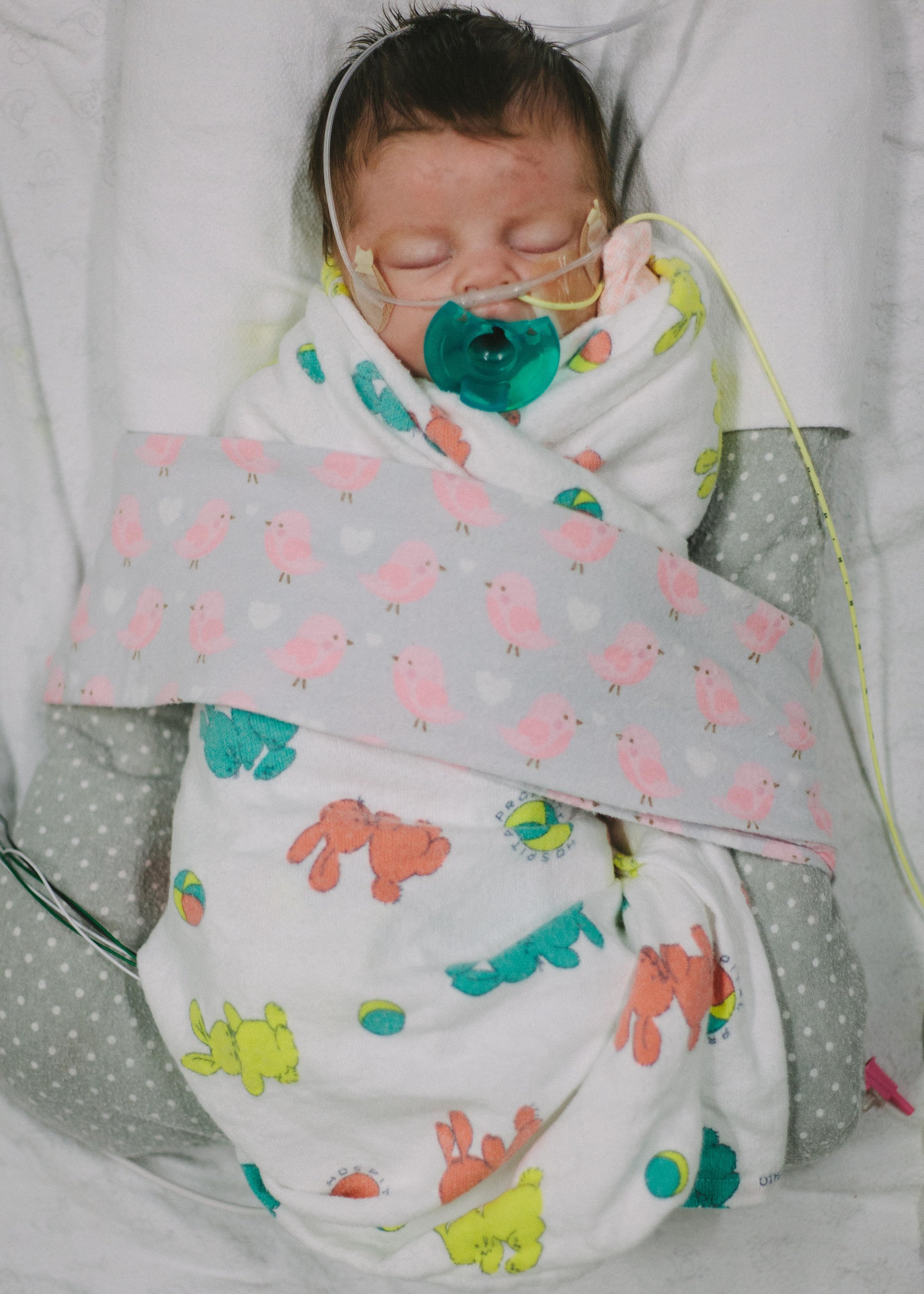



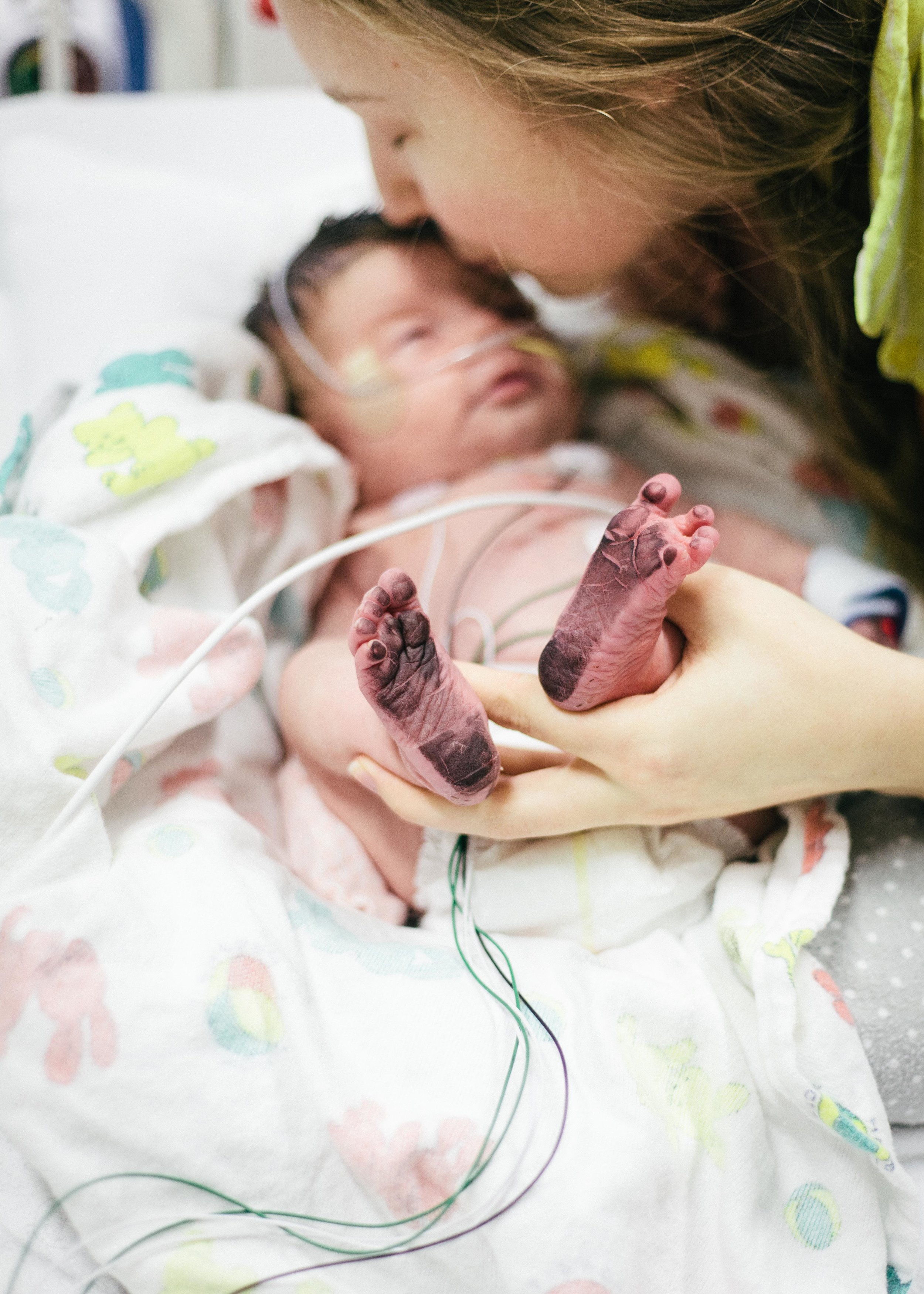
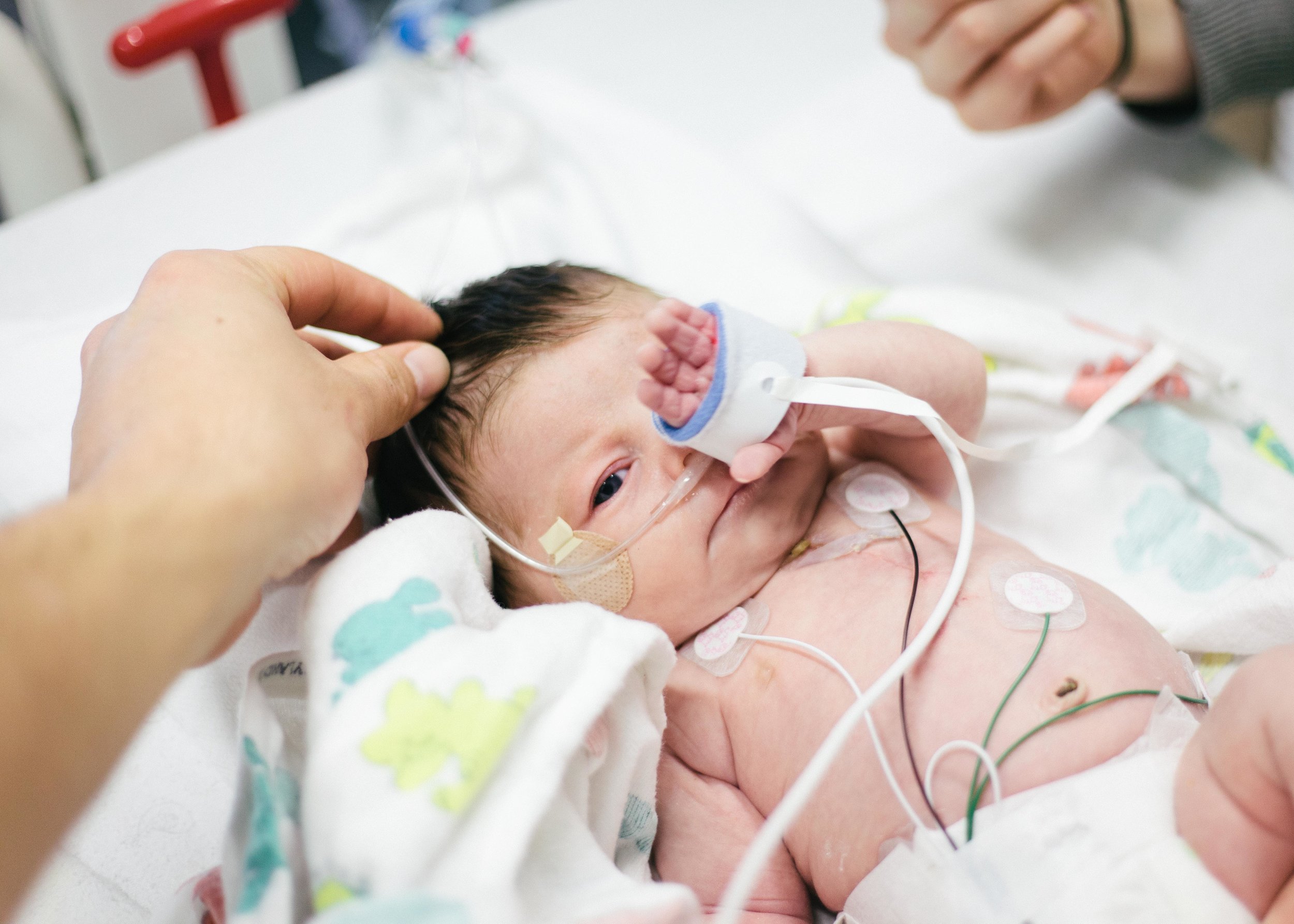
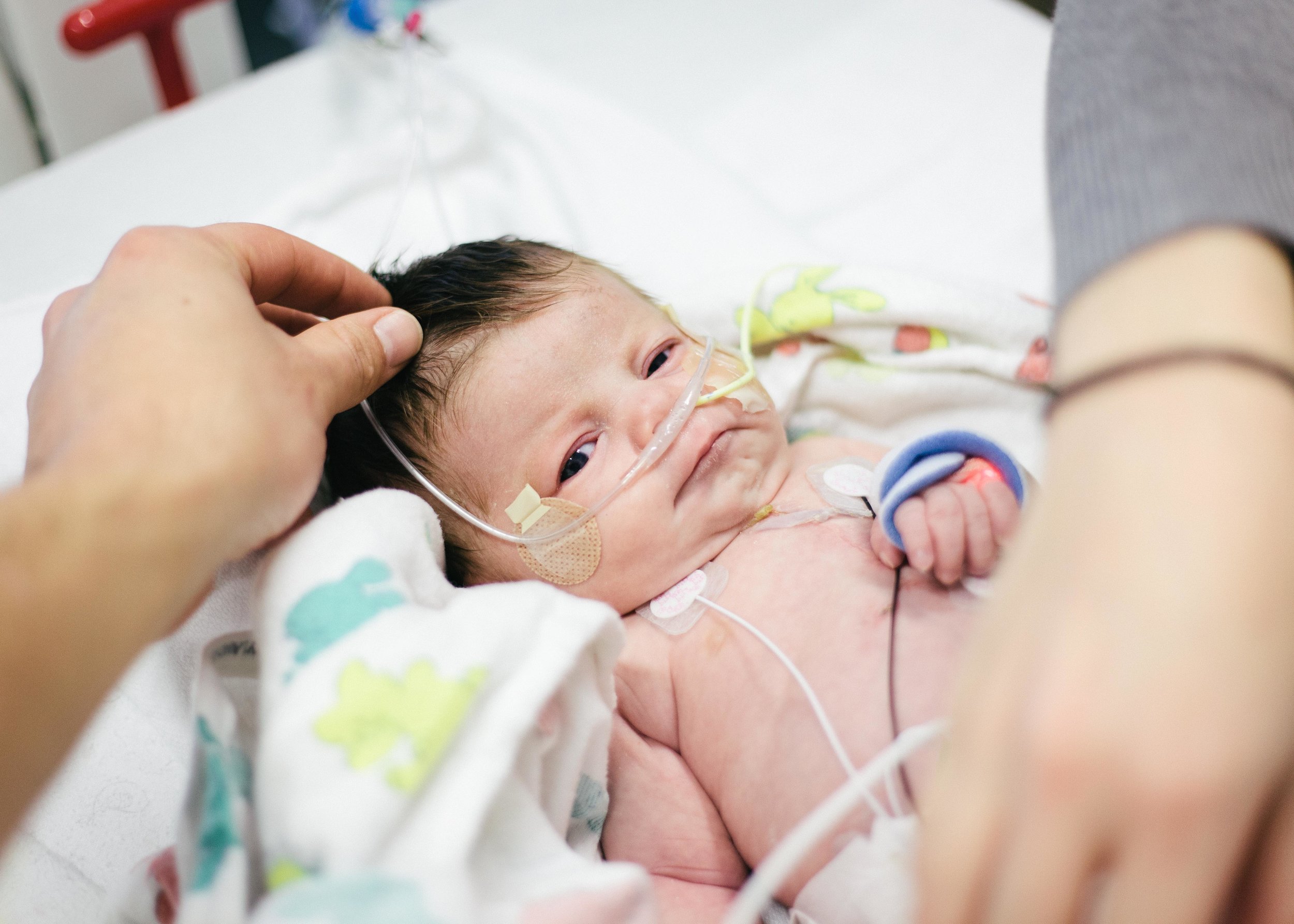
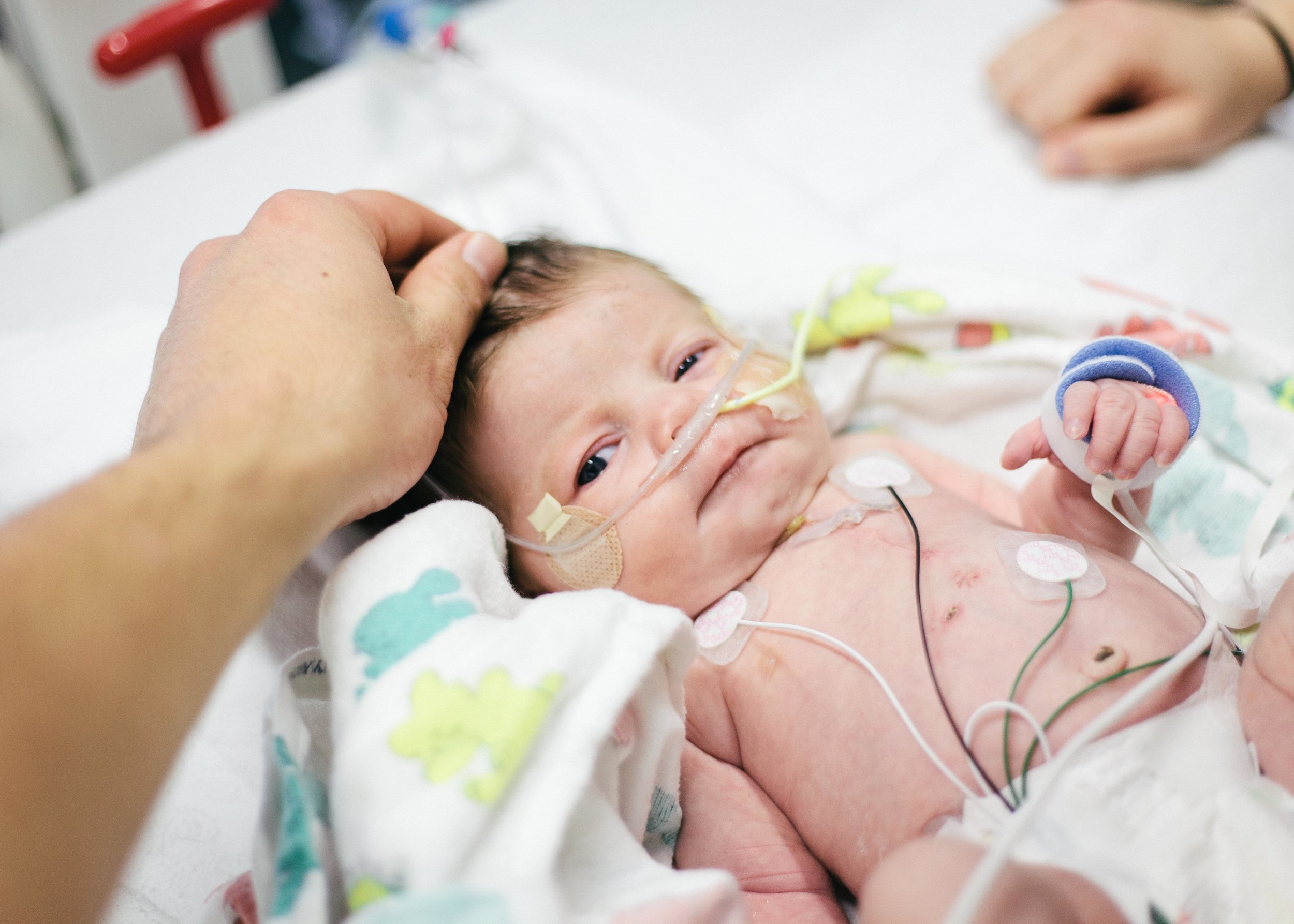
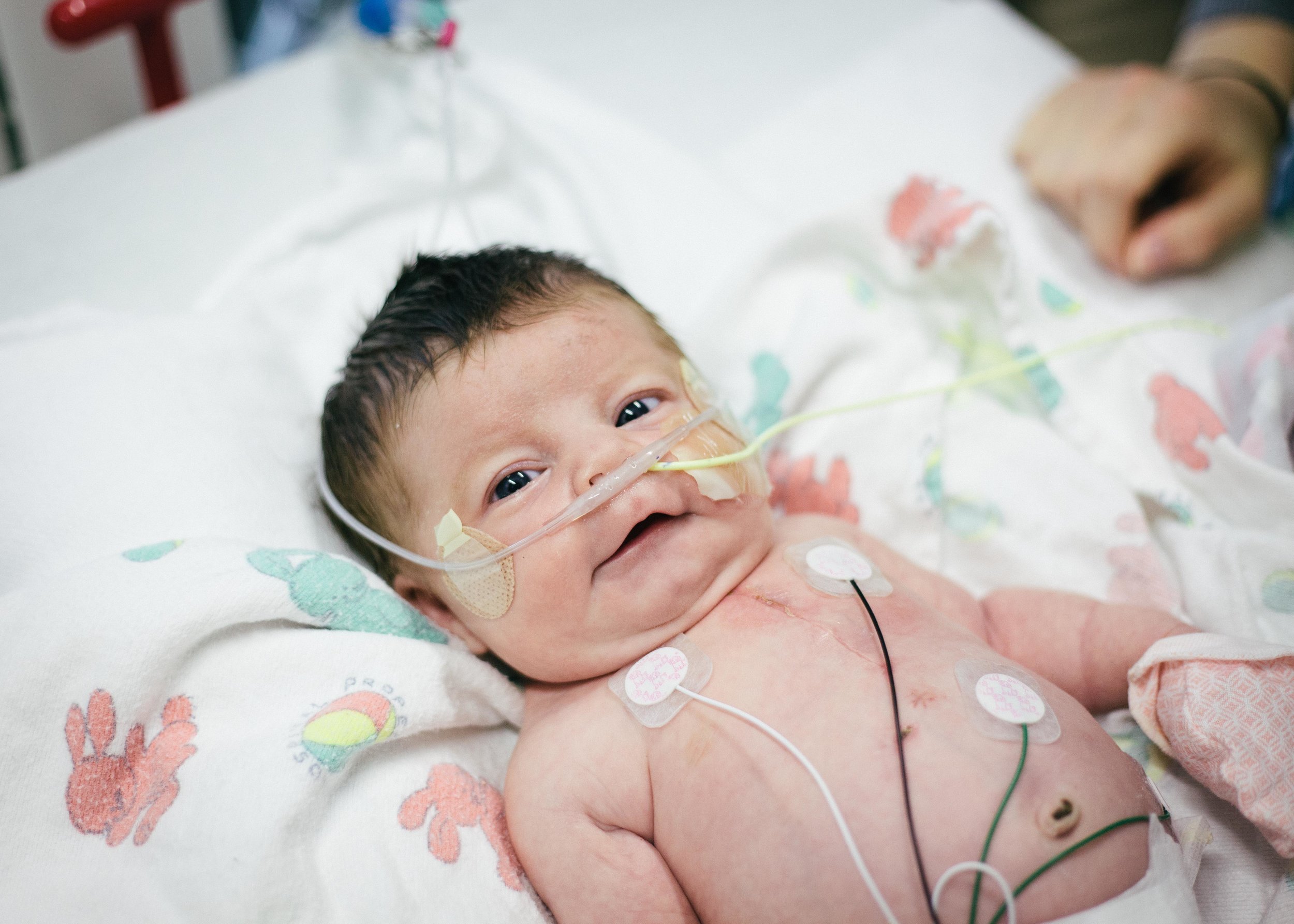
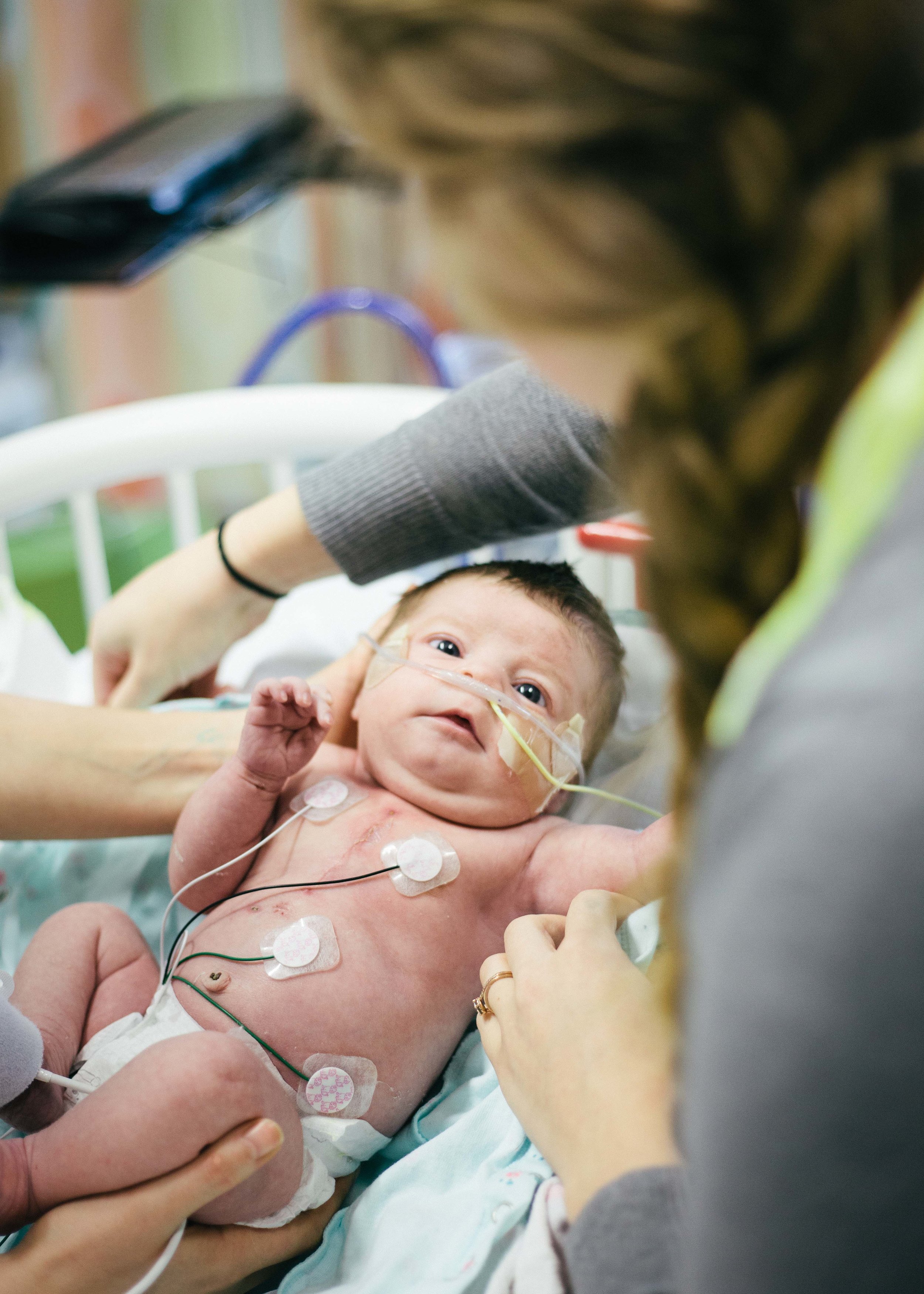
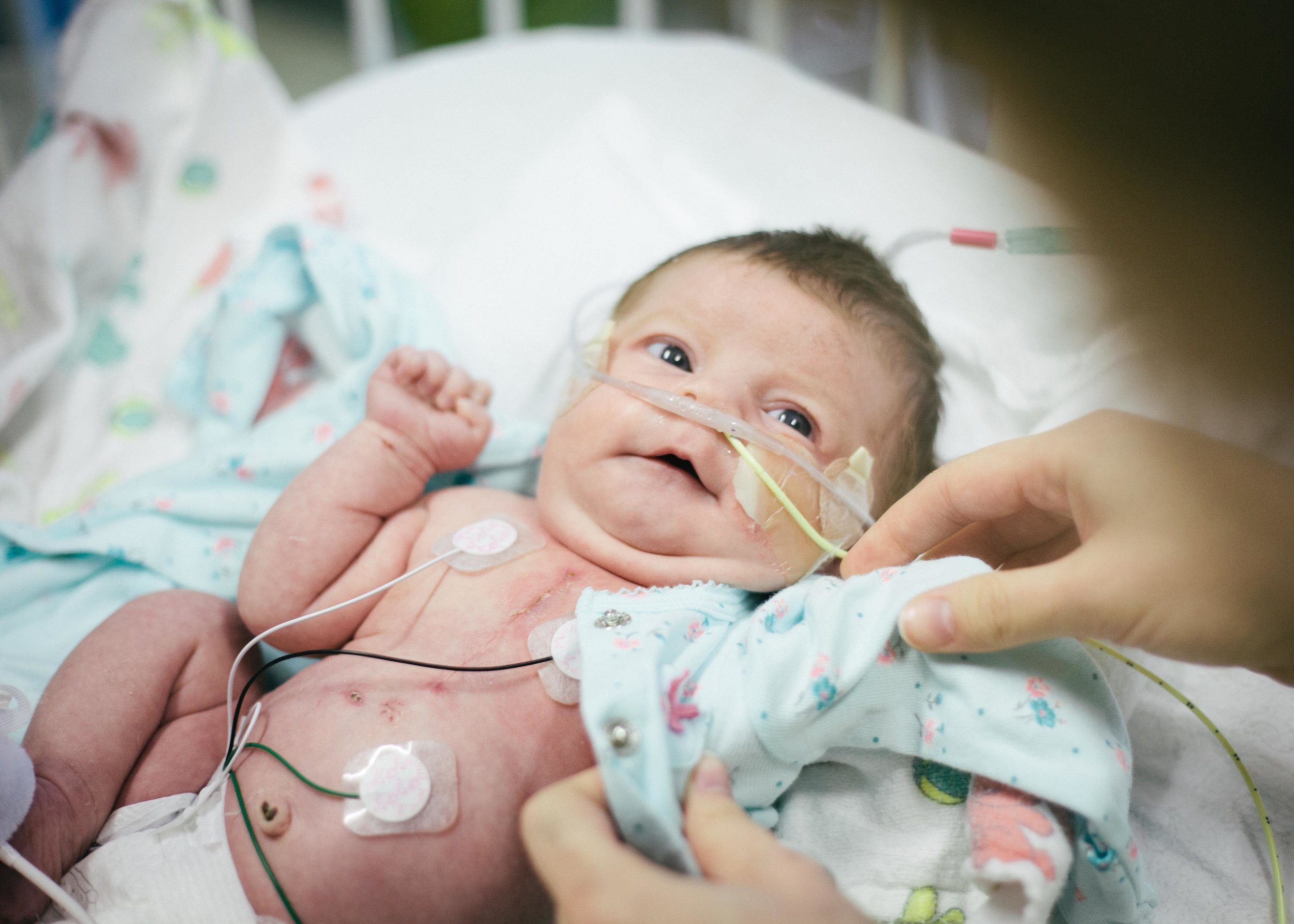

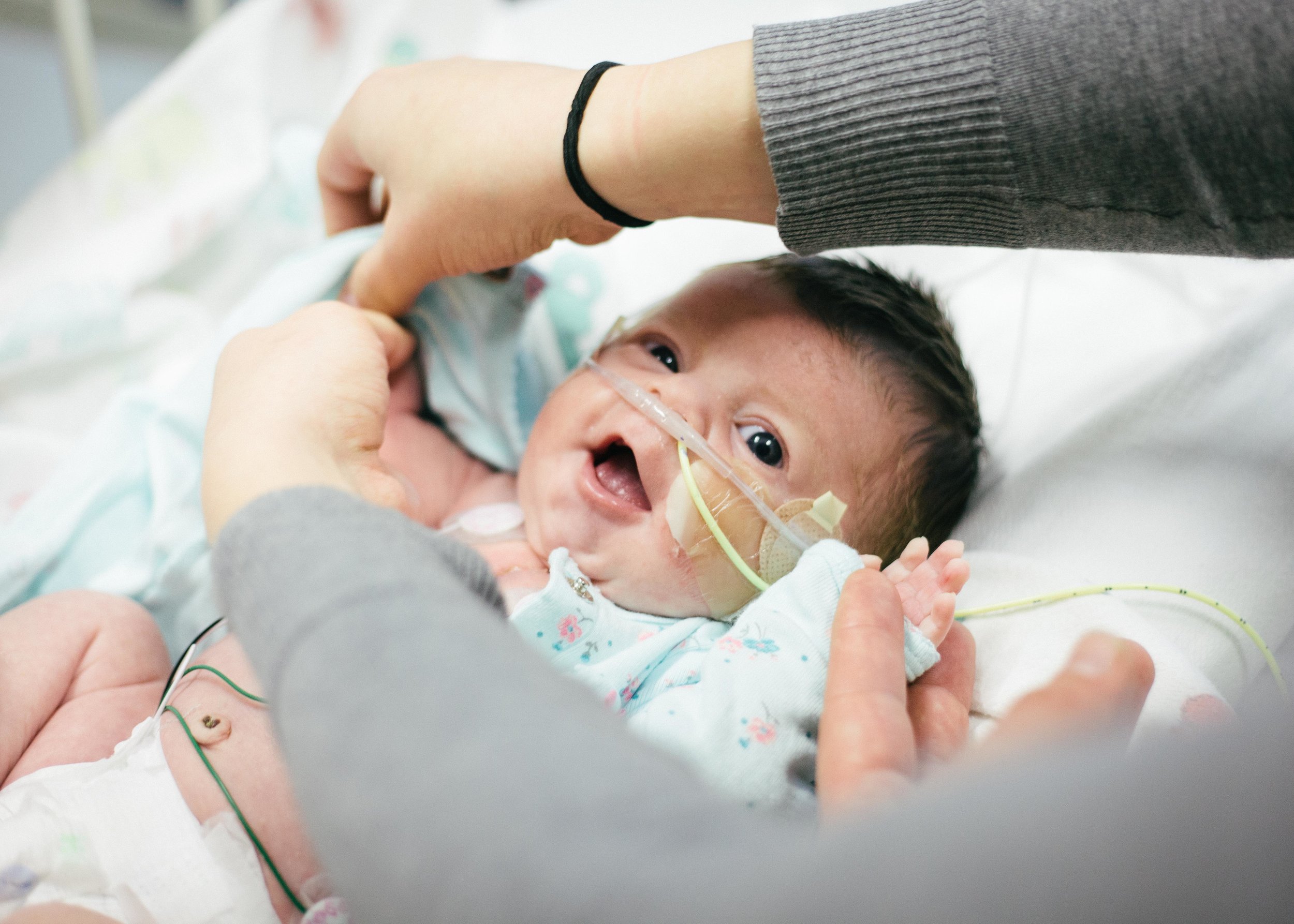

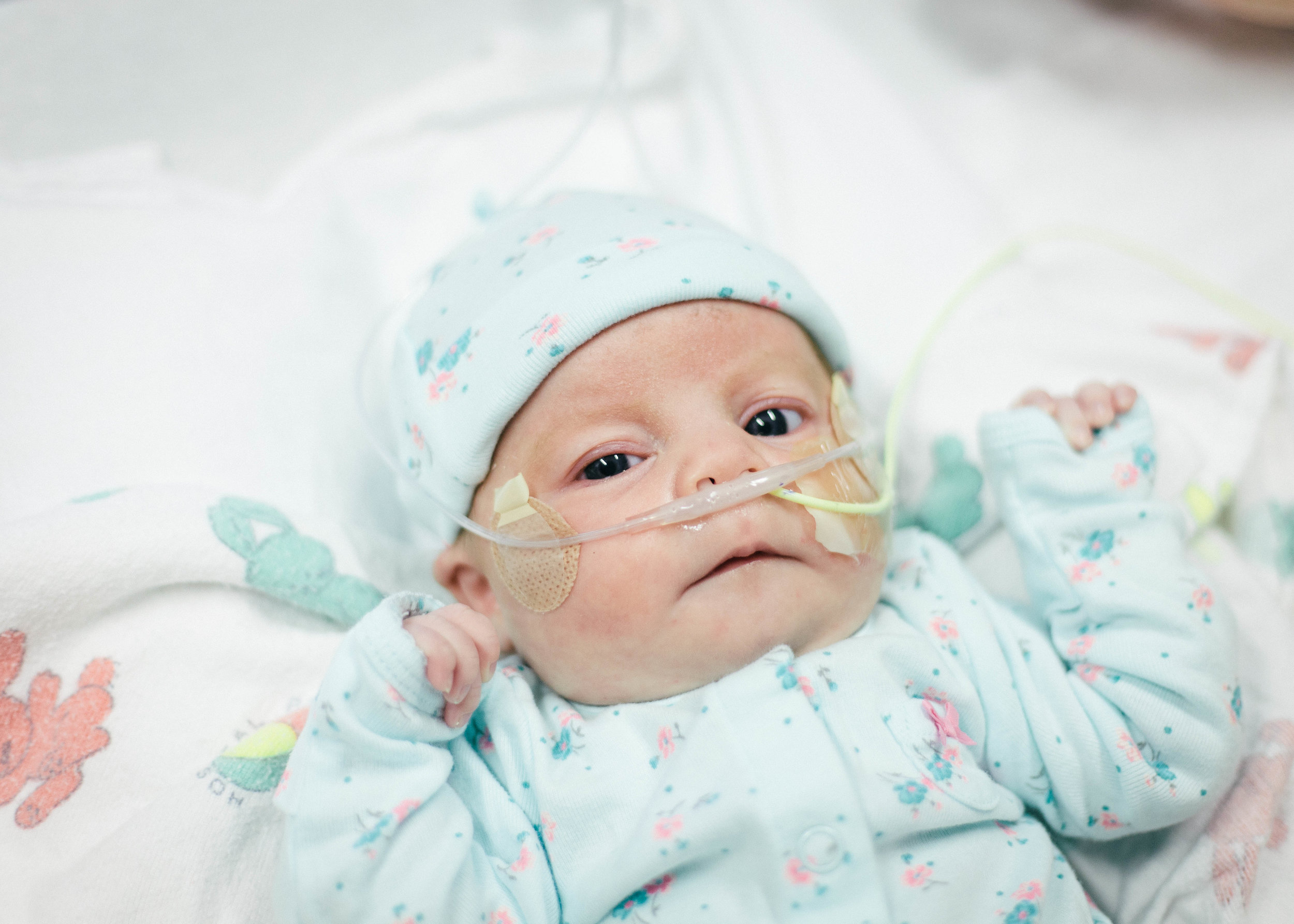


Pressing On
Breathing and Pooping
Shirley is having a pretty good day. Her HFNC was set to 7LPM this morning and then 6LPM this afternoon. Her RR has continued to hover in the 50-60s. The faster they wean her the sooner she can get to the step down unit. She has to be <4LPM for 24 hours and maintain a RR that doesn't strain her too much. Shirley is starting to make us feel more like parents these days. It used to be a real adventure to change her diaper. After surgery we had to take extra precautions to change her diaper and we still do but we have come a long way. She used to be on a medication that made her bones very soft. They even have a sign that warns people about "fragile bones." Before her PICC line came out you had to ensure that her foot was nowhere near her bottom when changing a poopy diaper. If her foot came in contact with her fecal matter you ran the risk of getting a blood infection. Those things are behind us now but a lot of the wires remain. I've changed a few diapers so it not just a learning curve! Today was the first time though that we changed her diaper, went through the whole ordeal and then 2 minutes later changed it again because she soiled it immediately after we were done. Even changing diapers can be the highlight of the day.
Heart Function
Shirley had another echo today, the first since she was taken off milrinone. In case you forgot, that was the vasodilator that also helped her heart contract. The echo wasn't the most positive but it's also not bad news. Her heart isn't contracting as well as it was when she was on milrinone which they expected, they just wanted it to be better than it is. The right side of her heart is also not up to par in the function category. These aren't things that will necessarily keep us in the CICU but they may be things that will need to be treated with drugs. If her heart is stressed beyond what it can handle and left to try and fix itself, there can be some rather negative results. They are going to give her a few days and continue to monitor her BNP levels. If her heart is up to the challenge she won't need more drugs but if there is no improvement they will add something to help her heart contract. Its a fine balance though. They don't want to do all the work for her but they also don't want her to begin to struggle. Pray that her little heart can strengthen before they have to intervene with more drugs.
Shirley keeps turning heads in the CICU, doctors and nurses are always stopping mid-sentence to remark about her cuteness or her calmness.
I'm still new to this whole blog thing but I figured out the comments and subscription thing today. There is a comment box at the end of the post as well as a link to receive e-mails when there are new posts!
I got some really great photos of Shirley being her usual happy self. Hope you enjoy.
-Joseph

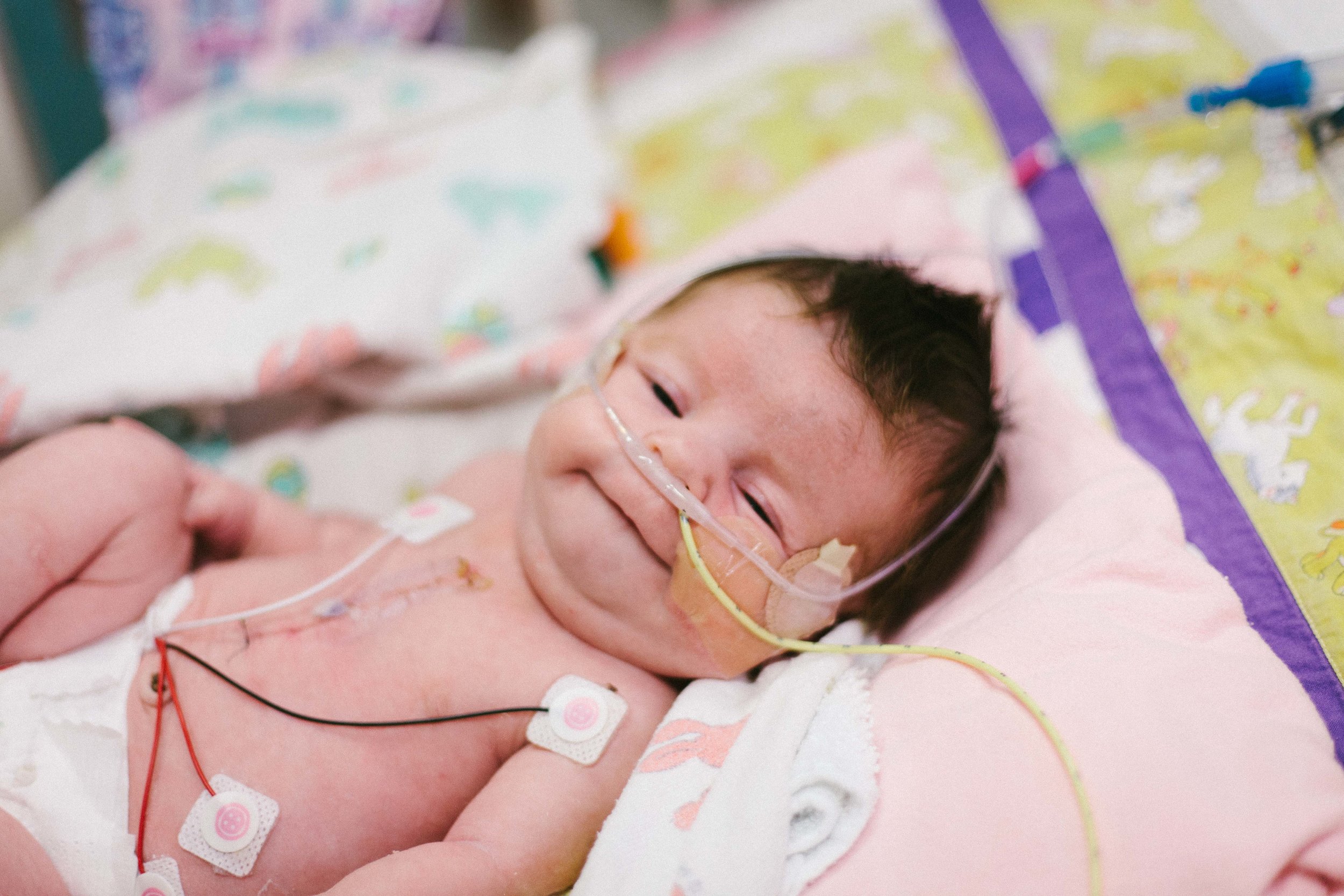
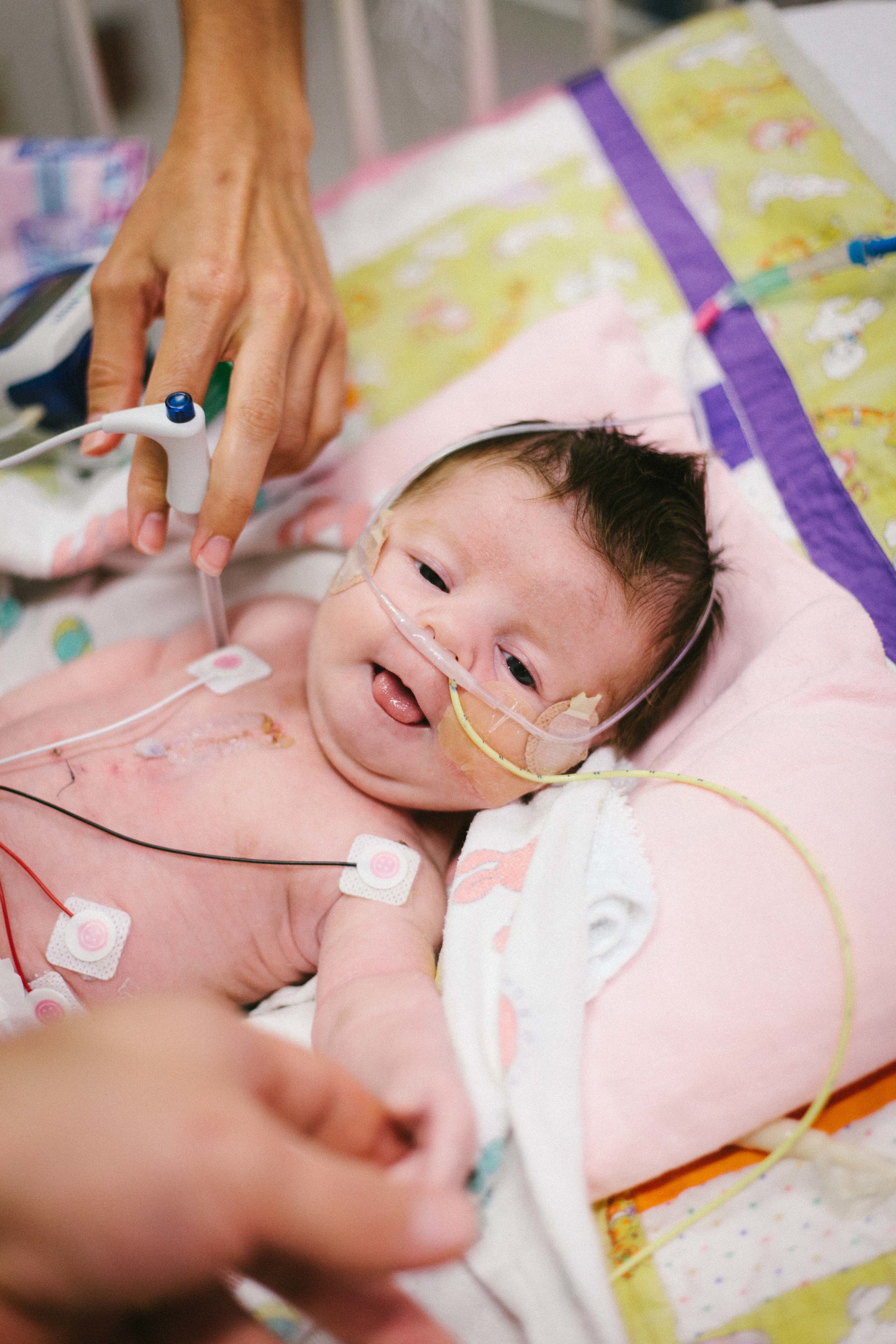
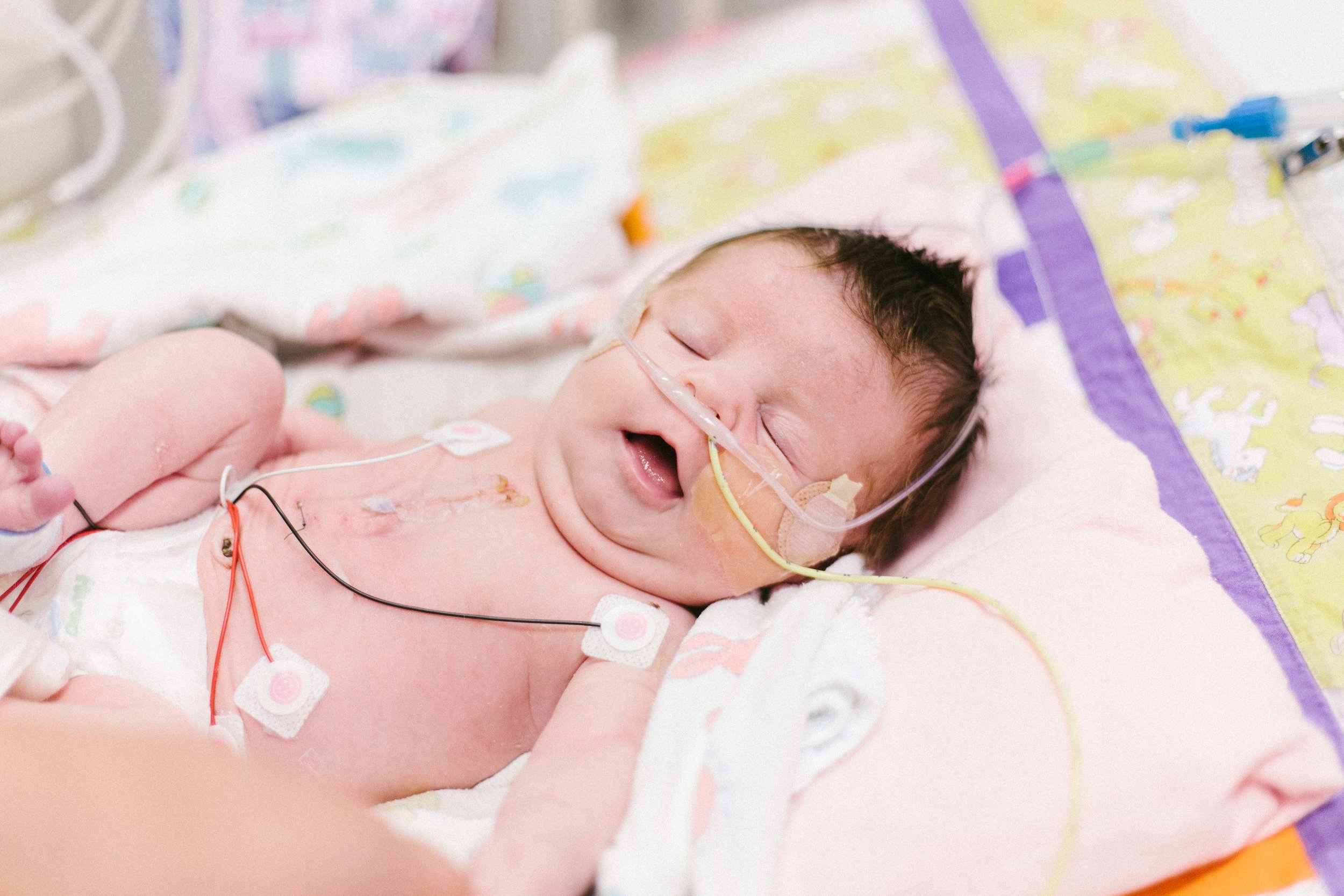
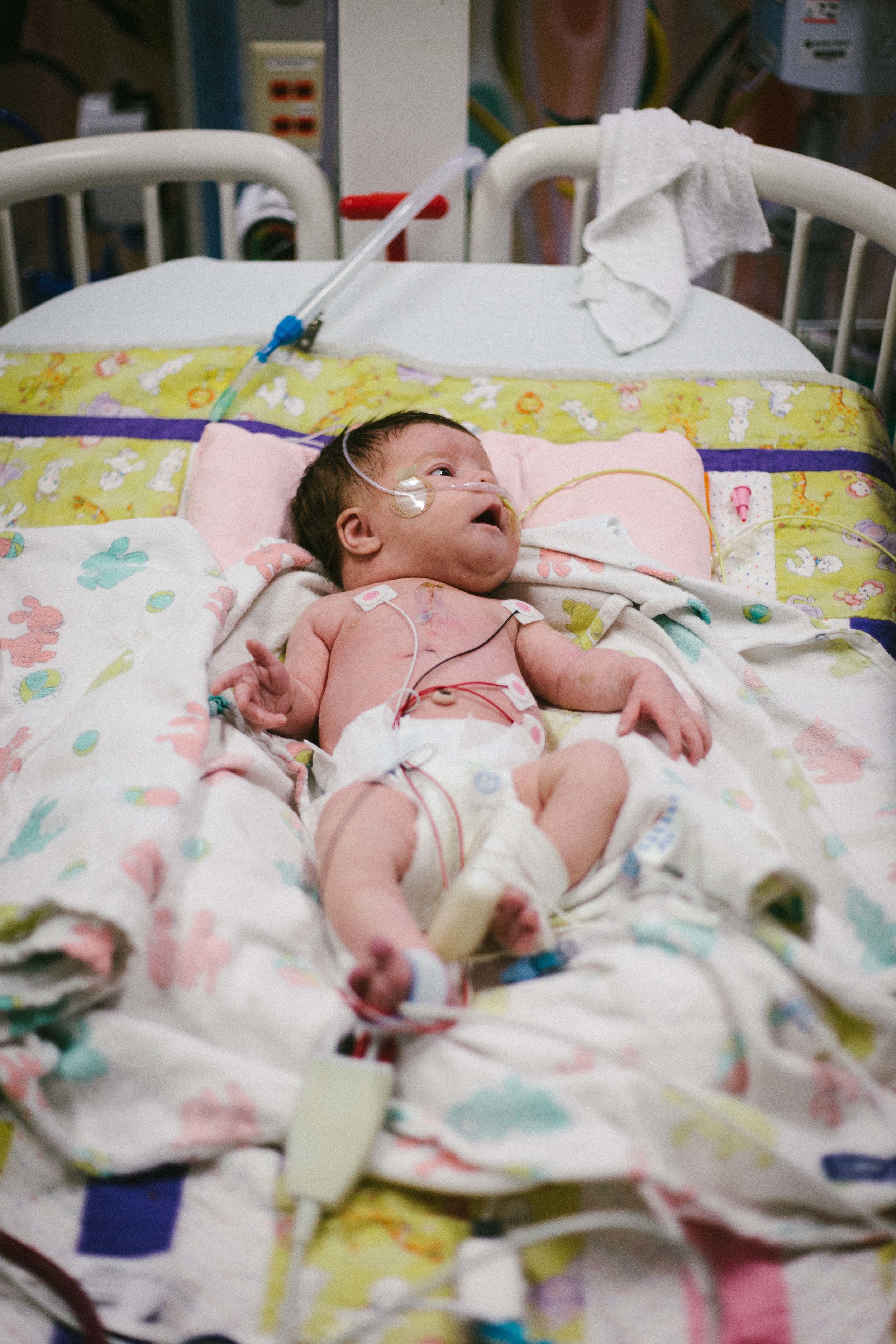

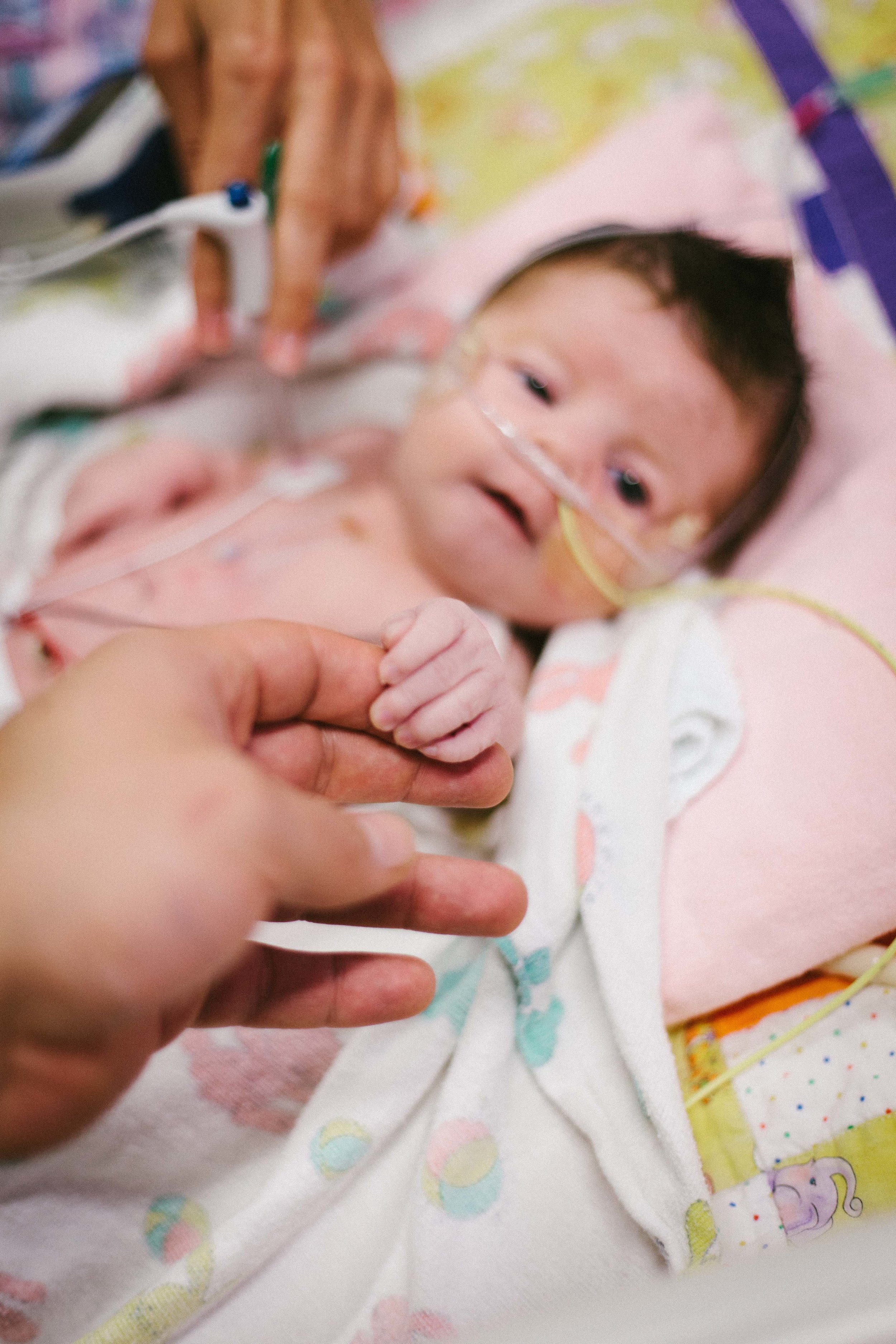
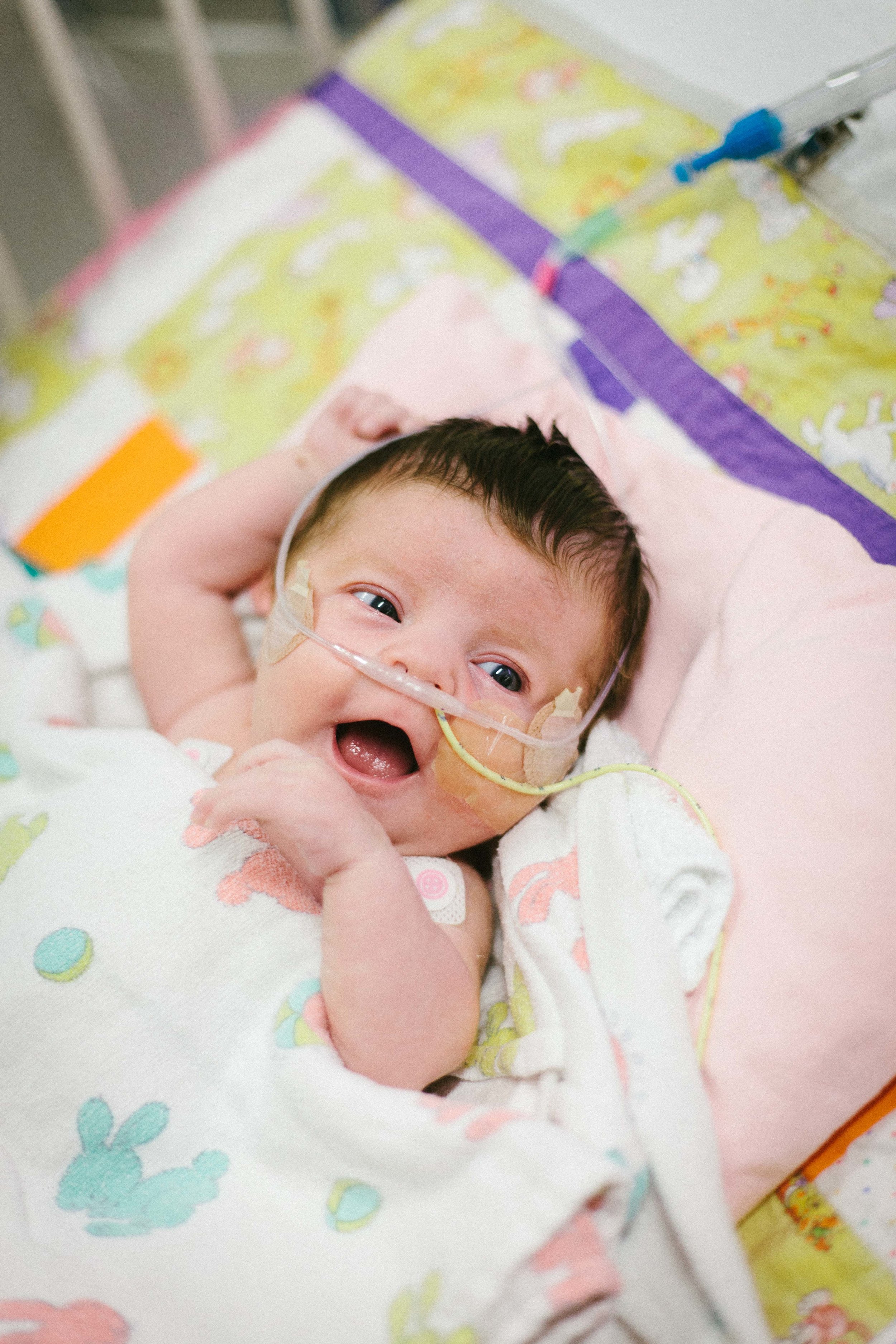
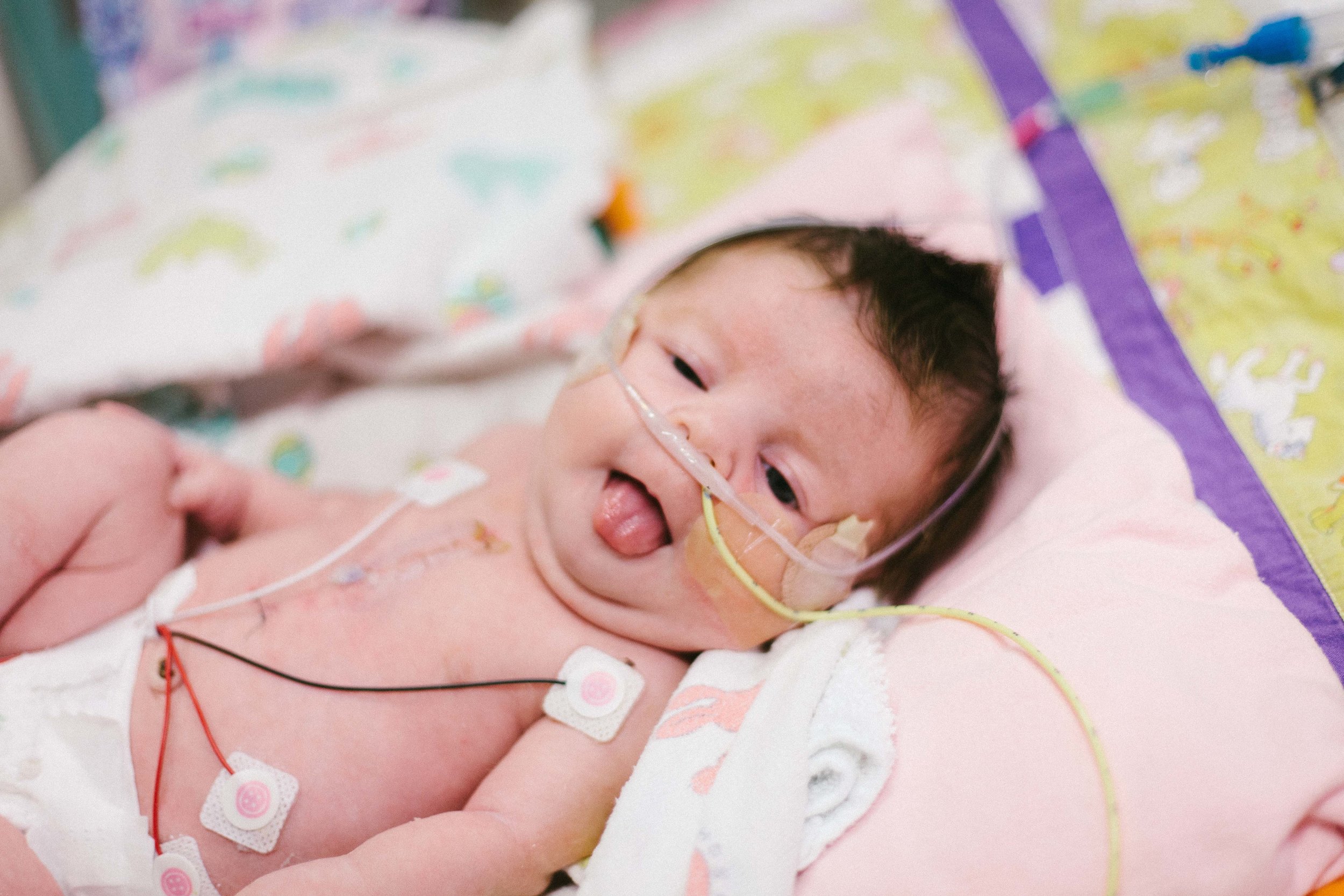
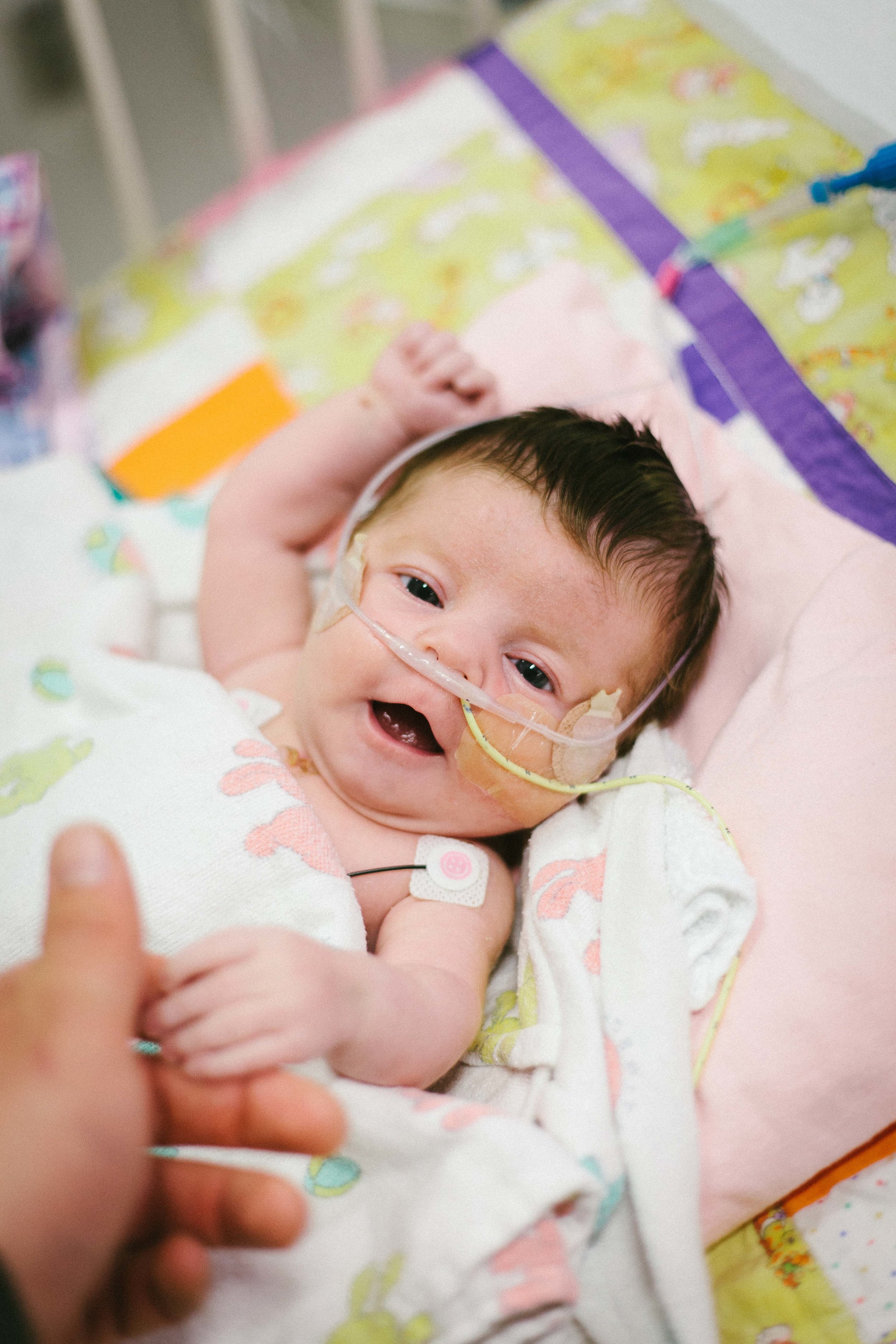

Jail Bird
Shirley had lots of visitors today! My mom's side of the family came and met Shirley for the first time! Grandpa and Grandma Link, Aunt Bronz, and Uncle Hudson came to see her also! The one resounding theme was: she is so much smaller in person.
Today has been a good day for this little girl. They took her PICC out that has been in her right leg for almost the whole time she has been here! They used that line for lots of drugs in the early days and because they are less worried about the need to intervene they felt confident taking it out. It is great to have another limb free of lines. Sure does make it easier to change her diaper.
She was also moved from her infant bed to a crib! She looks even smaller now that she is in a huge crib! It does kind of look like she is locked up in jail though!
She is still doing well on her HFNC at 8LPM and will probably remain there for another 24 hours. Lab results came in for BNP today and she is already down from 3300 to 1500 over the last two days! That was very exciting! Hopefully she continues to trend down.
That's about all for today.
-Joseph
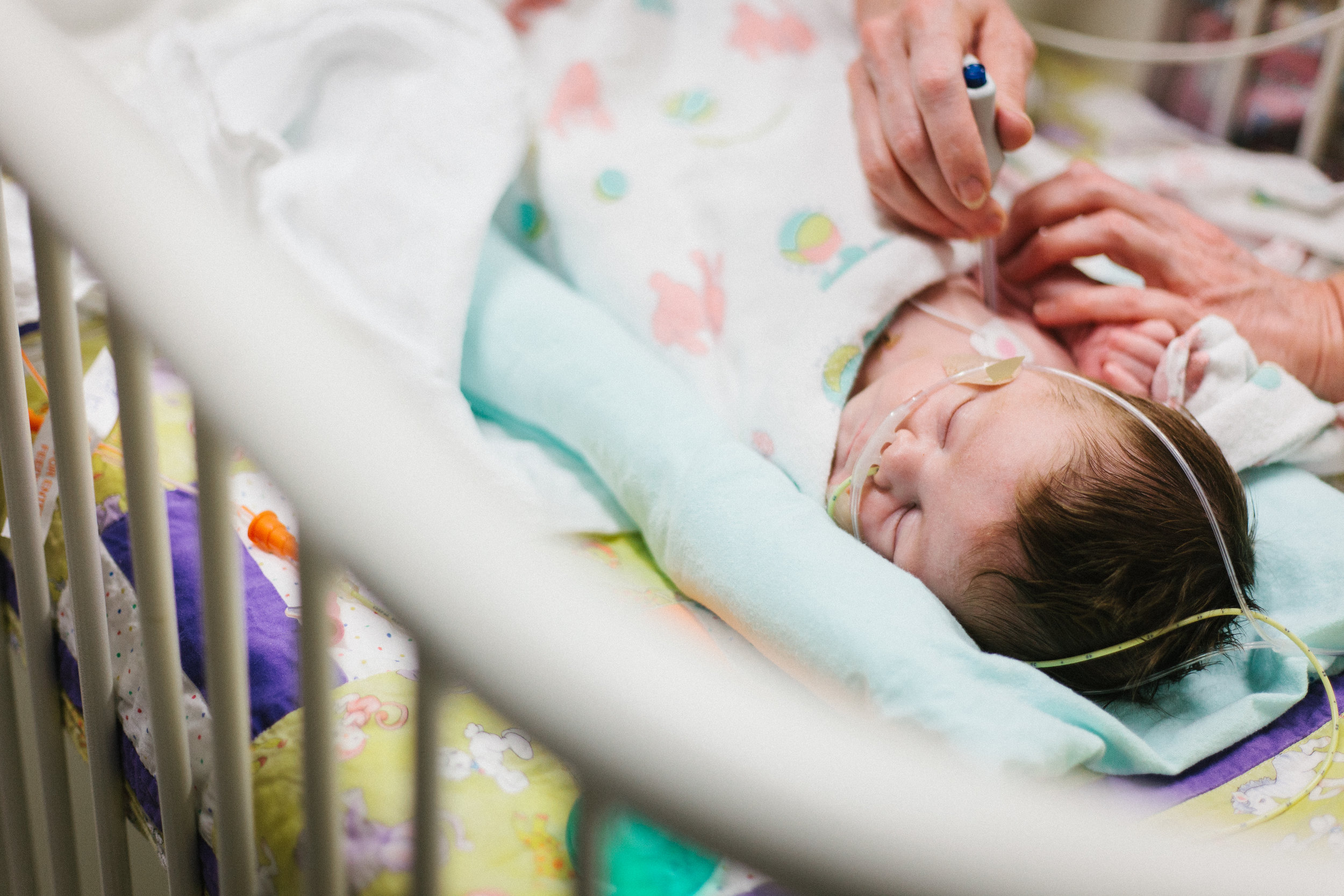
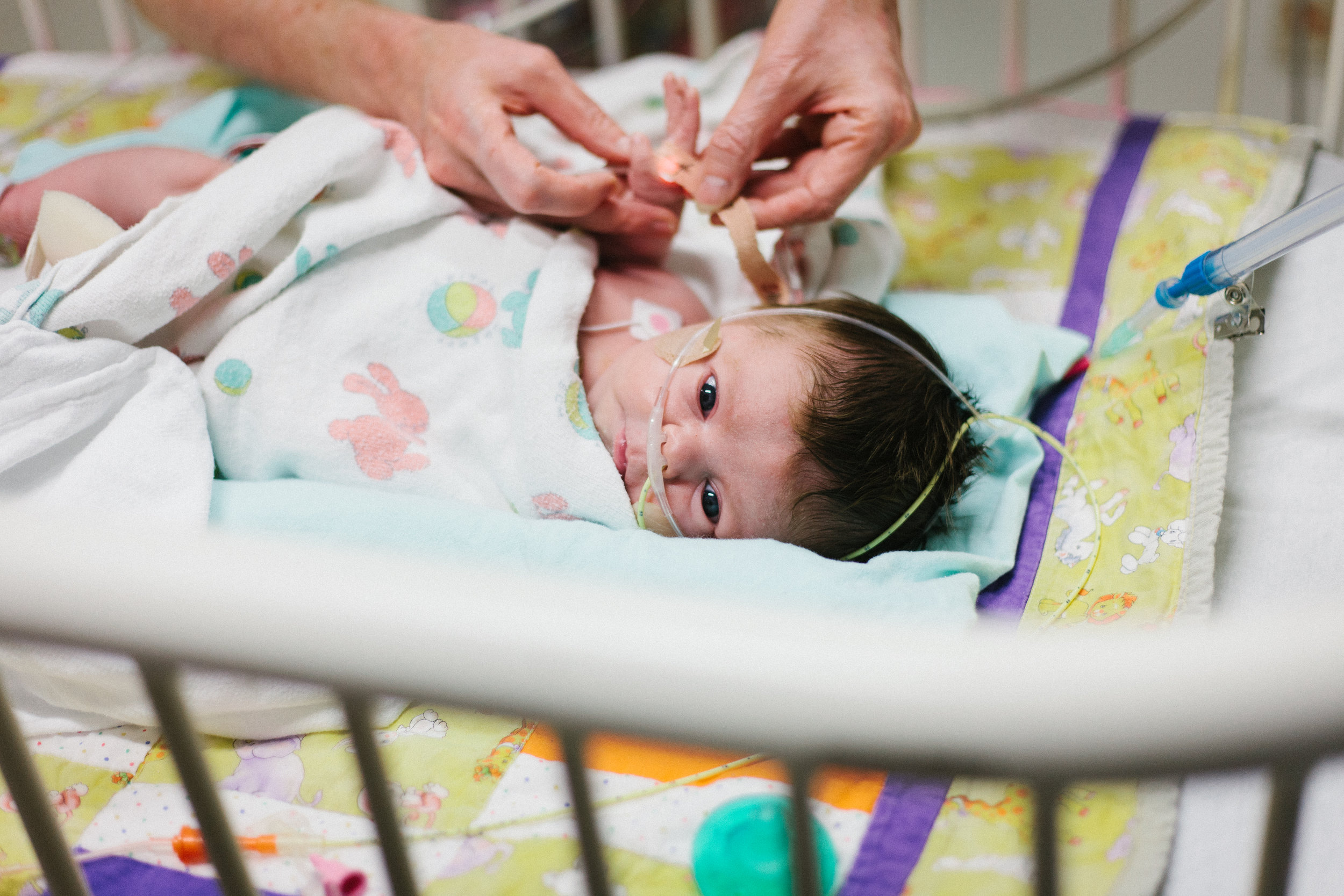
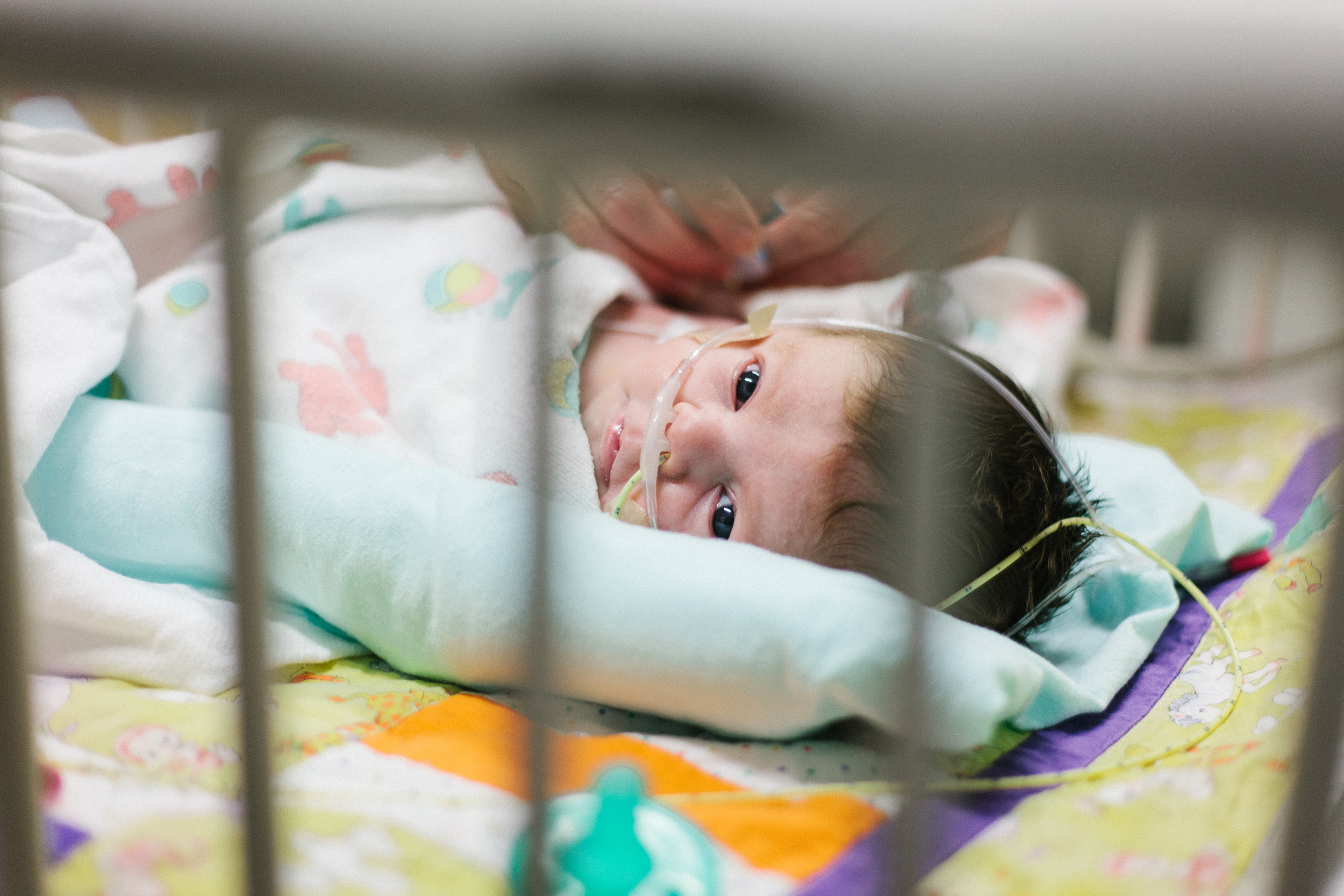
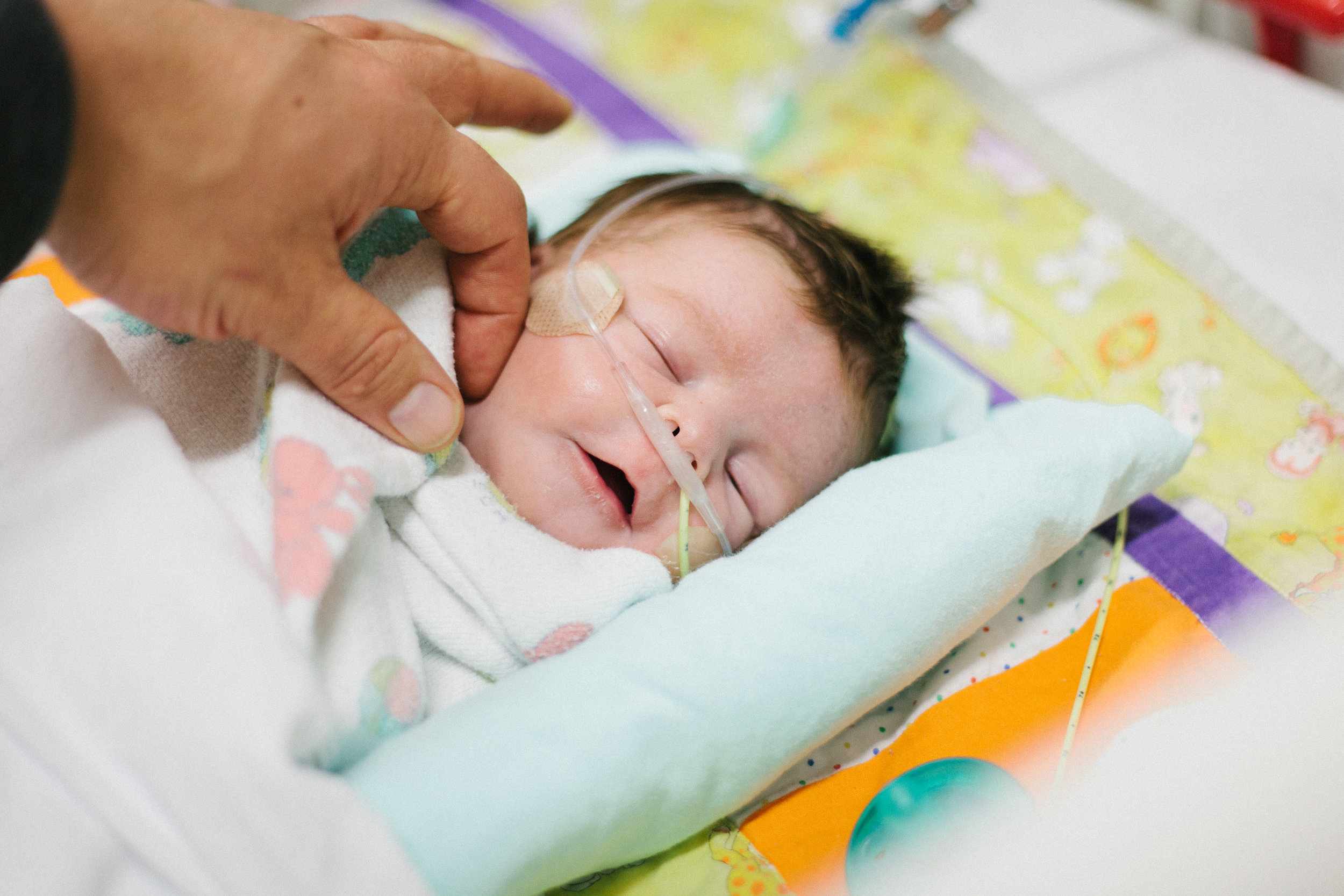

Shirley will tell us when.
"Shirley will tell us when." We hear that a lot! We are still in the CICU and it almost feels like we'll never leave. We may have moved closer to the exit but it was never a guarantee that we would be exiting soon. Just as I said in the last post, on paper Shirley looks like she is struggling but every time the docs look at here in the flesh they see a happy baby that doesn't appear to be struggling.
Her respiration rate has been consistently high since surgery. She takes anywhere from 80 to 100 breaths per minute (BPM) this is called, tachypnea. It would be best if her RR were between 30 to 60BPM. When you watch her chest rise and fall as she breathes you can see that it looks like hard work. Watch the video at the bottom of this post to see what her labored breathing looks like. I've talked about the high flow nasal cannula (HFNC) before and unfortunately I have to talk about it again. She has been on the HFNC since last Sunday and when she was extubated. It is supposed to help her breath a little easier by forcing air into her lungs... They often explain it by saying imagine sticking you head out the window of a car while driving down the road. Neither of those are great explanations but you get the picture. She started on a high flow of 6LPM last Sunday and was weaned all the way to 3LPM within 5 days. It never really helped her RR and today they almost turned it off entirely. The doctors had one last thing up their sleeves though. Turn the HFNC up to 8LPM and see if the added pressure would help. They didn't expect it to do anything and said they thought it would be turned off by midday. Well it worked... her RR has been in the 50's most of the day. Bad news is that you can't leave the CICU until the HFNC is set to <4LPM for at least 24 hours. Since Shirley just started responding at 8LPM its probably going to be a while before she is weaned to <4LPM. The good news is that this will help her lungs. Lots more to say but it just drags on.
Her heart rate has come down to about 150BPM and for Shirley that is pretty good! The drug she is on to help with perfusion is allowing blood to flow to the body easier than it was before and in turn hopefully decrease the amount of leakage back into her ventricle. You learn something new here everyday and we recently learned about a hormone called B-type natriuretic peptide (BNP). When the ventricles of the heart undergo volume and pressure changes, in Shirley's case, blood leaking back into the ventricle, it synthesizes BNP. It functions like a natural vasodilator, decreasing vascular resistance. It's not really a great thing though and is often times used as a predicting marker for congestive heart failure. Don't go freaking out! Shirley isn't in heart failure territory but she has elevated levels of BNP and its worth keeping an eye on. Her concentrations are about 20 to 30x higher that the average neonate. Some of this is to be expected but its still rather high. The hope is that it will trend down over the next few weeks and be a marker for her recovery. Just have to wait and see.
So we'll wait for Shirley to tell us when she is ready to leave the CICU. This may seem like a negative post but its really not. Shirley is doing well! She is only on two drugs right now Lasix and Captopril. That is almost nothing compared to what she was one after surgery. If Shirley were really struggling they would be intervening much more.
Please keep Shirley in your prayers.
-Joseph
Just pictures today!
No lengthy update today.
Shirley is doing well. Still in the CICU because, in short, on paper she looks like a struggling heart baby and in person she looks like a rockstar. She is a confusing young lady.
Please keep praying for little Shirley.
Here are some pictures from bath time today!
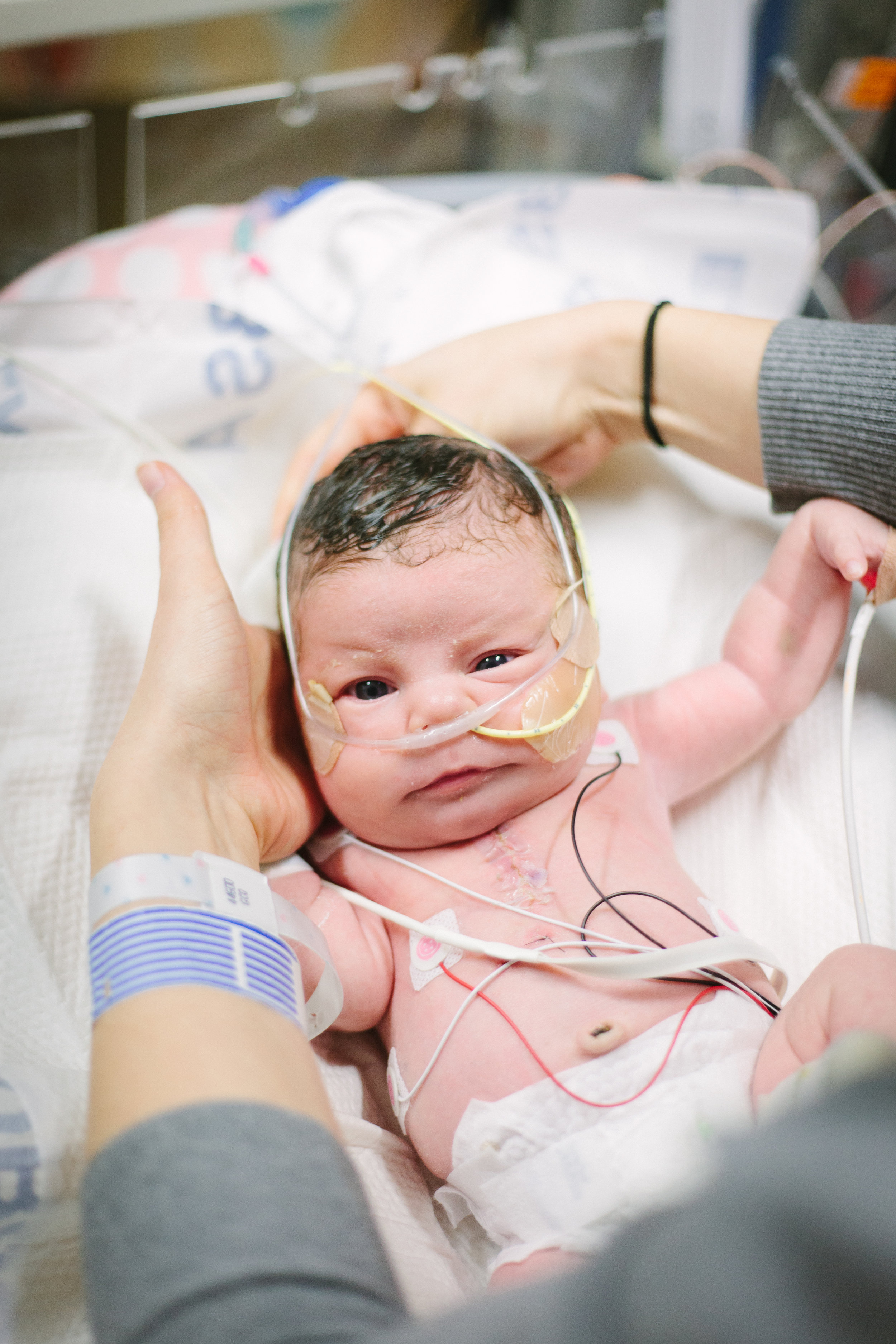
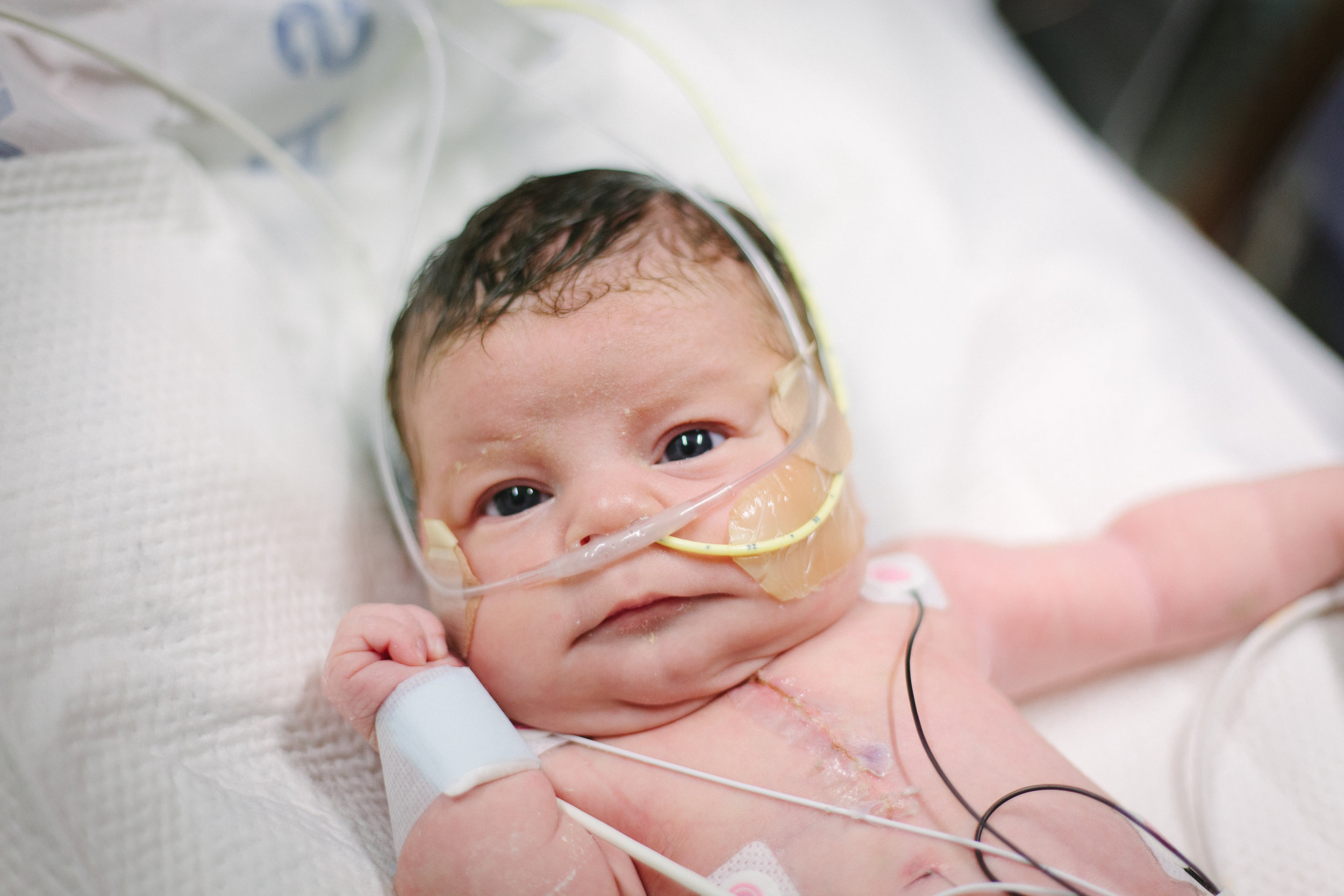
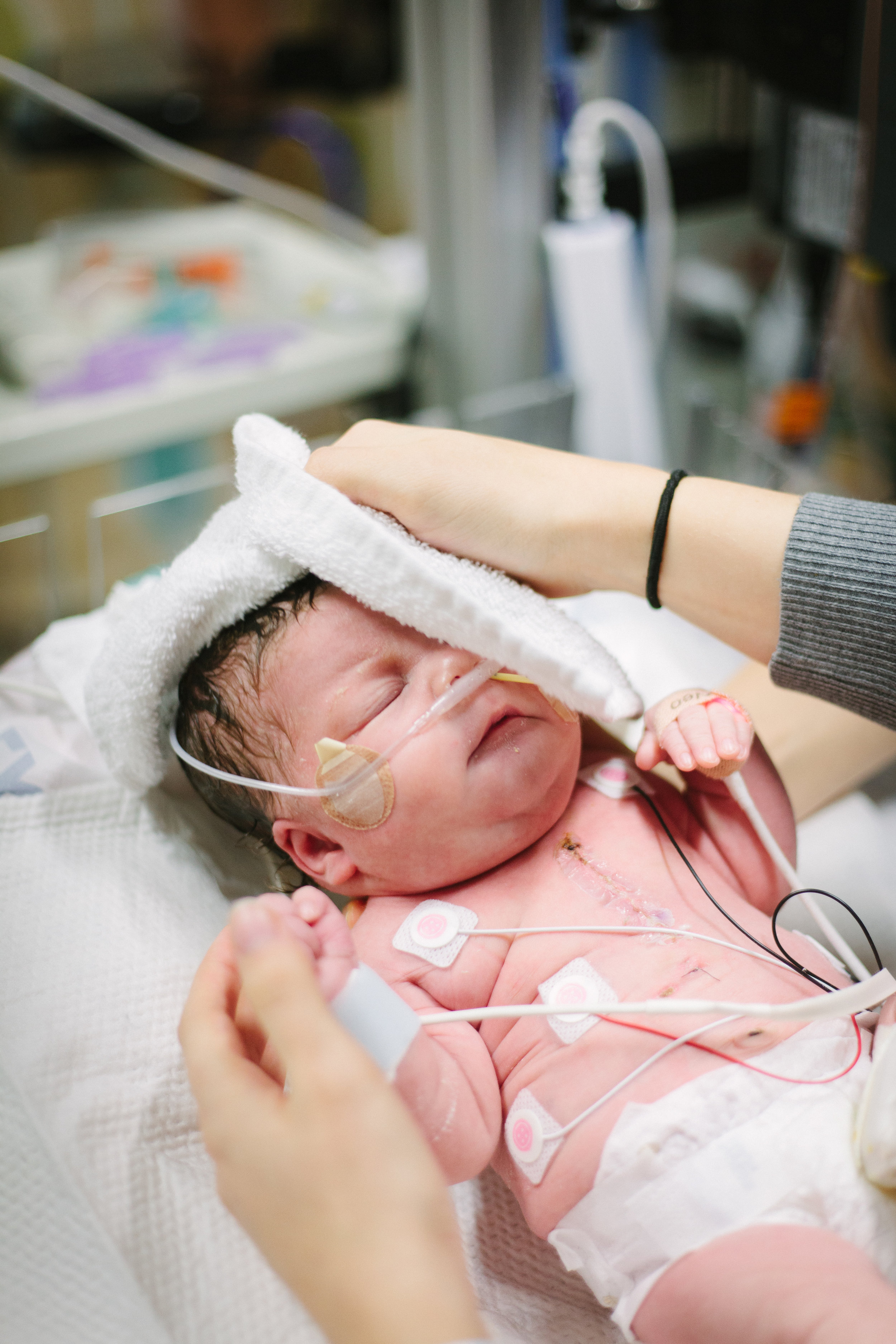
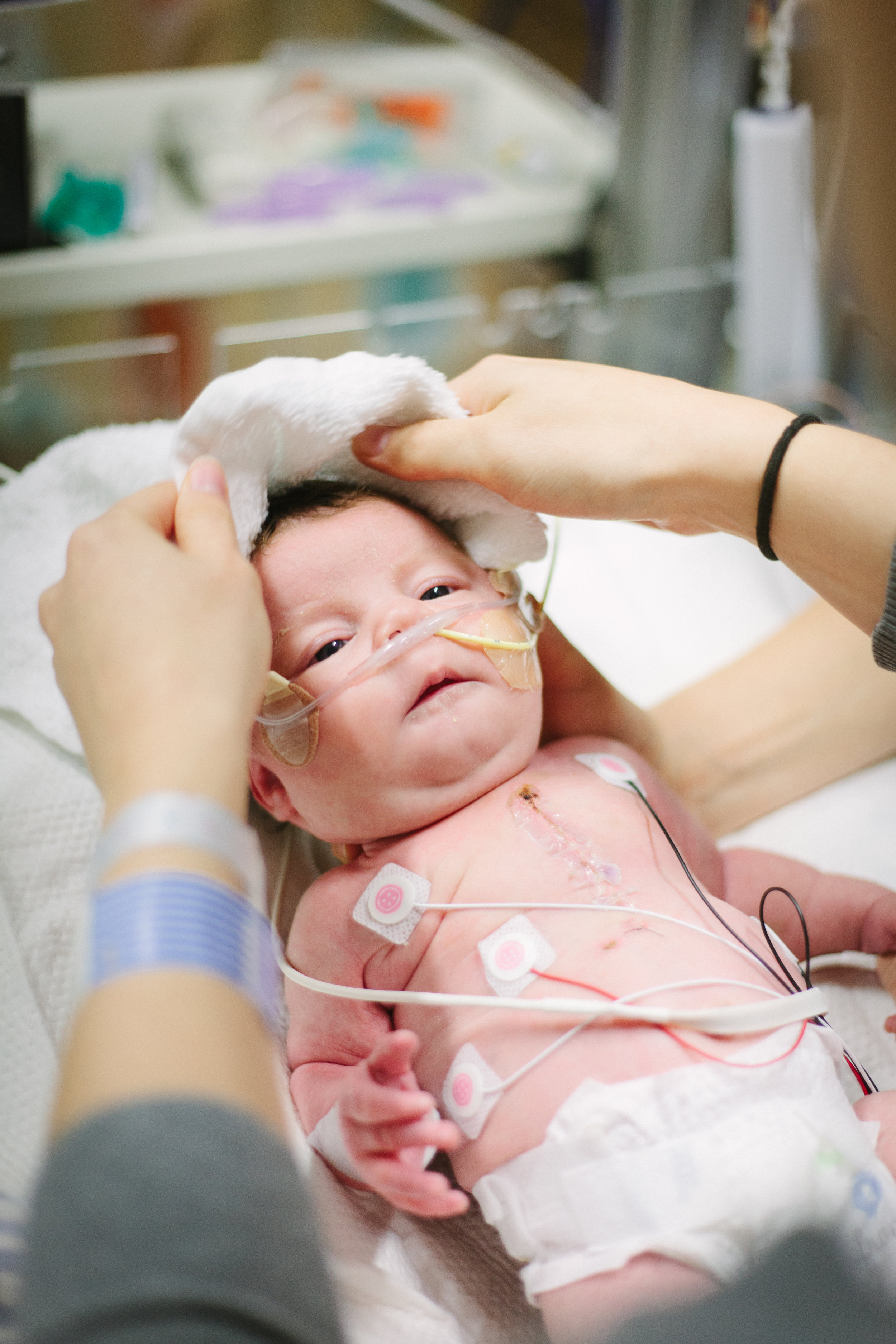
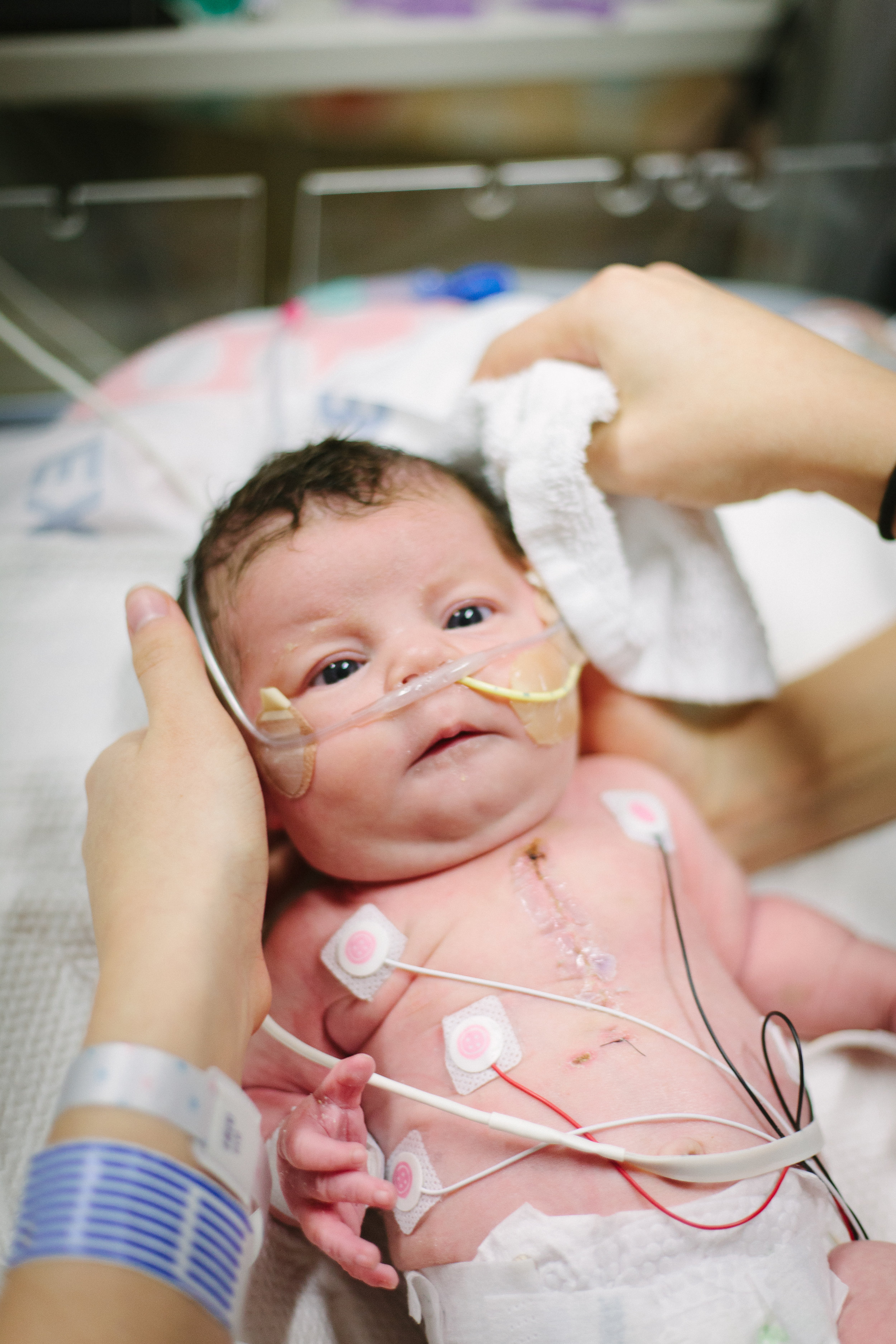
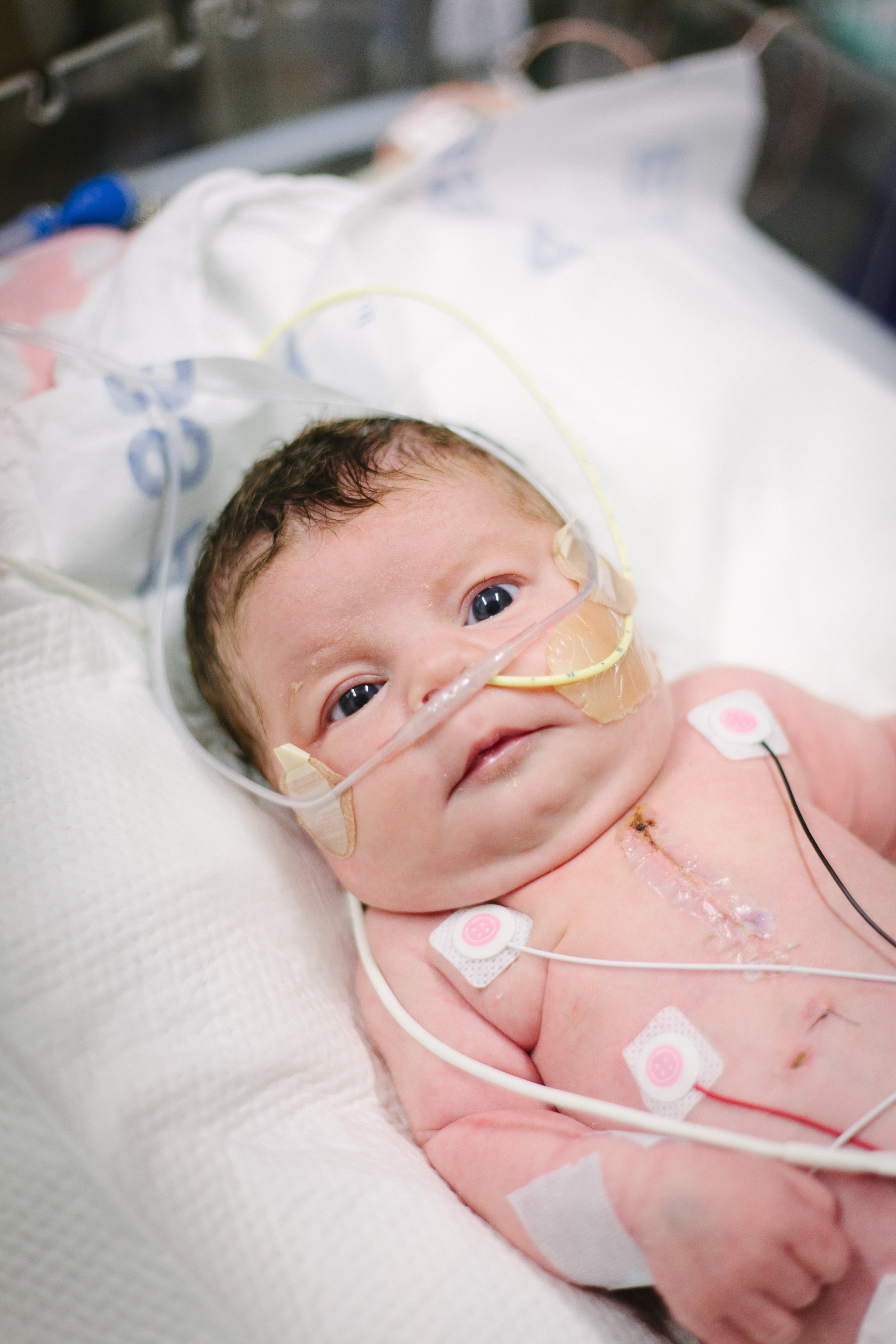
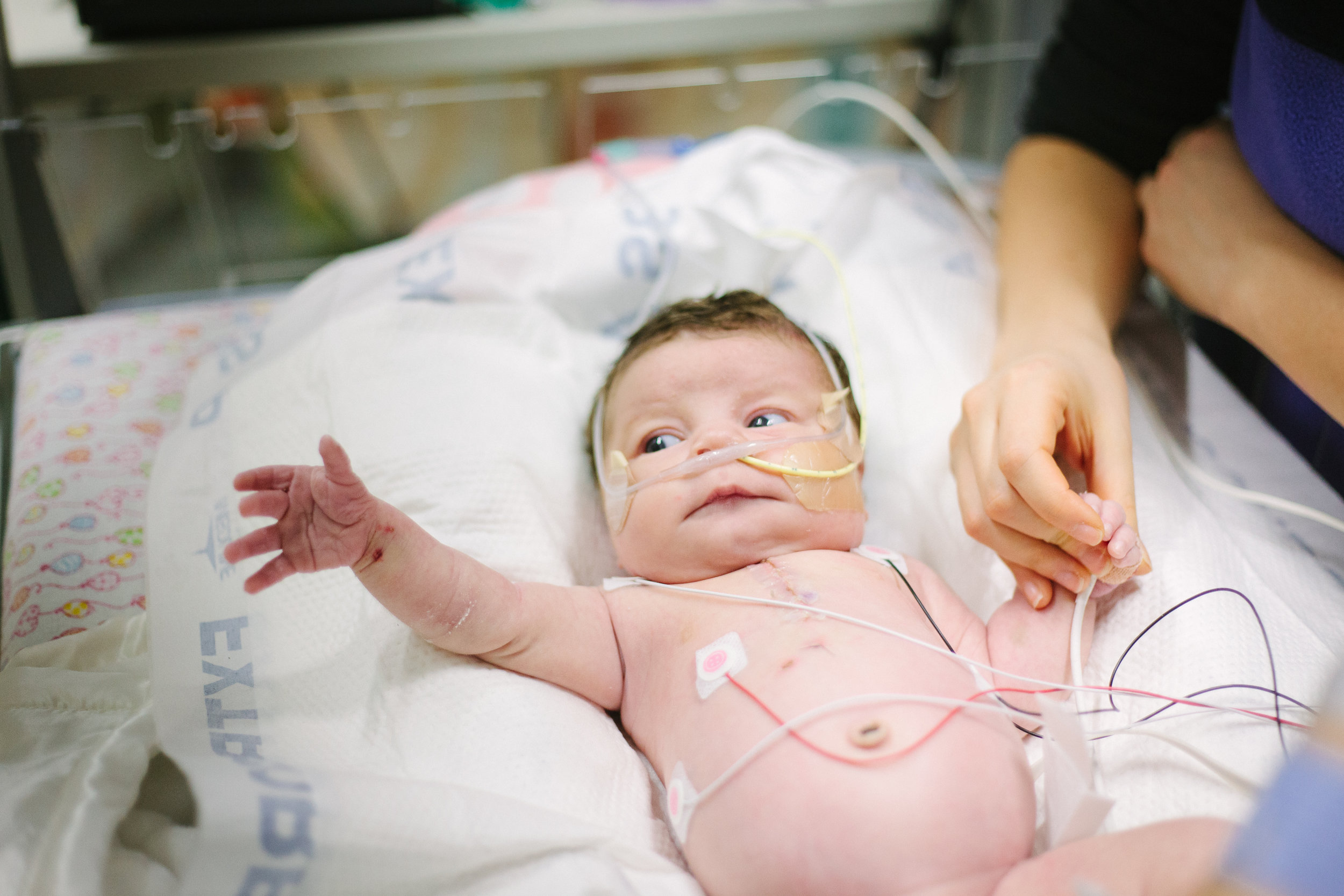
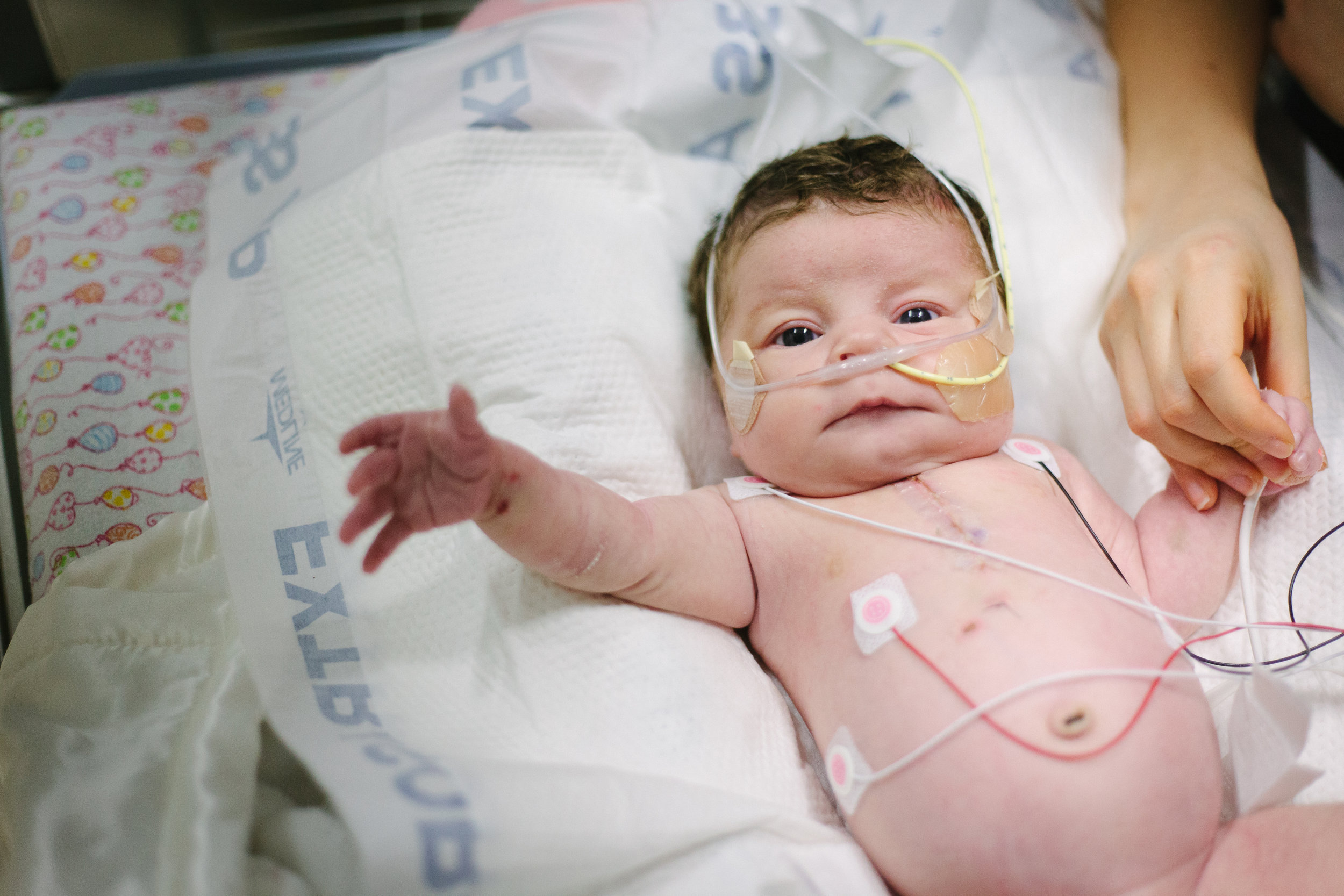
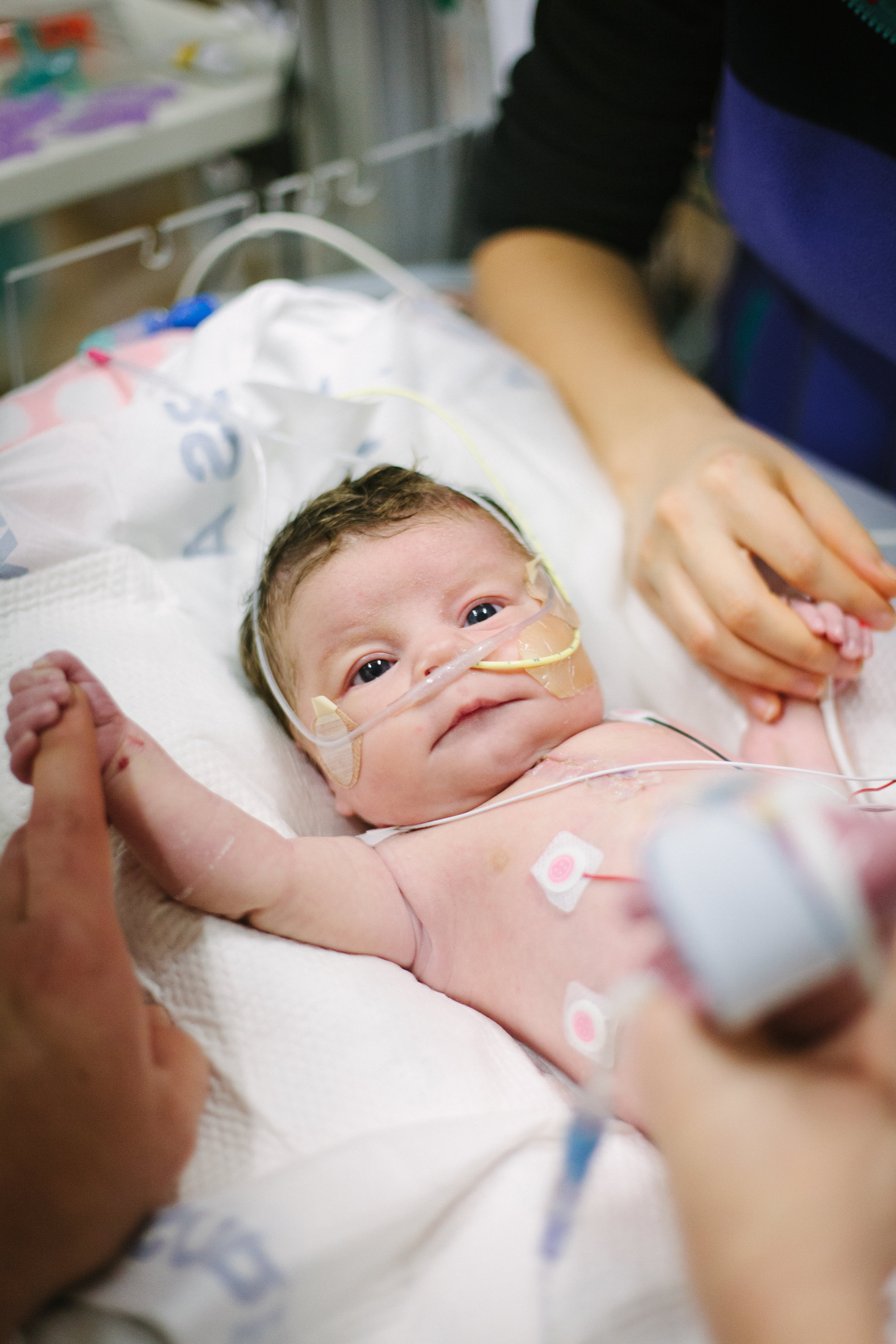
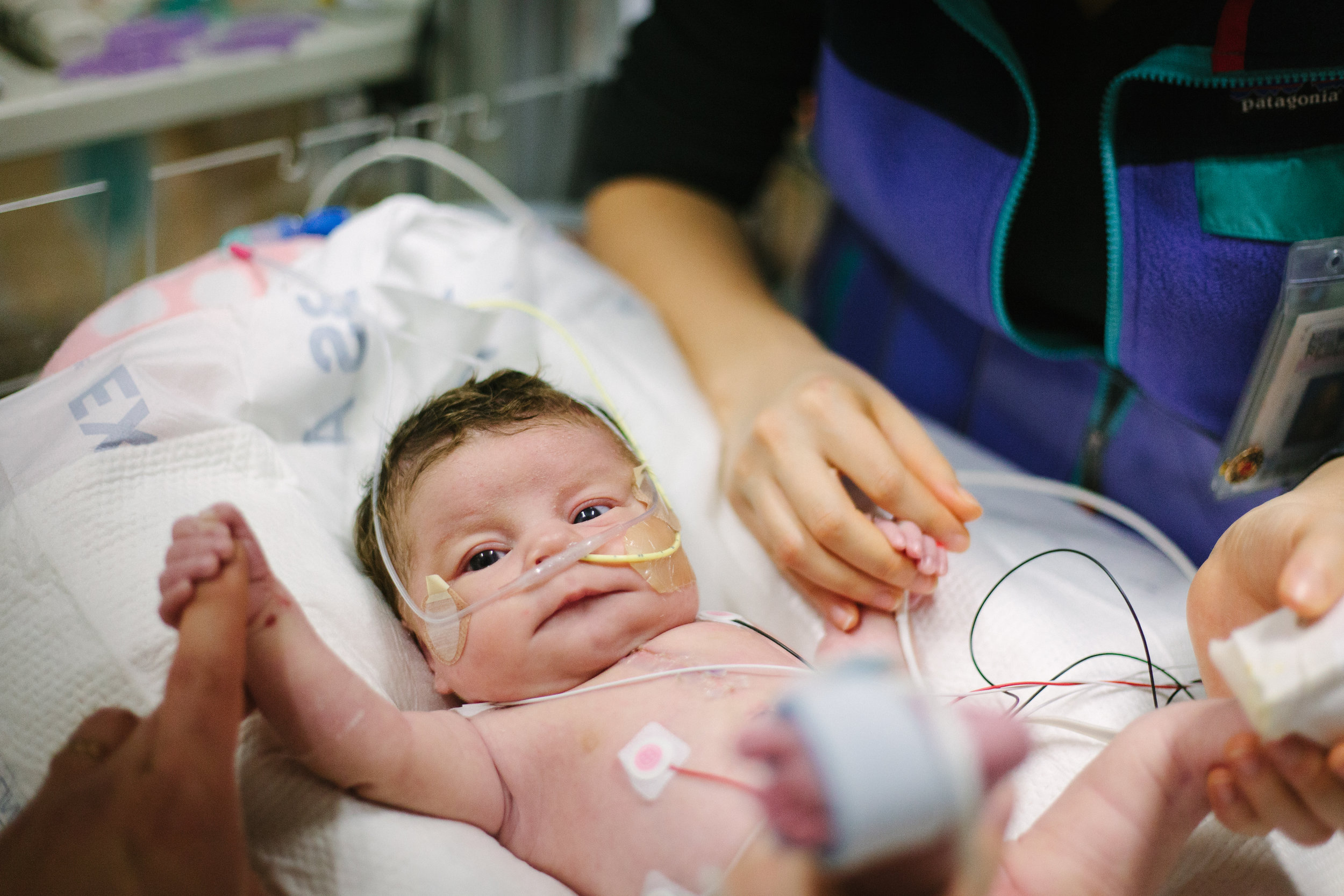
Two Weeks!
Can you believe it?! Shirley is already two weeks old! Let's do a small recap:
Born at UW Medical Center on 2/23/17 at 7:29pm, 7lbs 8oz, 18.5inches long! Then promptly transferred to SCH and admitted to the CICU. Surgery on 2/28/17 to make the initial repair of her truncus and patch her VSD! Chest closed on 3/2/17. Switched rooms on 3/6/17. Made her debut television appearance on 3/7/17!
Today, 3/9/17 is a pretty straight forward day. She is off milrinone entirely, down to 3L on high-flow, and fluid neutral. All great signs! There is a chance we will be leaving the CICU tomorrow (fingers crossed). She met her nutrition goals yesterday evening and is fed Brianna's breast milk fortified with some extra calories. They fortify her milk because heart babies burn more calories than they take in during their recovery from surgery and often times breathing and plain ol' living are more strenuous. She is still at her birth weight but if she keeps up this pace she will be plumping up in no time!
Shirley had her first appointment with the OT/PT's today. One of many. I think I mentioned in the last post how these little ones are behind the average child when it comes to early development. The instinctual things can be difficult and being two weeks behind is a long time for an infant. Today it was "oral skills." Suckling, swallowing and breathing are difficult and Shirley fought off the OT pretty hard today. She was also very tired and you will see some of the attempts at waking her up in the pictures I post. Her future OT/PT visits when we get home will be helpful in many other ways. Because their movements are restricted for so long after surgery its helpful to work on their range of motion down the road as well as other general baby skills like rolling over and other things that would have just come naturally. Pediatric heart surgery has come a long way and these days their is a focus on thriving after surgery rather than simply taking your baby home. The world of CHD is changing rapidly and there are a lot of people to thank for that. We owe a lot to the cardiologists, surgeons, nurses and endless other medical professionals but also the parents and other CHD babies who have helped pave the way to where we are now. Hopefully in a few more years the experiences of future heart babies will be even brighter than they are today.
Shirley had some visitors yesterday aunt Jen, aunt Mary, and aunt Brittany! It is such an interesting phenomena how infants can be an attraction and even a spectacle! Shirley, like most babies, sleeps the majority of the day yet all you want to do is look at her... anticipating, hoping, that she will move, smile, smirk, cry, suck on her pacifier, twitch, stretch, or maybe even toot. Babies get all the attention, I can't really explain why I want to look at her toes, nose, and elbows but I do.
Please continue to pray for little Shirley!
I also think Shirley is photogenic and here are some pictures to back up that claim. These are all from this morning when the OT arrived and we had to try and wake her up. hope you enjoy.
-Joseph
Slowing down.
Yesterday was a big day for Shirley! She was on the news and she was getting used to a new room in the hospital. Today during morning rounds the docs had some concerns about Shirley's heart rate overnight. She had another bout of tachycardia yesterday so they are watching it closely. They are still trying to wean her off some drugs that help her heart to pump but they also are adding a drug to help her perfusion. Seems like they're robbing Peter to pay Paul to me... but what do I know? There is some confusion as to why her numbers are the way they are right now but its nice to have so many great minds come together trying to figure it out!
We have a consult with occupational therapy soon to help Shirley with oral skills. Most babies don't need to learn how to breastfeed and if they do its something that takes place relatively naturally. There are, however, children that have difficulty or will never be able to breastfeed. Because Shirley was fed intravenously for 10 days she never really had the chance to learn these "oral skills." The goal now is to teach her how, with the hope that some of the instinctual behaviors will be resurrected and she will be able to latch and suckle normally. She has responded well to the pacifier and we know she wants to suck but it can still be difficult to transition to the breast.
Right in the middle of writing this she had another episode of tachycardia. It was not a very fun sight but it was so brief that she calms down rather quickly. It was good that it happened during the day while we were here so the docs have a solid time stamp for the event rather than seeing it after the fact. They are analyzing her rhythm now.
It looks like we'll be in the CICU for at least another 24 hours (probably longer).
Thank you everyone who has offered to help with our home break in. A lot of people have offered their televisions and the like but we are currently just trying to focus on Shirley and will be dealing with the material things at another date. Again, thank you so much for the support!
Here is a video of Shirley giving us a cute little smile!
-Joseph
Breaking News: Shirley's Story on Q13 Fox Tonight!
Q13 Fox contacted us out of the blue today and said that they had heard about Shirley's Grand Adventure as well as our break in and decided to do a last minute news segment on her!!! We couldn't believe it! We don't know what it will consist of yet but Brianna and I sat down with a reporter for a short interview that will air tonight at 9, 10 and 11pm on Q13 Fox! Shirley is already turning heads! Now back to our Usual broadcasting!
We changed rooms but Shirley is still in the CICU. They moved us down the hall to a room near the exit and for her its literally because she is headed that direction. From what we understand they keep the more critical children towards the far side of the unit; Doctors have the quickest access there. They keep the less critical children, Shirley in our case, towards that front of the unit. The move is just a sign of Shirley's progress.
Last night Shirley did have a bout of tachycardia (when the heart beats very fast) but the doctors weren't overly concerned. Remember, Shirley's heart is far from average and some of the drugs she has taken or still is taking can have many side effects. They think that this is probably the case with her and that it will not be an issue she struggles with in the future. Her heart rate maxed out at 220bpm last night but like I said, it was short lived. Her baseline heart rate is already higher than the average infant so its even less concerning. She is being weaned off a drug that helps her heart to work more efficiently. They also plan to take her off the TPN (corn syrup and salt) because she is being fed Brianna's milk at a rate that will really nourish her! Shirley had a central line in her neck that leaves a very short trip for meds to get to her heart or whatever they decide to administer. They took that out yesterday evening! She is slowly but Shirley ;) getting back to normal!
Our wonderful host keeps going above and beyond for us. She has bought us dinner and cooked us breakfast sandwiches multiple times. We feel very blessed to have landed where we did with no prior knowledge of her and going with the cheapest option for housing! Today she offered to do our laundry!
Nothing new about the house but we have continued to have people ask us what we need and to be honest we don't need any of that stuff that was stolen and aren't very concerned about it currently. None of Shirley's baby stuff was stolen, go figure, so we have what we need to bring our daughter home when its time.
Last but not least! I held Shirley for the first time in 8 days today! The day of surgery I thought it would be best for Brianna to get as many snuggles in as possible and post surgery I thought the same. Now that Shirley is easier to maneuver I can make up for some of the time I missed out on cuddling my sweet girl.
Here is a picture of me holding her today! The news clip is also attached below.
This is a news story done by Q13 FOX in Seattle about our daughter Shirley!
On the mend!
Shirley has been doing well in the short time she has been off her vent! They weaned her off morphine and her other sedatives. She is alert and happy. She had quite a bit of snuggle time with Brianna today which is always nice. The other big news is that she pooped! This was her first bowel movement after being fed breast milk so it a pretty good sign that her gut is doing its job. She had another echo today to get a good look at her heart post surgery. What used to be her truncus is now her aorta which can cause some issues but nothing too serious. She did get a blood transfusion today to replace the blood they take for labs and such. Her vitals went up immediately after receiving some new blood and they have stayed up since.
I was able to go and survey the damage at the house today and was glad to find that pretty much everything that was taken is easily replaceable. There have been a couple leads already with the help of some Apple software allowing the police to track the iPad. Hopefully this will lead to getting some of our stuff back. While I was in Tacoma trying to figure everything out I received a call from TPD letting me know that a woman had found some random documents in her garbage can today. Lots of personal information and Brianna's passport turned up in there. The officer dropped them off to me just before I headed back up north to see Shirley. Thankfully we have a lot of people watching the house so this shouldn't happen again.
Thanks for the continued support and prayers! Many people have already offered to replace our material possessions. We are certainly going to wait before we buy anything new but from what I calculate we lost less than $1000 in possessions. I'm kind of cheap when it comes to electronics so everything that was stolen was bought used. We haven't even had a television that long and didn't have one the first year of married life so maybe this is just a sign that we don't need one.
-Joseph
Extubation & Break in
Shirley is doing well, she is off her ventilator. This is great news. She is back on a high-flow but they expected to still need some breathing support after she was taken off her vent. She is also much more aware! She is looking around a lot! It so great to see those pretty little eyes looking back at you! She is making good progress so hopefully we will be moving out of the CICU within the next few days!
Unfortunately though we found out that our house has been broken into. We aren't sure when it happened but it certainly happened! My in-laws stopped by the house today to pick some stuff up and bring it to us but when they walked in the door the house was a wreck and there was no mistaking it. Our house was plundered with all the usual stuff missing: TV, iPad, DVD player, tools, and who knows what else. Hopefully we will be able to get back soon and do an inventory of what is missing. Sometimes things just don't make sense. Please keep our family in your prayers as we now try to tackle how to deal with the break in on top of little Shirley's issues.
Sometimes when it rains it pours. The sun always manages to come back out and brighten things up though. We look forward to bringing our wonderful little daughter home and expect that good can come even from a robbery. We have a strong belief that all things happen for a reason and that we will truly find good in all of these trials. Thanks for your prayers.
Here are a couple of pictures! One from last night and one from this afternoon. We had a wonderful nurse last night who thought it would be okay if Brianna held Shirley for a few moments while she changed her bedding! It was a chore getting everything situated but we managed! That was the first time Brianna had held her since Tuesday! The last one was taken only a few hours ago right after she was taken off the vent!
-Joseph
Post-op day 4!
Big day for Shirley! She did well last night! She could have done better but we celebrate just about anything!
Shirley will have to remain on her vent for at least 24 more hours, but today she will receive breast milk through her NG tube for the first time! This feels like a huge win! There is of course some risk that she will not tolerate the milk but the cardiologist thinks she is ready and the nutritionist didn't have any objection. They will measure her stomach on fixed time intervals in order to determine if she is digesting the milk properly. They also want to take her drainage tubes out. She has two tubes placed in her chest currently one was placed after the surgery to help drain excess fluids and one placed when they closed her chest that drains fluids trapped behind her heart in her pericardial cavity (I think). Both have functioned well and drained a substantial amount of fluid. Whatever fluids are left to drain will be absorbed by the surrounding tissue. They will also be weaning her off the vent. She is still breathing beyond the RR the machine is set to but the vent is providing some support inflating her lungs as well as providing nitric oxide (NO) to lower the blood pressure in her lungs and in turn take some burden off the heart. The doc said that weaning is the easy part and that most children handle it well; it is from 1ppm to 0 that they tend to struggle with. She is currently receiving 2.5ppm and they plan to be at zero by sometime tomorrow morning. They are also removing her pacer wires. She hasn't needed them yet so hopefully she won't need them later! It is a big day for little Shirley.
We spoke with another family today that arrived the same day we did, their child was taken off the vent yesterday and they are moving out of the CICU today. Hopefully this will be the case with Shirley in a few days. The step-down unit is like having one foot out the door of the hospital. We are excited about her progress and can't wait for the day we can walk out of the building with her, strap her in the car, and head south to Tacoma. It will probably be a journey on par with Frodo's return to the Shire! Not sure why I thought of the Lord of the Rings and the Shire but it's just what came to mind when I thought about taking my girls home!
Please feel free to critique my medical jargon! I know there are at least a couple Dr's reading this, a few nurses, and perhaps even a respiratory therapist. Comments section below!
The first two photos were taken today and the last two a few days back.
-Joseph
Post-op day 3 +
Shirley is continuing to make progress. She has come a long way for having only being born 8ish days ago. She is still intubated and likely will remain so for a few days. The Dr's hoped to be able to get her off earlier but her little body is fighting against it currently. She is retaining too much fluid and until she can balance out and perhaps go a little negative they'll keep the ventilator running. Its a very complicated thing to balance her nutrition, drugs, and fluids. Hopefully she will be able to come off the vent soon enough and start introducing milk to her diet. Feeding is still a risk the cardiologists aren't willing to take. If her gut does not get the blood and in turn oxygen it needs feeding milk would only complicate her issues. Currently she is on "Total Parenteral Nutriton" (TPN). This is supplying some basic nutrients such as: water, sugar, electrolytes, ect. She is also on a Intralipid (fat) drip. This supplies fats directly to the bloodstream. After just a little research you find that Intralipid is mostly water, soybean oil, egg yolk phospholipids, and glycerin (pretty sure its used as an emulsifier). Kind of depressing that soybean oil is the go-to for lipids. There may be some research that says soybeans are the best source of lipids for these purposes but I have a feeling that is not the case. Dextrose is the primary sugar used in TPN and you guessed it... corn based. Crazy to see how big agriculture is literally everywhere. Both of these are not ideal options but they are necessary post surgery. The docs and nutritionist are hard at work to get her milk as soon as possible!
Sorry, if that post was more than you wanted to know about her nutritional intake but thankfully she is doing well enough that I don't have to talk about something more serious! Also, my mention of big agriculture, corn, and soybeans is not politically motivated. I was just intrigued by how pervasive these things are.
Lets forget about all that nutrition talk and admire how cute Shirley is. This one taken a day before she went under the knife.
-Joseph
Post-op day 2 and Zipper Club
Great news! Less than 48 hours after surgery Shirley's chest was closed! She is now officially a part of the "Zipper Club." The surgeon had prepared us for 4 to 5 days of her with an open chest but due to her swelling dispersing quickly they were able to sew her up around 11am this morning! Her next big hurdle will be coming off the ventilator. She is currently intubated through her nasal passage in order to provide mechanical ventilation. In short she is hooked up to a machine that breathes for her. In her case, however, its simply used as a backup for her own respiration. She has consistently exceeded the minimum respiration rate (RR) that the machine is calibrated to. Its kind of like a pacemaker if she falls under the set RR then the machine will take a breath for her. Hopefully it will come out soon! Please keep praying.
Hopefully everything keeps going according to plan and she will be on her way out the door of the hospital in no time. Well, not no time, but maybe a couple weeks!
We were fortunate to have our pastor and intern pastor show up and visit us today with encouraging words from our church community and to pray for our family! Grandma Anne stopped by after an appointment in Seattle, unfortunately none of the visitors were able to see little Shirley due to her procedure but we appreciated the company.
Here is a picture of Shirley shortly after her chest was closed.
-Joseph
Post-op day 1
Shirley had a great night! Her nurse, one that has been caring for her three evenings in a row, said that she did almost nothing but monitor our little one. Lots of things went well: little swelling, stable blood pressure, and she's responding well to her drug cocktail. She is on the minimal amount of support that a post-op might need. A lot of her care and purpose of the machines and drugs are to allow her heart and lungs to rest as much as possible. So many things have to come together in order for Shirley to be comfortable and still functioning properly. It has been amazing to see how this technology works and how it is benefiting our little girl.
Thank you all for your prayers and support! The next few days are a very critical time for Shirley but they may also be a very uneventful time. Shirley is just laying on her little bed and she cannot be held until they close her chest. We are looking forward to them weaning her off some of the pain meds so that we can interact with her. I can't wait to see those sweet little eyes starring back at me again!
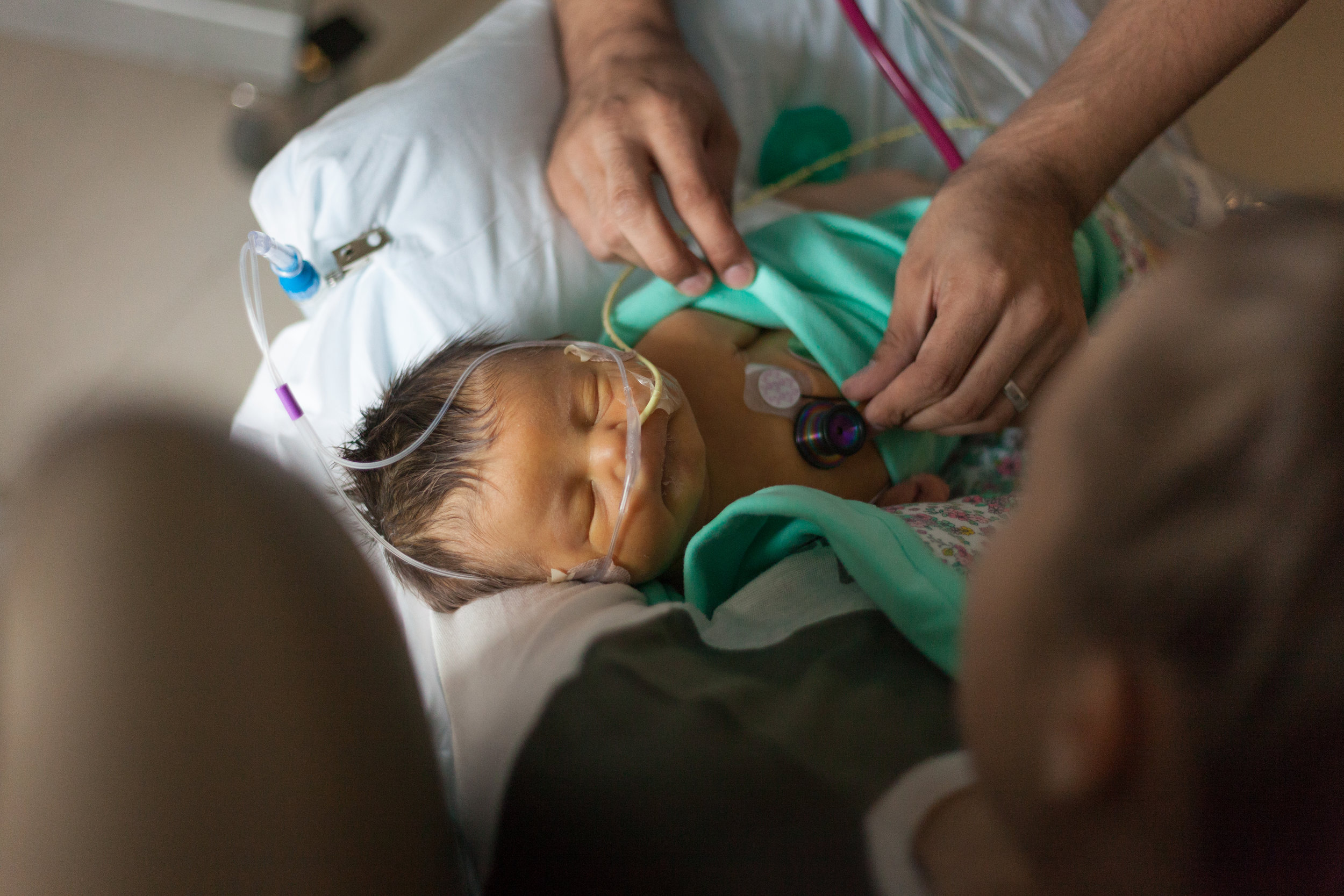
Here are a couple photos of little Shirley. The first one is of a nurse that we've had going on 5 days now. She spends 12 hours a day caring for little Shirley and us! We have developed a wonderful relationship with her and she has already earned the title: Aunt Viv. Aunt Viv has pulled strings and manipulated her schedule multiple times in order to be Shirley's primary nurse. The last two photos were taken just before surgery when a wonderful Dr. came to check Shirley's vitals. I was moved by how gentle he was and couldn't help but get a few pictures.
-Joseph
Out of surgery
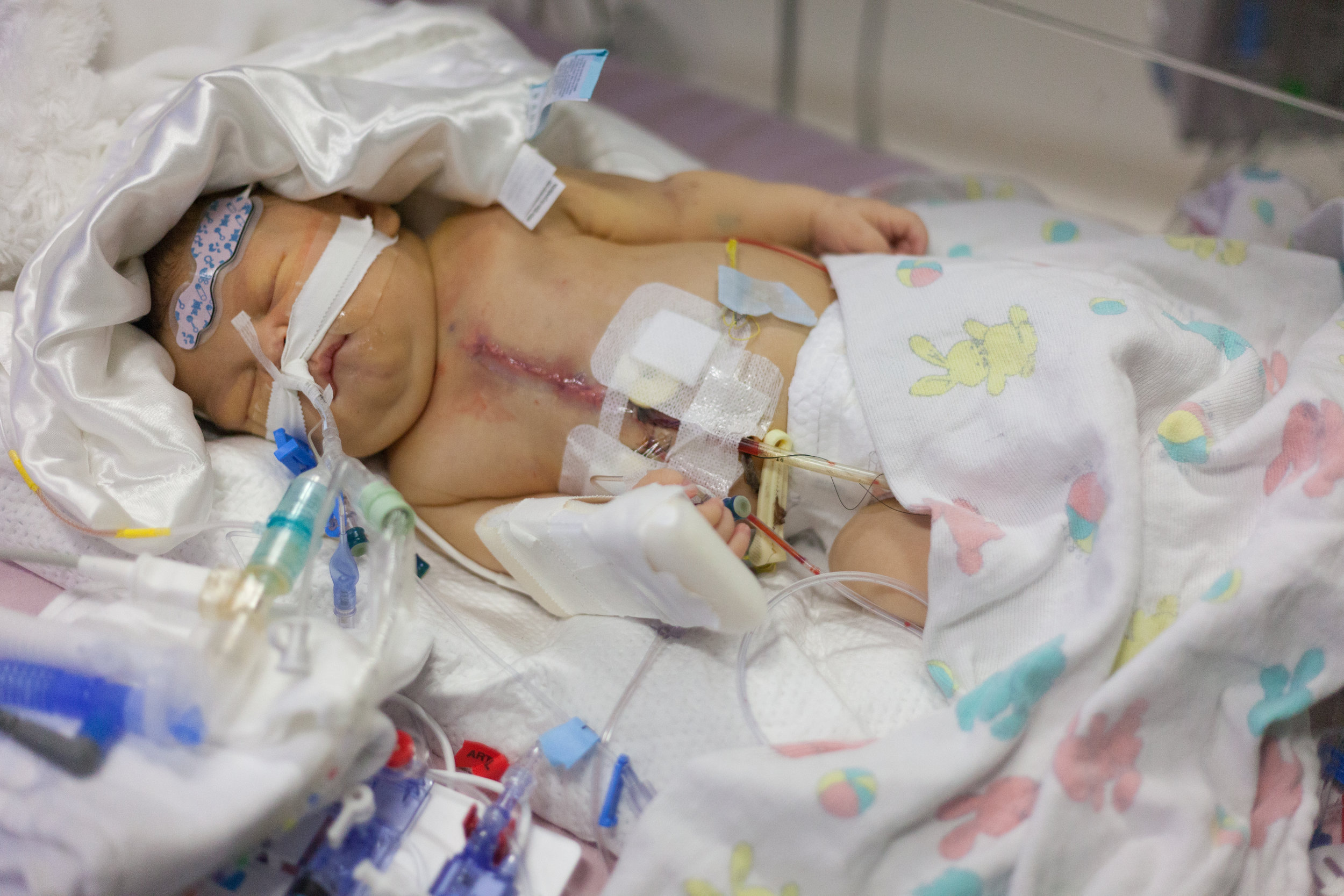
Shirley is out of surgery but not out of the woods. Surgery went well and the surgeon was very confident in his work. We had a great talk with him concerning the whole procedure. There are a lot of things that change after surgery regarding the way that her heart functions and those things can stress the heart in the early days of recovery. These are complications that they expect and anticipate. The surgeon was concerned about the anatomy of her large truncal valve. It is rather abnormal even for truncal valves and he foresees that it will need to be replaced during her next surgery (Lord willing that will be a few years). Shirley currently has an open chest and will be recovering in this state for up to five days. They leave it open in order too drain fluid, ensuring that the tissue around the heart doesn't swell. There is so much more that can be said about the specifics of her surgery but I would be writing all night.
We want to thank everyone for their prayers and ask that you continue praying for our little girl.
We aren't really holding anything back with the photos and they may be shocking but its just the reality of her current condition.
-Joseph